ICD-10 A83-A86, B94.1, G05 DiseasesDB 22543 eMedicine emerg/163 | ICD-9-CM 323 MedlinePlus 001415 | |
 | ||
Specialty Neurology, infectious disease | ||
Encephalitis is a sudden onset inflammation of the brain. Encephalitis with meningitis is known as meningoencephalitis. Symptoms include headache, fever, confusion, drowsiness, and fatigue. Further symptoms include seizures or convulsions, tremors, hallucinations, stroke, and memory problems. In 2013, encephalitis was estimated to have resulted in 77,000 deaths worldwide, down from 92,000 in 1990. The word is from Ancient Greek ἐνκέφαλος, enképhalos "brain", composed of ἐν, en, "in" and κεφαλή, kephalé, "head", and the medical suffix -itis "inflammation".
Contents
Signs and symptoms
Adult patients with encephalitis present with acute onset of fever, headache, confusion, and sometimes seizures. Younger children or infants may present irritability, poor appetite and fever. Neurological examinations usually reveal a drowsy or confused patient. Stiff neck, due to the irritation of the meninges covering the brain, indicates that the patient has either meningitis or meningoencephalitis.
Viral
Viral encephalitis can occur either as a direct effect of an acute infection, or as one of the sequelae of a latent infection. The most common causes of acute viral encephalitis are rabies virus, HSV infection, poliovirus, and measles virus.
Other possible viral causes are arbovirus (St. Louis encephalitis, West Nile encephalitis virus), bunyavirus (La Crosse strain), arenavirus (lymphocytic choriomeningitis virus) and reovirus (Colorado tick virus)
Bacterial and other
It can be caused by a bacterial infection, such as bacterial meningitis, or may be a complication of a current infectious disease syphilis (secondary encephalitis).
Certain parasitic or protozoal infestations, such as toxoplasmosis, malaria, or primary amoebic meningoencephalitis, can also cause encephalitis in people with compromised immune systems. Lyme disease and/or Bartonella henselae may also cause encephalitis.
Other bacterial pathogens, like Mycoplasma and those causing rickettsial disease, cause inflammation of the meninges and consequently encephalitis. A non-infectious cause includes acute disseminated encephalitis which is demyelinated.
Limbic encephalitis
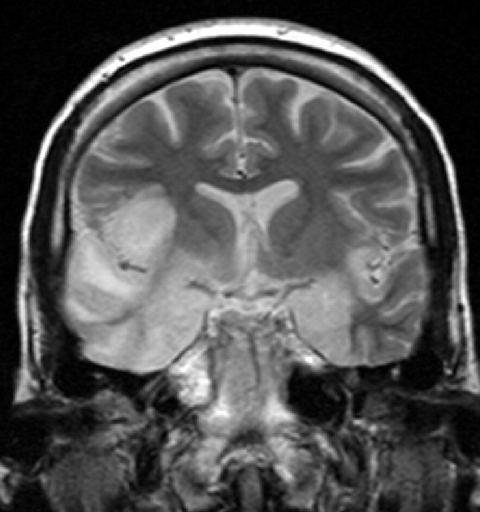
Limbic encephalitis refers to inflammatory disease confined to the limbic system of the brain. The clinical presentation often includes disorientation, disinhibition, memory loss, seizures, and behavioral anomalies. MRI imaging reveals T2 hyperintensity in the structures of the medial temporal lobes, and in some cases, other limbic structures. Some cases of limbic encephalitis are of autoimmune origin.
Autoimmune encephalitis
Autoimmune encephalitis signs can include catatonia, psychosis, abnormal movements, and autonomic dysregulation. Antibody-mediated anti-N-methyl-D-aspartate-receptor encephalitis and Rasmussen encephalitis are examples of autoimmune encephalitis.
Encephalitis lethargica
Encephalitis lethargica is identified by high fever, headache, delayed physical response, and lethargy. Individuals can exhibit upper body weakness, muscular pains, and tremors, though the cause of encephalitis lethargica is not currently known. From 1917 to 1928, an epidemic of encephalitis lethargica occurred worldwide.
Diagnosis
Diagnosing encephalitis is done via a variety of tests:
Treatment
Treatment (which is based on supportive care) is as follows:
Prevention
Vaccination is available against tick-borne and Japanese encephalitis and should be considered for at-risk individuals. Post-infectious encephalomyelitis complicating smallpox vaccination is avoidable, for all intents and purposes, as smallpox is nearly eradicated. Contraindication to Pertussis immunization should be observed in patients with encephalitis.
Epidemiology
The number of new cases a year of acute encephalitis in Western countries is 7.4 cases per 100,000 population per year. In tropical countries, the incidence is 6.34 per 100,000 per year. In 2013, encephalitis was estimated to have resulted in 77,000 deaths, down from 92,000 in 1990. Herpes simplex encephalitis has an incidence of 2–4 per million population per year.
