ICD-9-CM 079.82 MedlinePlus 007192 | ICD-10 U04 DiseasesDB 32835 eMedicine med/3662 | |
 | ||
Similar Middle East respiratory syndrome , Upper respiratory tract infection , Coronavirus | ||
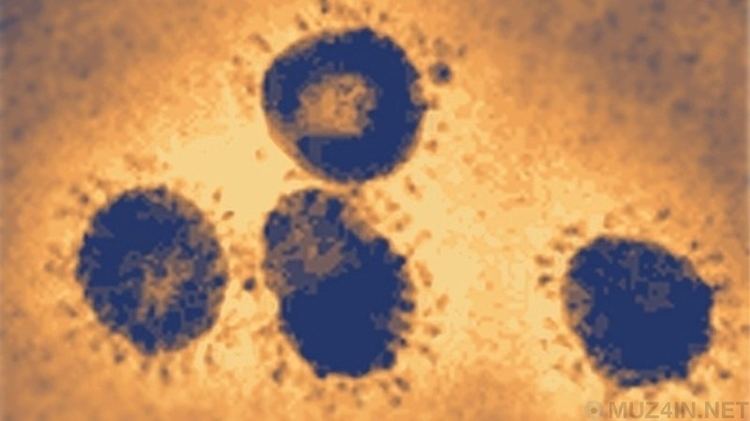
Severe acute respiratory syndrome (SARS) is a viral respiratory disease of zoonotic origin caused by the SARS coronavirus (SARS-CoV). Between November 2002 and July 2003, an outbreak of SARS in southern China caused an eventual 8,098 cases, resulting in 774 deaths reported in 37 countries, with the majority of cases in Hong Kong (9.6% fatality rate) according to the World Health Organization (WHO). No cases of SARS have been reported worldwide since 2004.
Contents
Signs and symptoms
Initial symptoms are flu-like and may include fever, myalgia, lethargy symptoms, cough, sore throat, and other nonspecific symptoms. The only symptom common to all patients appears to be a fever above 38 °C (100 °F). SARS may eventually lead to shortness of breath and/or pneumonia; either direct viral pneumonia or first bacterial pneumonia.
Diagnosis
SARS may be suspected in a patient who has:
- Contact (sexual or casual) with someone with a diagnosis of SARS within the last 10 days OR
- Travel to any of the regions identified by the World Health Organization (WHO) as areas with recent local transmission of SARS (affected regions as of 10 May 2003 were parts of China, Hong Kong, Singapore and the town of Geraldton, Ontario, Canada).
For a case to be considered probable, a chest X-ray must be positive for atypical pneumonia or respiratory distress syndrome.
The World Health Organization (WHO) has added the category of "laboratory confirmed SARS" for patients who would otherwise be considered "probable" but who have not yet had a positive chest X-ray changes, but have tested positive for SARS based on one of the approved tests (ELISA, immunofluorescence or PCR).
When it comes to the chest X-ray the appearance of SARS is not always uniform but generally appears as an abnormality with patchy infiltrates.
Prevention
There is no vaccine for SARS to date and isolation and quarantine remain the most effective means to prevent the spread of SARS. Other preventative measures include:
Treatment
Antibiotics are ineffective, as SARS is a viral disease. Treatment of SARS is largely supportive with antipyretics, supplemental oxygen and mechanical ventilation as needed.
People with SARS must be isolated, preferably in negative pressure rooms, with complete barrier nursing precautions taken for any necessary contact with these patients.
Some of the more serious damage caused by SARS may be due to the body's own immune system reacting in what is known as cytokine storm.
As of 2017, there is no cure or protective vaccine for SARS that has been shown to be both safe and effective in humans. The identification and development of novel vaccines and medicines to treat SARS is a priority for governments and public health agencies around the world. MassBiologics, a non-profit organization engaged in the discovery, development and manufacturing of biologic therapies, is cooperating with researchers at NIH and the CDC developed a monoclonal antibody therapy that demonstrated efficacy in animal models.
