Specialty obstetrics ICD-9-CM 641.2 MedlinePlus 000901 | ICD-10 O45 DiseasesDB 40 eMedicine med/6 emerg/12 | |
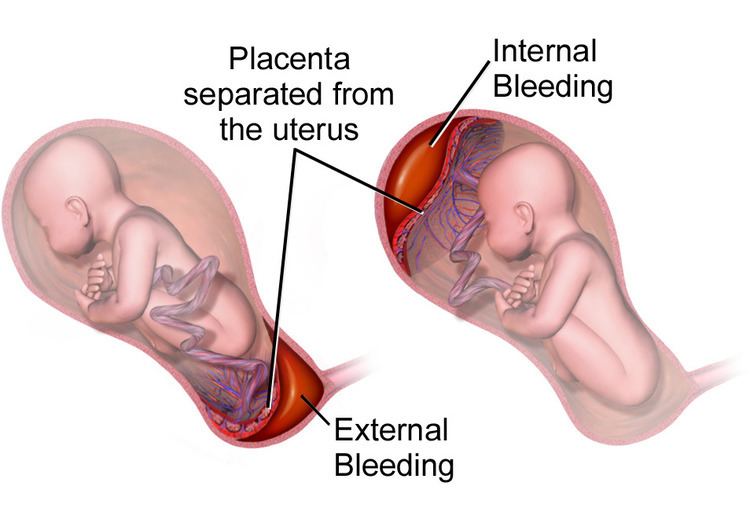 | ||
Placental abruption, also known as abruptio placentae, is a complication of pregnancy, wherein the placental lining separates from the uterus of the mother prior to delivery. The effects on the mother depend primarily on the severity of the abruption, while the effects on the baby depend on both its severity and the gestational age at which it occurs. The heart rate of the baby is associated with the severity.
Contents
- Signs and symptoms
- Risk factors
- Pathophysiology
- Diagnosis
- Classification
- Prevention
- Management
- Prognosis
- Mother
- Baby
- Epidemiology
- References
Early medical intervention is needed to ensure a good outcome, and this is not available in many parts of the world. Treatment depends on how serious the abruption is and how far along the woman is in her pregnancy.
It is the most common pathological cause of late pregnancy bleeding. In humans, it refers to the abnormal separation after 20 weeks of gestation and prior to birth. It occurs on average in 0.5%, or 1 in 200, deliveries. Placental abruption is a significant contributor to maternal mortality worldwide.
Signs and symptoms
In the early stages of placental abruption, there may be no symptoms. When symptoms develop, they tend to develop suddenly. Common symptoms include sudden-onset abdominal pain, contractions that seem continuous and do not stop, pain in the abdomen and back, vaginal bleeding, enlarged uterus disproportionate to the gestational age of the fetus, decreased fetal movement, and decreased fetal heart rate.
A placental abruption caused by arterial bleeding at the center of the placenta leads to sudden development of severe symptoms and life-threatening conditions including fetal heart rate abnormalities, severe maternal hemorrhage, and disseminated intravascular coagulation. Those abruptions caused by venous bleeding at the periphery of the placenta develop more slowly and cause small amounts of bleeding, intrauterine growth restriction, and oligohydramnios (low levels of amniotic fluid).
Risk factors
Risk factors for placental abruption include disease, trauma, history, anatomy, and exposure to substances. The risk of placental abruption increases sixfold after severe maternal trauma. Anatomical risk factors include uncommon uterine anatomy (e.g. bicornuate uterus), uterine synechiae, and leiomyoma. Substances that increase risk of placental abruption include cocaine and tobacco when consumed during pregnancy, especially the third trimester. History of placental abruption or previous Caesarian section increases the risk by a factor of 2.3.
