 | ||
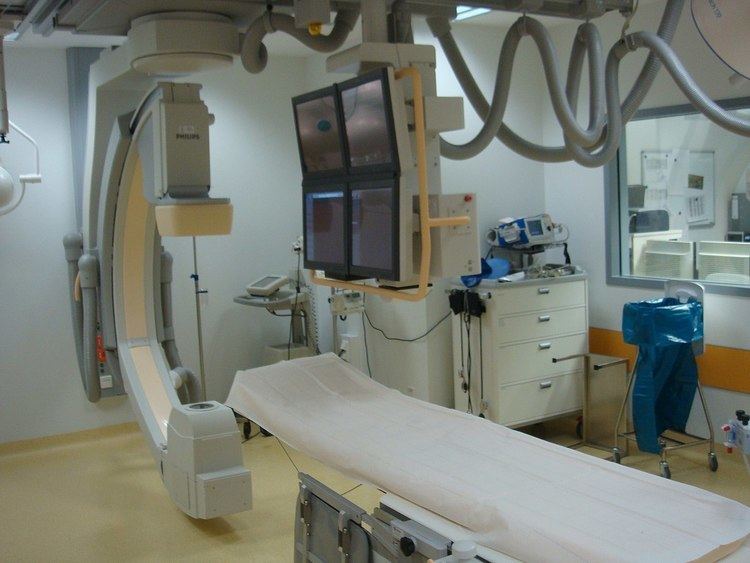
Cardiac catheterization (heart cath) is the insertion of a catheter into a chamber or vessel of the heart. This is done both for diagnostic and interventional purposes. Subsets of this technique are mainly coronary catheterization, involving the catheterization of the coronary arteries, and catheterization of cardiac chambers and valves of the cardiac system.
Contents
Procedure
"Cardiac catheterization" is a general term for a group of procedures that are performed using this method, such as coronary angiography and left ventricle angiography. Once the catheter is in place, it can be used to perform a number of procedures including, coronary angioplasty, balloon septostomy, electrophysiology study or catheter ablation.
Procedures can be diagnostic or therapeutic. For example, coronary angiography is a diagnostic procedure that allows the interventional cardiologist to visualize the coronary vessels. Percutaneous coronary intervention, however, involves the use of mechanical stents to increase blood flow to previously blocked (or occluded) vessels. Other common diagnostic procedures include measuring pressures throughout the four chambers of the heart and evaluating pressure differences across the major heart valves. Interventional cardiologists can also use cardiac catheterization to estimate the cardiac output, the amount of blood pumped by the heart per minute.
Cardiac catheterization requires the use of fluoroscopy to visualize the path of the catheter as it enters the heart or as it enters the coronary arteries. The coronary arteries are known as "epicardial vessels" as they are located in the epicardium, the outermost layer of the heart. Fluoroscopy can be conceptually described as continuous x-rays. The use of fluoroscopy requires radiopaque contrast, which in rare cases can lead to contrast-induced kidney injury (see Contrast-induced nephropathy).
There are two major categories of cardiac catheterization:
Coronary catheterization
Main page: Coronary catheterization
Indications for diagnostic use of coronary catheterization
Patients without cardiac symptoms or high-risk markers for a heart problem should not have a coronary catheterization to screen for problems.
Indications for cardiac catheterization include the following:
Right heart catheterization, along with pulmonary function testing and other testing should be done to confirm pulmonary hypertension prior to having vasoactive pharmacologic treatments approved and initiated.
Investigative techniques used with coronary catheterization
Catheterization of chambers and valves
Catheterization of cardiac chambers and valves may be performed at the same time as a coronary catheterization, and may also involve nearby major vessels, such as the aorta. It is the main method of cardiac ventriculography (another being radionuclide ventriculography, whose use has largely been replaced by echocardiography).
It has the ability to measure the pressure gradient across a valve and derive valve area from it. Thereby, it can assist in diagnosis of, for example, aortic stenosis.
This is also the procedure used in balloon septostomy, which is the widening of a foramen ovale, patent foramen ovale (PFO), or atrial septal defect (ASD) using a balloon catheter.
History
The history of cardiac catheterization dates back to Claude Bernard (1813-1878), who used it on animal models. Clinical application of cardiac catheterization begins with Werner Forssmann in the 1930s, who inserted a catheter into the vein of his own forearm, guided it fluoroscopically into his right atrium, and took an X-ray picture of it. Forssmann won the Nobel Prize in Physiology or Medicine for this achievement, though hospital administrators removed him from his position owing to his unorthodox methods. During World War II, André Frédéric Cournand, a professor at Columbia University College of Physicians and Surgeons who also shared the Nobel Prize, and his colleagues developed techniques for left and right heart catheterization.
Dr. Eugene A. Stead, founder of the Physician Assistant profession, also performed research in the 1940s which paved the way for cardiac catheterization in medicine today.
