Precursor Ectoderm Latin Glandula sudorifera TA A16.0.00.029 | System Integumentary MeSH A10.336.899 | |
 | ||
Nerve Eccrine: cholinergic sympathetic nervesApocrine: adrenergic nerves | ||
Sweat glands, also known as sudoriferous or sudoriparous glands, from Latin sudor, meaning 'sweat', are small tubular structures of the skin that produce sweat. Sweat glands are a type of exocrine gland, which are glands that produce and secrete substances onto an epithelial surface by way of a duct. There are two main types of sweat glands that differ in their structure, function, secretory product, mechanism of excretion, anatomic distribution, and distribution across species:
Contents
- Structure
- Distribution
- Animals
- Apocrine
- Eccrine
- Apoeccrine
- Others
- Sweat
- Mechanism
- Thermal
- Emotional
- Gustatory
- Antiperspirant
- Pathology
- Tumors
- As signs in other illnesses
- References
Ceruminous glands (which produce ear wax), mammary glands (which produce milk), and ciliary glands in the eyelids are modified apocrine sweat glands.
Structure
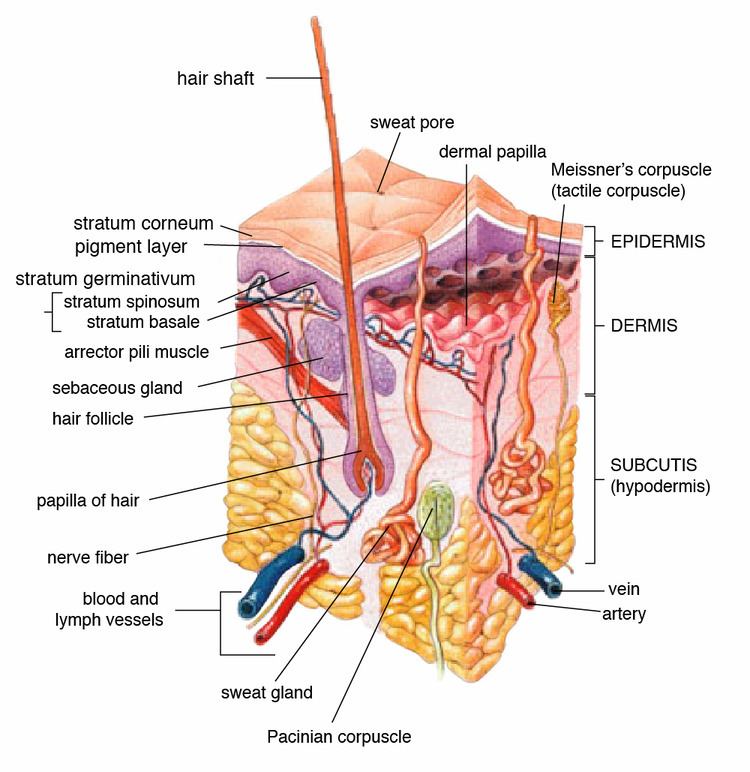
Generally, sweat glands consist of a secretory unit consisting of a base rolled into a glomerulum, and a duct that carries the sweat away. The secretory coil or base, is set deep in the lower dermis and hypodermis, and the entire gland is surrounded by adipose tissue. In both sweat gland types, the secretory coils are surrounded by contractile myoepithelial cells that function to facilitate excretion of secretory product. The secretory activities of the gland cells and the contractions of myoepithelial cells are controlled by both the autonomic nervous system and by the circulating hormones. The distal or apical part of the duct that opens to the skin's surface is known as the acrosyringium.
Each sweat gland receives several nerve fibers that branch out into bands of one or more axons and encircle the individual tubules of the secretory coil. Capillaries are also interwoven among sweat tubules.
Distribution
The number of active sweat glands varies greatly among different people, though comparisons between different areas (ex. axillae vs. groin) show the same directional changes (certain areas always have more active sweat glands while others always have fewer). According to Henry Gray's estimates, the palm has around 370 sweat glands per cm2; the back of the hand has 200 per cm2; the forehead has 175 per cm2; the breast, abdomen, and forearm have 155 per cm2; and the back and legs have 60–80 per cm2.
