ICD-9-CM 701.0 710.1 | ICD-10 L94.0-L94.1, M34 MedlinePlus 000429 | |
 | ||
Similar Scleroderma polyrhizum, Scleroderma areolatum, Scleroderma cepa | ||
Scleroderma is a long term autoimmune disease that results in hardening of the skin. In the more severe form, it also affects internal organs. The cause is unknown. The underlying mechanism involves the body's immune system attacking healthy tissues. There is a strong association with certain mutations in HLA genes. Environmental factors have also been implicated.
Contents
- Signs and symptoms
- Cause
- Pathophysiology
- Diagnosis
- Differential
- Classification
- Treatment
- Prognosis
- Epidemiology
- Pregnancy
- References
There are two main types of the disease: the localized form (called localized scleroderma, limited scleroderma, or morphea) and the systemic form (called Systemic scleroderma, diffuse scleroderma, generalized scleroderma, or systemic sclerosis). Limited scleroderma involves mainly the skin of the hands, arms and face. Diffuse scleroderma is rapidly progressing and affects a large area of the skin and one or more internal organs, frequently the kidneys, esophagus, heart and/or lungs. This form of scleroderma can be quite disabling. A limited cutaneous subtype of it is called CREST syndrome.
There are no treatments for scleroderma itself, but organ system–specific complications are treated. Outcomes are generally good for limited scleroderma of the skin when there are no lung complications. They are worse for those with the diffuse skin disease, particularly in older age and males. Death occurs most often from lung, heart and kidney complications. In diffuse cutaneous disease, five-year survival is 70% and 10-year survival is 55%. Scleroderma was first described in 1753 by Carlo Curzio of Ospedale degli Incurabili, Naples.
Signs and symptoms
Potential signs and symptoms include:
Cause
Scleroderma is caused by genetic and environmental factors. Mutations in HLA genes seem to play a crucial role in the pathogenesis of some cases (but not all), likewise silica, aromatic and chlorinated solvents, ketones, trichloroethylene, welding fumes and white spirits exposure seems to contribute to the condition in a small proportion of affected persons.
Pathophysiology
It is characterised by increased synthesis of collagen (leading to the sclerosis), damage to small blood vessels, activation of T lymphocytes and production of altered connective tissues. Its proposed pathogenesis is the following:
Vitamin D is implicated in the pathophysiology of the disease. An inverse correlation between plasma levels of vitamin D and scleroderma severity has been noted and vitamin D is known to play a crucial role in regulating (usually suppressing) the actions of the immune system.
Diagnosis
Typical scleroderma is classically defined as symmetrical skin thickening, with about 70% of cases also presenting with Raynaud's phenomenon, nail-fold capillary changes and antinuclear antibodies. Affected individuals may or may not experience systemic organ involvement. There is no single test for scleroderma that works all of the time and hence the diagnosis is often a matter of exclusion. Atypical scleroderma may show any variation of these changes without skin changes or with finger swelling only.
Laboratory testing can show antitopoisomerase antibodies, like anti-scl70 (causing a diffuse systemic form), or anticentromere antibodies (causing a limited systemic form and the CREST syndrome). Other autoantibodies can be seen, such as anti-U3 or anti-RNA polymerase.