Prognosis
Several consequent reports from China on some recovered SARS patients showed severe long-time sequelae exist. The most typical diseases include, among other things, pulmonary fibrosis, osteoporosis, and femoral necrosis, which have led to the complete loss of working ability or even self-care ability of these cases. As a result of quarantine procedures, some of the post-SARS patients have been documented suffering from posttraumatic stress disorder (PTSD) and major depressive disorder.
Epidemiology
SARS was a relatively rare disease, with 8,273 cases as of 2003.
Outbreak in South China
The SARS epidemic appears to have started in Guangdong Province, China in November 2002 where the first case was reported that same month. The patient, a farmer from Shunde, Foshan, Guangdong, was treated in the First People's Hospital of Foshan. The patient died soon after, and no definite diagnosis was made on his cause of death. Despite taking some action to control it, Chinese government officials did not inform the World Health Organization of the outbreak until February 2003. This lack of openness caused delays in efforts to control the epidemic, resulting in criticism of the People's Republic of China from the international community. China has since officially apologized for early slowness in dealing with the SARS epidemic.
The outbreak first appeared on 27 November 2002, when Canada's Global Public Health Intelligence Network (GPHIN), an electronic warning system that is part of the World Health Organization's Global Outbreak Alert and Response Network (GOARN), picked up reports of a "flu outbreak" in China through Internet media monitoring and analysis and sent them to the WHO. While GPHIN's capability had recently been upgraded to enable Arabic, Chinese, English, French, Russian, and Spanish translation, the system was limited to English or French in presenting this information. Thus, while the first reports of an unusual outbreak were in Chinese, an English report was not generated until 21 January 2003.
Subsequent to this, the WHO requested information from Chinese authorities on 5 and 11 December. Despite the successes of the network in previous outbreak of diseases, it didn't receive intelligence until the media reports from China several months after the outbreak of SARS. Along with the second alert, WHO released the name, definition, as well as an activation of a coordinated global outbreak response network that brought sensitive attention and containment procedures (Heymann, 2003). By the time the WHO took action, over 500 deaths and an additional 2,000 cases had already occurred worldwide.
In early April, after Jiang Yanyong pushed to report the danger to China, there appeared to be a change in official policy when SARS began to receive a much greater prominence in the official media. Some have directly attributed this to the death of American James Earl Salisbury. It was around this same time that Jiang Yanyong made accusations regarding the undercounting of cases in Beijing military hospitals. After intense pressure, Chinese officials allowed international officials to investigate the situation there. This revealed problems plaguing the aging mainland Chinese healthcare system, including increasing decentralization, red tape, and inadequate communication.
Many healthcare workers in the affected nations risked and lost their lives by treating patients and trying to contain the infection before ways to prevent infection were known.
Spread to other countries and regions
The epidemic reached the public spotlight in February 2003, when an American businessman traveling from China became afflicted with pneumonia-like symptoms while on a flight to Singapore. The plane stopped in Hanoi, Vietnam, where the victim died in The French Hospital of Hanoi. Several of the medical staff who treated him soon developed the same disease despite basic hospital procedures. Italian doctor Carlo Urbani identified the threat and communicated it to WHO and the Vietnamese government; he later succumbed to the disease.
The severity of the symptoms and the infection among hospital staff alarmed global health authorities, who were fearful of another emergent pneumonia epidemic. On 12 March 2003, the WHO issued a global alert, followed by a health alert by the United States Centers for Disease Control and Prevention (CDC). Local transmission of SARS took place in Toronto, Ottawa, San Francisco, Ulaanbaatar, Manila, Singapore, Taiwan, Hanoi and Hong Kong whereas within China it spread to Guangdong, Jilin, Hebei, Hubei, Shaanxi, Jiangsu, Shanxi, Tianjin, and Inner Mongolia.