In the finger pads, sweat glands are somewhat irregularly spaced on the epidermal ridges. There are no pores between the ridges, though sweat tends to spill into them. The thick epidermis of the palms and soles causes the sweat glands to become spirally coiled.
Animals
Non-primate mammals have eccrine sweat glands only on the palms and soles. Apocrine glands cover the rest of the body, though they are not as effective as humans' in temperature regulation (with the exception of horses'). Prosimians have a 1:20 ratio of follicles with apocrine glands versus follicles without. They have eccrine glands between hairs over most of their body (while humans have them between the hairs on their scalp).
The overall distribution of sweat glands varies among primates: the rhesus and patas monkeys have them on the chest; the squirrel monkey has them only on the palms and soles; and the stump-tailed macaque, Japanese monkey, and baboon have them over the entire body.
Domestic animals have apocrine glands at the base of each hair follicle, but eccrine glands only in foot pads and snout. Their apocrine glands, like those in humans, produce an odorless oily milky secretion evolved not to evaporate and cool but rather coat and stick to hair so odor-causing bacteria can grow on it. Eccrine glands on their foot pads, like those on palms and soles of humans, did not evolve to cool either but rather increase friction and enhance grip.
Dogs and cats have apocrine glands that are specialized in both structure and function located at the eyelids (Moll's glands), ears (ceruminous glands), anal sac, prepuce vulva, and circumanal area.
Apocrine
Apocrine sweat glands are found in the armpit, areola (around the nipples), perineum (between the anus and genitals), in the ear, and in the eyelids. The secretory portion is larger than that of eccrine glands (making them larger overall). Rather than opening directly onto the surface of the skin, apocrine glands secrete sweat into the pilary canal of the hair follicle.
Before puberty, the apocrine sweat glands are inactive; hormonal changes in puberty cause the glands to increase in size and begin functioning. The substance secreted is thicker than eccrine sweat and provides nutrients for bacteria on the skin: the bacteria's decomposition of sweat is what creates the acrid odor. Apocrine sweat glands are most active in times of stress and sexual excitement.
In mammals (including humans), apocrine sweat contains pheromone-like compounds to attract other organisms within their species. Study of human sweat has revealed differences between men and women in apocrine secretions and bacteria.
Eccrine
Eccrine sweat glands are everywhere except the lips, ear canal, prepuce, glans penis, labia minora, and clitoris. They are ten times smaller than apocrine sweat glands, do not extend as deeply into the dermis, and excrete directly onto the surface of the skin. The proportion of eccrine glands decreases with age.
The clear secretion produced by eccrine sweat glands is termed sweat or sensible perspiration. Sweat is mostly water, but it does contain some electrolytes, since it is derived from blood plasma. The presence of sodium chloride gives sweat a salty taste.
The total volume of sweat produced depends on the number of functional glands and the size of the surface opening. The degree of secretory activity is regulated by neural and hormonal mechanisms (men sweat more than women). When all of the eccrine sweat glands are working at maximum capacity, the rate of perspiration for a human being may exceed three liters per hour, and dangerous losses of fluids and electrolytes can occur.
Eccrine glands have three primary functions:
Apoeccrine
Some human sweat glands cannot be classified as either apocrine or eccrine, having characteristics of both; such glands are termed apoeccrine. They are larger than eccrine glands, but smaller than apocrine ones; their secretory portion has a narrow portion similar to secretory coils in eccrine glands as well as a wide section reminiscent of apocrine glands.
Apoeccrine, found in the armpits and perianal region, have ducts opening onto the skin surface. They are presumed to have developed in puberty from the eccrine glands, and can comprise up to 50% of all axillary glands. Apoeccrine glands secrete more sweat than both eccrine and apocrine glands, thus playing a large role in axillary sweating. Apoeccrine glands are sensitive to cholinergic activity, though they can also be activated via adrenergic stimulation. Like eccrine glands, they continuously secrete a thin, watery sweat.
Others
Specialized sweat glands, including the ceruminous glands, mammary glands, ciliary glands of the eyelids, and sweat glands of the nasal vestibulum, are modified apocrine glands. Ceruminous glands are near the ear canals, and produce cerumen (earwax) that mixes with the oil secreted from sebaceous glands. Mammary glands use apocrine secretion to produce milk.