Differential
Diseases that are often in the differential include:
Classification
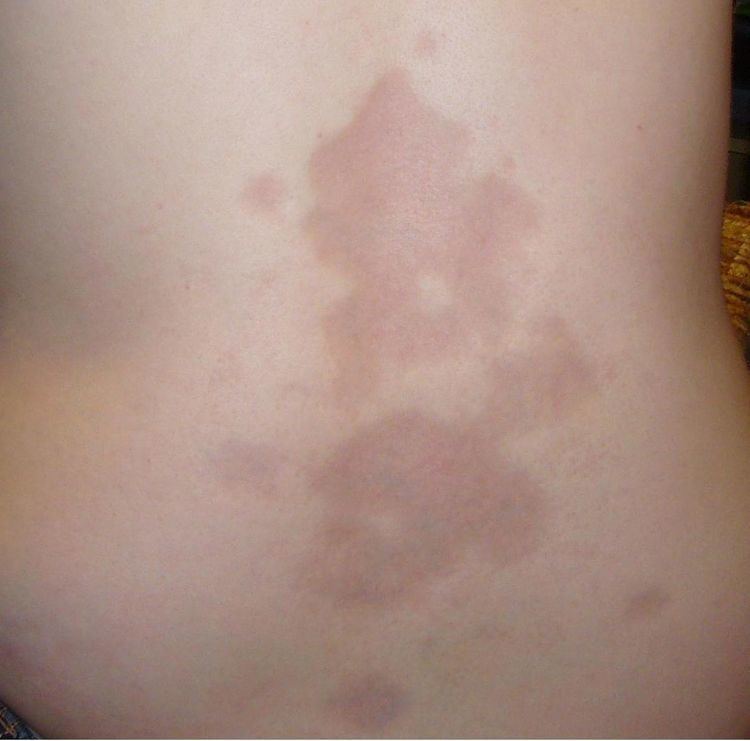
Scleroderma is characterised by the appearance of circumscribed or diffuse, hard, smooth, ivory-colored areas that are immobile and which give the appearance of hidebound skin, a disease occurring in both localised and systemic forms:
Treatment
There is no cure for scleroderma, although relief of symptoms is often achieved. These include
Systemic disease-modifying treatment with immunosuppressants is often used. Immunosuppressants used in its treatment include azathioprine, methotrexate, cyclophosphamide, mycophenolate, intravenous immunoglobulin, rituximab, sirolimus, alefacept and the Tyrosine kinase inhibitors, imatinib, nilotinib and dasatinib.
Experimental therapies under investigation include endothelin receptor antagonsits, tyrosine kinase inhibitors, beta-glycan peptides, halofuginone, basiliximab, alemtuzumab, abatacept and haematopoietic stem cell transplantation.
Prognosis
The 5-year survival rate for scleroderma is about 85%, whereas the 10-year survival rate is less than 70%. This varies according to the subtype; for instance, persons with limited skin disease have a 10-year survival rate of 71%, whereas the outlook for patients with systemic scleroderma has generally improved over the years. Ten-year survival rates rose from 54% in 1972 to 66% in 2001 The major causes of death in persons with scleroderma are: pulmonary hypertension, pulmonary fibrosis and scleroderma renal crisis. People with scleroderma are also at a heightened risk for contracting cancers (especially liver, lung, haematologic and bladder cancers) and, perhaps, cardiovascular disease.
Epidemiology
Scleroderma most commonly first presents between the ages of 20 and 50 years, although any age group can be affected. Women are four to nine times more likely to develop scleroderma than men.
This disease is found worldwide. In the United States, prevalence is estimated at 240 per million and the annual incidence of scleroderma is 19 per million people. Likewise in the United States, it is slightly more common in African Americans than in their white counterparts, Scleroderma occurs much more often in women than it does in men. Choctaw Native Americans are more likely than Americans of European descent to develop the type of scleroderma that affects internal organs. In Germany, the prevalence is between 10 and 150 per million people, and the annual incidence is between 3 and 28 per million people. In South Australia, the annual incidence is 23 per million people, and the prevalence 233 per million people. Scleroderma is less common in the Asian population.
Pregnancy
Scleroderma in pregnancy is a complex situation; it increases the risk to both mother and child. Overall scleroderma is associated with reduced fetal weight for gestational age. The treatment for scleroderma often includes known teratogens such as cyclophosphamide, methotrexate, mycophenolate, etc. and hence careful avoidance of such drugs during pregnancy is advised. In these cases hydroxychloroquine and low-dose corticosteroids might be used for disease control.