Hong Kong
In Hong Kong, the first cohort of affected people were discharged from the hospital on 29 March 2003. The disease spread in Hong Kong from a mainland doctor who arrived in February and stayed on the ninth floor of the Metropole Hotel in Kowloon, infecting 16 of the hotel visitors. Those visitors traveled to Canada, Singapore, Taiwan, and Vietnam, spreading SARS to those locations.
Another larger cluster of cases in Hong Kong centred on the Amoy Gardens housing estate. Its spread is suspected to have been facilitated by defects in its drainage system. Concerned citizens in Hong Kong worried that information was not reaching people quickly enough and created a website called sosick.org, which eventually forced the Hong Kong government to provide information related to SARS in a timely manner.
Toronto
The first case of SARS in Toronto, Canada was identified on February 23, 2003. Beginning with a woman returning from a trip to Hong Kong, the virus eventually infected 257 individuals in the province of Ontario. The trajectory of this outbreak is typically divided into two phases, with the second major wave of cases clustered around accidental exposure among patients, visitors, and staff within a major Toronto hospital. The WHO officially removed Toronto from its list of infected areas by the end of June, 2003.
The Canadian State’s official response has been widely criticized in the years following the outbreak. Brian Schwartz, vice-chair of the Ontario's SARS Scientific Advisory Committee, described public health officials’ preparedness and emergency response at the time of the outbreak as “very, very basic and minimal at best”. Critics of the response often cite poorly outlined and enforced protocol for protecting healthcare workers and identifying infected patients as a major contributing factor to the continued spread of the virus. The atmosphere of fear and uncertainty surrounding the outbreak resulted in staffing issues in area hospitals when healthcare workers elected to resign rather than risk exposure to SARS.
Identification of virus
The CDC and Canada's National Microbiology Laboratory identified the SARS genome in April 2003. Scientists at Erasmus University in Rotterdam, the Netherlands demonstrated that the SARS coronavirus fulfilled Koch's postulates thereby confirming it as the causative agent. In the experiments, macaques infected with the virus developed the same symptoms as human SARS victims.
In late May 2003, studies were conducted using samples of wild animals sold as food in the local market in Guangdong, China. The results found that the SARS coronavirus could be isolated from masked palm civets (Paguma sp.), even if the animals did not show clinical signs of the virus. The preliminary conclusion was the SARS virus crossed the xenographic barrier from asian palm civet to humans, and more than 10,000 masked palm civets were killed in Guangdong Province. The virus was also later found in raccoon dogs (Nyctereuteus sp.), ferret badgers (Melogale spp.), and domestic cats. In 2005, two studies identified a number of SARS-like coronaviruses in Chinese bats. Phylogenetic analysis of these viruses indicated a high probability that SARS coronavirus originated in bats and spread to humans either directly or through animals held in Chinese markets. The bats did not show any visible signs of disease, but are the likely natural reservoirs of SARS-like coronaviruses. In late 2006, scientists from the Chinese Centre for Disease Control and Prevention of Hong Kong University and the Guangzhou Centre for Disease Control and Prevention established a genetic link between the SARS coronavirus appearing in civets and humans, bearing out claims that the disease had jumped across species.
Containment
The World Health Organization declared severe acute respiratory syndrome contained on 9 July 2003. In the following years, four of SARS cases were reported in China between December 2003 and January 2004. There were also three separate laboratory accidents that resulted in infection. In one of these cases, an ill lab worker spread the virus to several other people. The precise coronavirus that caused SARS is believed to be gone, or at least contained to BSL-4 laboratories for research.
Community response
Fear of contracting the virus from consuming infected wild animals resulted in public bans and reduced business for meat markets throughout southern China and Hong Kong. In China, Cantonese foodways, which often incorporate a wide range of meat sources, were frequently indicted as an important contributing factor to the origins of the SARS outbreak.
Toronto’s Asian minority population faced increased discrimination over the course of the city’s outbreak. Local advocacy groups reported Asians being passed over by real-estate agents and taxi drivers and shunned on public transportation. In Boston and New York City, rumors and April Fools pranks gone awry resulted in an atmosphere of fear and substantial economic loss in the cities’ Chinatowns.