Sweat
Sweat glands are used to regulate temperature and remove waste by secreting water, sodium salts, and nitrogenous waste (such as urea) onto the skin surface. The main electrolytes of sweat are sodium and chloride, though the amount is small enough to make sweat hypotonic at the skin surface. Eccrine sweat is clear, odorless, and is composed of 98–99% water; it also contains NaCl, fatty acids, lactic acid, citric acid, ascorbic acid, urea, and uric acid. Its pH ranges from 4 to 6.8. On the other hand, the apocrine sweat has a pH of 6 to 7.5; it contains water, proteins, carbohydrate waste material, lipids, and steroids. The sweat is oily, cloudy, viscous, and originally odorless; it gains odor upon decomposition by bacteria. Because both apocrine glands and sebaceous glands open into the hair follicle, apocrine sweat is mixed with sebum.
Mechanism
It was originally thought that both apocrine and eccrine sweat glands used merocrine secretion, where vesicles in the gland released sweat via exocytosis, leaving the entire cell intact. More recent studies have revealed that apocrine glands release sweat in the hair follicle via apocrine secretion, where portions of the cell are actually pinched off, and disintegrate later to excrete sweat.
In both apocrine and eccrine sweat glands, the sweat is originally produced in the gland's coil, where it is isotonic with the blood plasma there. When the rate of sweating is low, salt is conserved and reabsorbed by the gland's duct; high sweat rates, on the other hand, lead to less salt reabsorption and allow more water to evaporate on the skin (via osmosis) to increase evaporative cooling.
Secretion of sweat occurs when the myoepithelial cell cells surrounding the secretory glands contract. Eccrine sweat increases the rate of bacterial growth and volatilizes the odor compounds of apocrine sweat, strengthening the latter's acrid smell.
Normally, only a certain number of sweat glands are actively producing sweat. When stimuli call for more sweating, more sweat glands are activated, with each then producing more sweat.
Thermal
Both eccrine and apocrine sweat glands participate in thermal (thermoregulatory) sweating, which is directly controlled by the hypothalamus. Thermal sweating is stimulated by a combination of internal body temperature and mean skin temperature. In eccrine sweat glands, stimulation occurs via activation by acetylcholine, which binds to the gland's muscarinic receptors.
Emotional
Emotional sweating is stimulated by stress, anxiety, fear, and pain; it is independent of ambient temperature. Acetylcholine acts on the eccrine glands and adrenaline acts on both eccrine and apocrine glands to produce sweat. Emotional sweating can occur anywhere, though it is most evident on the palms, soles of the feet, and axillary regions. Sweating on the palms and soles is thought to have evolved as a fleeing reaction in mammals: it increases friction and prevents slipping when running or climbing in stressful situations.
Gustatory
Gustatory sweating refers to thermal sweating induced by the ingestion of food. The increase in metabolism caused by ingestion raises body temperature, leading to thermal sweating. Hot and spicy foods also leads to mild gustatory sweating in the face, scalp and neck: capsaicin (the compound that makes spicy food taste "hot"), binds to receptors in the mouth that detect warmth. The increased stimulation of such receptors induces a thermoregulatory response.
Antiperspirant
Unlike deodorant, which simply reduces axillary odor without affecting body functions, antiperspirant reduces both eccrine and apocrine sweating. Antiperspirants, which are classified as drugs, cause proteins to precipitate and mechanically block eccrine (and sometimes apocrine) sweat ducts. The metal salts found in antiperspirants alters the keratin fibrils in the ducts; the ducts then close and form a "horny plug". The main active ingredients in modern antiperspirants are aluminum chloride, aluminum chlorohydrate, aluminum zirconium chlorohydrate, and buffered aluminum sulfate.
On apocrine glands, antiperspirants also contain antibacterial agents such as trichlorocarbanilide, hexamethylene tetramine, and zinc ricinoleate. The salts are dissolved in ethanol and mixed with essential oils high in eugenol and thymol (such as thyme and clove oils). Antiperspirants may also contain levomethamphetamine
Pathology
Diseases of the sweat glands include:
Tumors
Sweat gland tumors include:
Adenolipomas are lipomas associated with eccrine sweat glands.
As signs in other illnesses
Many diseases cause sweat gland dysfunction:
