ICD-9-CM 697.0 MedlinePlus 000867 | ICD-10 L43 DiseasesDB 7452 eMedicine derm/233 derm/663 | |
 | ||
Lichen planus (LP) is an uncommon disease of the skin with a prevalence of 0.1% in men and 0.3% in women. The cause is unknown, but it is thought to be the result of an autoimmune process with an unknown initial trigger. There is no cure, but many different medications and procedures have been used in efforts to control the symptoms.
Contents
- Classification
- Site
- Pattern
- Overlap syndromes
- Signs and symptoms
- Cutaneous lichen planus
- Mucosal lichen planus
- Oral lichen planus
- Causes
- Diagnosis
- Histopathology
- Differential diagnosis
- Treatment
- Prognosis
- Epidemiology
- History
- References
The term lichenoid reaction (or lichenoid lesion) refers to a lesion of similar or identical histopathologic and clinical appearance to lichen planus (i.e. an area which looks the same as lichen planus, both to the naked eye and under a microscope). Sometimes dental materials or certain medications can cause a lichenoid reaction. They can also occur in association with graft versus host disease.
Classification
Lichen planus (LP) is a chronic inflammatory disease of the skin, mucous membranes and nails.
Lichen planus lesions are so called because of their "lichen-like" appearance and can be classified by the site they involve, or by their morphology.
Site
Lichen planus may be categorized as affecting mucosal or cutaneous surfaces.
Pattern
Lichen planus lesions can occur in many different forms:
Overlap syndromes
Occasionally, lichen planus is known to occur with other conditions. For example:
Signs and symptoms
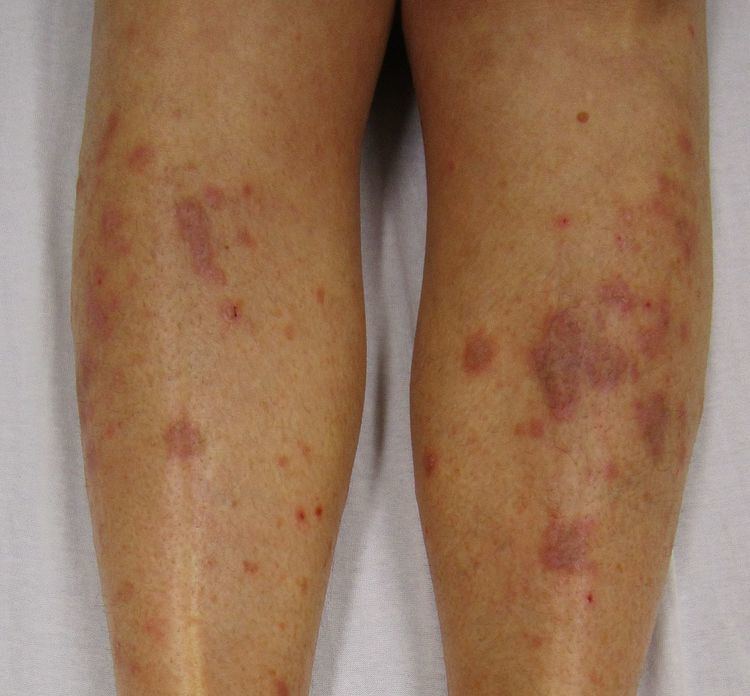
Although lichen planus can present with a variety of lesions, the most common presentation is as a well-defined area of purple-coloured, itchy, flat-topped papules with interspersed lacy white lines (Wickham's striae). This description is known as the characteristic "6 Ps" of lichen planus: planar (flat-topped), purple, polygonal, pruritic, papules, and plaques. This rash, after regressing, is likely to leave an area of hyperpigmentation that slowly fades. That said, a variety of other lesions can also occur.
Cutaneous lichen planus
Variants of cutaneous lichen planus are distinguished based upon the appearance of the lesions and/or their distribution. Lesions can affect the:
Other variants may include:
Mucosal lichen planus
Lichen planus affecting mucosal surfaces may have one lesion or be multifocal. Examples of lichen planus affecting mucosal surfaces include:
Oral lichen planus
Oral lichen planus (also termed oral mucosal lichen planus), is a form of mucosal lichen planus, where lichen planus involves the oral mucosa, the lining of the mouth. This may occur in combination with other variants of lichen planus. Six clinical forms of oral lichen planus are recognized:
These types often coexist in the same individual. Oral lichen planus tends to present bilaterally as mostly white lesions on the inner cheek, although any mucosal site in the mouth may be involved. Other sites, in decreasing order of frequency, may include the tongue, lips, gingivae, floor of the mouth, and very rarely, the palate.
Generally, oral lichen planus tends not to cause any discomfort or pain, although some people may experience soreness when eating or drinking acidic or spicy foodstuffs or beverages. When symptoms arise, they are most commonly associated with the atrophic and ulcerative subtypes. These symptoms can include a burning sensation to severe pain. Lichen planus, particularly when concomitant oral or genital lesions occur, significantly affects patients’ quality of life.
Causes
The cause of lichen planus is unknown, but it is not contagious and does not involve any known pathogen. It is thought to be a T cell mediated autoimmune reaction (where the body's immune system targets its own tissues). This autoimmune process triggers apoptosis of the epithelial cells. Several cytokines are involved in lichen planus, including tumor necrosis factor alpha, interferon gamma, interleukin-1 alpha, interleukin 6, and interleukin 8. This autoimmune, T cell mediated, process is thought to be in response to some antigenic change in the oral mucosa, but a specific antigen has not been identified.
Where a causal or triggering agent is identified, this is termed a lichenoid reaction rather than lichen planus. These may include:
It has been suggested that lichen planus may respond to stress, where lesions may present during times of stress. Lichen planus can be part of Grinspan's syndrome.
It has also been suggested that mercury exposure may contribute to lichen planus.
Diagnosis
Lichen planus lesions are diagnosed clinically by their "lichen-like" appearance. A biopsy can be used to rule out conditions that may resemble lichen planus, and can pick up any secondary malignancies.
Histopathology
Lichen planus has a unique microscopic appearance that is similar between cutaneous, mucosal and oral. A Periodic acid-Schiff stain of the biopsy may be used to visualise the specimen. Histological features seen include:
Differential diagnosis
The differential diagnosis for OLP includes:
Treatment
There is no cure for lichen planus, and so treatment of cutaneous and oral lichen planus is for symptomatic relief or due to cosmetic concerns. When medical treatment is pursued, first-line treatment typically involves corticosteroids, and removal of any triggers. Without treatment, most lesions will spontaneously resolve within 6–9 months for cutaneous lesions, and longer for mucosal lesions. Recently, it was hypothesized that the interferon gamma/CXCL10 axis could be a target to reverse inflammation.
Cutaneous lichen planus
Many different treatments have been reported for cutaneous lichen planus, however there is a general lack of evidence of efficacy for any treatment. Treatments tend to be prolonged, partially effective and disappointing. The mainstay of localized skin lesions is topical steroids. Additional treatments include retinoids such as Acitretin, or sulfosalazin. Narrow band UVB phototherapy or systemic PUVA therapy are known treatment modalities for generalized disease.
However, there is striking paucity of evidence regarding therapy, since randomized clinical trials on the medical or physical treatment of LP are lacking.
Oral lichen planus
Reassurance that the condition is benign, elimination of precipitating factors and improving oral hygiene are considered initial management for symptomatic OLP, and these measures are reported to be useful. Treatment usually involves topical corticosteroids (such as betamethasone, clobetasol, dexamethasone, and triamcinolone) and analgesics, or if these are ineffective and the condition is severe, the systemic corticosteroids may be used. Calcineurin inhibitors (such as pimecrolimus, tacrolimus or cyclosporin) are sometimes used.
Prognosis
In contrast to cutaneous lichen planus, lichen planus lesions in the mouth may persist for many years, and tend to be difficult to treat, with relapses being common. Atrophic/erosive lichen planus is associated with a small risk of malignant transformation, and so people with OLP tend to be kept on long term review to detect any potential change early. Sometimes OLP can become secondarily infected with Candida organisms.
Epidemiology
The overall prevalence of lichen planus in the general population is about 0.1–4.0%. It generally occurs more commonly in females, in a ratio of 3:2, and most cases are diagnosed between the ages of 30 and 60, but it can occur at any age.
Oral lichen planus is relatively common, It is one of the most common mucosal diseases. The prevalence in the general population is about 1.27–2.0%, and it occurs more commonly in middle aged people. OLP in children is rare. About 50% of females with oral lichen planus were reported to have undiagnosed vulvar lichen planus.
History
Lichen planus was first reported in 1869 by Erasmus Wilson.