Pathophysiology
In the vast majority of cases, placental abruption is caused by the maternal vessels tearing away from the decidua basalis, not the fetal vessels. The underlying cause is often unknown. A small number of abruptions are caused by trauma that stretches the uterus. Because the placenta is less elastic than the uterus, it tears away when the uterine tissue stretches suddenly. When anatomical risk factors are present, the placenta does not attach in a place that provides adequate support, and it may not develop appropriately or be separated as it grows. Cocaine use during the third trimester has a 10% chance of causing abruption. Though the exact mechanism is not known, cocaine and tobacco cause systemic vasoconstriction, which can severely restrict the placental blood supply (hypoperfusion and ischemia), or otherwise disrupt the vasculature of the placenta, causing tissue necrosis, bleeding, and therefore abruption.
In most cases, placental disease and abnormalities of the spiral arteries develop throughout the pregnancy and lead to necrosis, inflammation, vascular problems, and ultimately, abruption. Because of this, most abruptions are caused by bleeding from the arterial supply, not the venous supply. Production of thrombin via massive bleeding causes the uterus to contract and leads to DIC.
The accumulating blood pushes between the layers of the decidua, pushing the uterine wall and placenta apart. When the placenta is separated, it is unable to exchange waste, nutrients, and oxygen, a necessary function for the fetus's survival. The fetus dies when it no longer receives enough oxygen and nutrients to survive.
Diagnosis
Placental abruption is suspected when a pregnant mother has sudden localized abdominal pain with or without bleeding. The fundus may be monitored because a rising fundus can indicate bleeding. An ultrasound may be used to rule out placenta praevia but is not diagnostic for abruption. The diagnosis is one of exclusion, meaning other possible sources of vaginal bleeding or abdominal pain have to be ruled out in order to diagnose placental abruption. Of note, use of magnetic resonance imaging has been found to be highly sensitive in depicting placental abruption, and may be considered if no ultrasound evidence of placental abruption is present, especially if the diagnosis of placental abruption would change management.
Classification
Based on severity:
Prevention
Although the risk of placental abruption cannot be eliminated, it can be reduced. Avoiding tobacco, alcohol and cocaine during pregnancy decreases the risk. Staying away from activities which have a high risk of physical trauma is also important. Women who have high blood pressure or who have had a previous placental abruption and want to conceive must be closely supervised by a doctor.
The risk of placental abruption can be reduced by maintaining a good diet including taking folic acid, regular sleep patterns and correction of pregnancy-induced hypertension.
It is crucial for women to be made aware of the signs of placental abruption, such as vaginal bleeding, and that if they experience such symptoms they must get into contact with their health care provider/the hospital without any delay.
Management
Treatment depends on the amount of blood loss and the status of the fetus. If the fetus is less than 36 weeks and neither mother or fetus is in any distress, then they may simply be monitored in hospital until a change in condition or fetal maturity whichever comes first.
Immediate delivery of the fetus may be indicated if the fetus is mature or if the fetus or mother is in distress. Blood volume replacement to maintain blood pressure and blood plasma replacement to maintain fibrinogen levels may be needed. Vaginal birth is usually preferred over caesarean section unless there is fetal distress. Caesarean section is contraindicated in cases of disseminated intravascular coagulation. Patient should be monitored for 7 days for PPH. Excessive bleeding from uterus may necessitate hysterectomy. The mother may be given Rhogam if she is Rh negative.
Prognosis
The prognosis of this complication depends on whether treatment is received by the patient, on the quality of treatment, and on the severity of the abruption. Outcomes for the baby also depend on the gestational age.
In the Western world, maternal deaths due to placental abruption are rare. The fetal prognosis is worse than the maternal prognosis; approximately 12% of fetuses affected by placental abruption die. 77% of fetuses that die from placental abruption die before birth; the remainder die due to complications of preterm birth.
Without any form of medical intervention, as often happens in many parts of the world, placental abruption has a high maternal mortality rate.
Mother
Baby
Epidemiology
Placental abruption occurs in approximately 0.2%-1% of all pregnancies. Though different causes change when abruption is most likely to occur, the majority of placental abruptions occur before 37 weeks gestation, and 14% occur before 32 weeks gestation.
