ICD-9-CM 70.64, 70.62, 70.64, 70.94, 70.6, 70.95 | ||
Vaginoplasty is any surgical procedure that results in the construction or reconstruction of the vagina. It is a type of genitoplasty. Sometimes a vaginoplasty is needed following the treatment or removal of malignant growths or abscesses in order to restore a normal vaginal structure and function. Vaginoplasty is also used to correct congenital defects to the vagina, urethra and rectum. Vaginoplasty can correct uterine and vaginal prolapse. It will correct protrusion of the urinary bladder into the vagina and protrusion of the rectum into the vagina. Often, a vaginoplasty is performed to repair the vagina and its attached structures due to trauma.
Contents
- Medical uses
- Vaginoplasties in children
- Risks and complications
- Techniques
- Reconstructive surgery after cancer treatment
- McIndoe surgical technique
- Bowel vaginoplasty
- Sex reassignment surgery
- Elective vaginoplasty
- Labiaplasty
- Hymen surgical procedures
- Balloon vaginoplasty
- Pull through or Vecchietti procedure
- Wilson Method
- References
Congenital disorders such as adrenal hyperplasia can affect the structure and function of the vagina and sometimes the vagina is absent; these can be reconstructed or formed, using a vaginoplasty. Other candidates for the surgery include babies born with a microphallus, people with Müllerian agenesis resulting in vaginal hypoplasia, and women who have had a vaginectomy after malignancy or trauma. Vaginoplasty can reduce the size of the entrance of the vagina or alter the appearance of the vulva.
Medical uses
Vaginoplasty is the description of the following surgical interventions:
In some instances, extra tissue is needed to reconstruct or construct the vagina. These grafts used in vaginoplasty can be an allogenic, a heterograph, an autograft, xenograft, or a autologous material.
Vaginoplasties in children
Vaginoplasties may be performed in children or adolescents with intersex conditions or disorders of sex development. Conditions such as congenital adrenal hyperplasia virilize genetic females due to a 21-hydroxylase deficiency. Specific procedures include: clitoral reduction, labiaplasty, normalizing appearance, vagina creation. initiating vaginal dilation.
There are significant human rights concerns about vaginoplasties and other genital surgeries in children who are not old enough to consent, including concern with post-surgical sexual function, and assumptions of heteronormativity. There is no consensus attitude amongst clinicians about their necessity, timing, method or evaluation.
Vaginoplasty is used as part of the series of surgeries needed to treat those girls and women born with the bladder located outside of their abdomen. After the repairs, women have been able to give birth but are at risk of prolapse.
Risks and complications
Reconstructive vaginoplasty in children and adolescents carries the risk of "superinfection".
In adults, rates and types of complications varied with gender reassignment vaginoplasty. Necrosis of the clitoral region was 1-3%. Necrosis of the surgically created vagina was 3.7-4.2%. Vaginal shrinkage occurred was documented in 2-10% of those treated. Stricture, or narrowing of the vaginal orifice was reported in 12-15% of the cases. Of those reporting stricture, 41% underwent a second operation to correct the condition. Necrosis of two scrotal flaps has been described. Posterior vaginal wall is rare complication. Genital pain was reported in 4-9%. Rectovaginal fistula is also rare with only 1% documented. Vaginal prolapse was seen in 1-2% of people assigned male at birth undergoing this procedures.
The ability of emptying the bladder was affected after this procedure with 13% reporting improvement, 68% said that there was no change and 19% reported that voiding got worse.Those reporting a negative outcome experienced in which loss of bladder control and urinary incontinence were 19%. Urinary tract infections occurred in 32% of those treated.
Techniques
Non-surgical vagina creation was used in the past to treat the congenital absence of a vagina. The procedure involved the wearing of a saddle-like device and the use of increasing-diameter dilators. The procedure took several months and was sometimes painful. It was not effective in every instance. Uncommon growths, cysts, septums in the vagina can also require vaginoplasty.
Reconstructive surgery after cancer treatment
Radiological cancer treatment can result in the destruction or alteration of vaginal tissues. Vaginoplasty is often performed to reconstruct the vagina and other genital structures. In some cases, normal sexual function can be restored.
McIndoe surgical technique
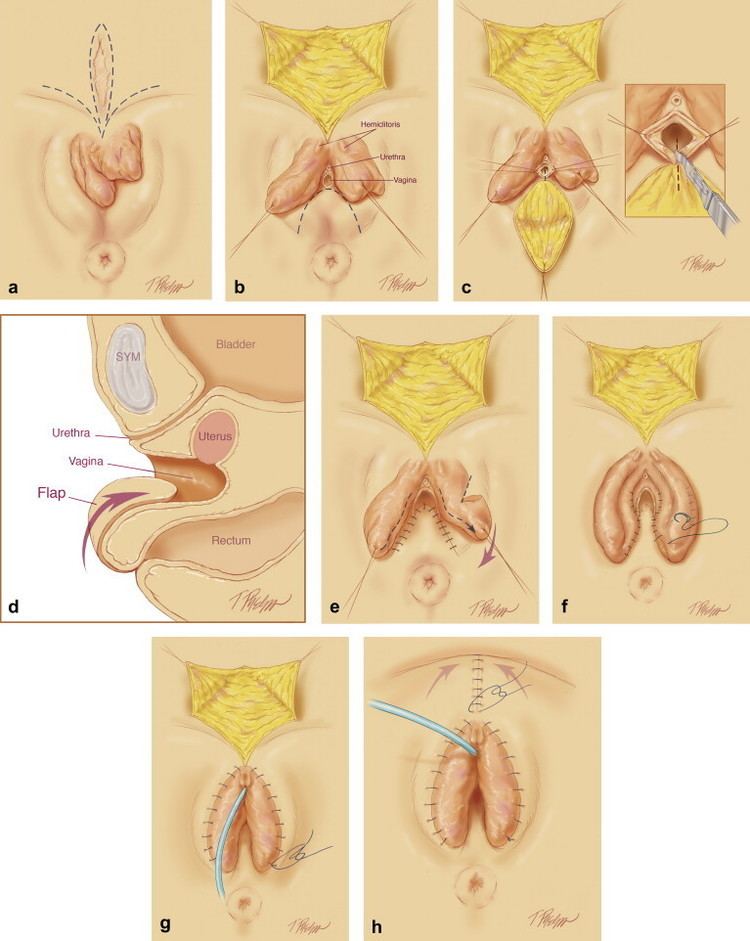
A canal is surgically constructed between the urinary bladder and urethra in the anterior portion of the pelvic region and the rectum. A skin graft is used from another area of the person's body. The graft is removed from the thigh, buttocks, or inguinal region. It is then wrapped around a mold and placed into the surgically created canal. Other materials have been used to create the lining of the new vagina. These have been cutaneous skin flaps, amniotic membranes, and buccal mucosa.
Bowel vaginoplasty
Bowel vaginoplasty is a commonly used method to create an artificial vagina in male-to-female transgender surgery.
Sex reassignment surgery
sex reassignment surgery to create a vagina consists of using segments from the large intestine or small intestine. In addition, penile-scrotal skin flaps are also used. Nongenital full-thickness graft (FTG) or split-thickness skin grafts from other parts of the body have been used. Inversion of the penile skin is the method most often selected by surgeons performing gender reassignment surgery. The inverted penile skin uses inferior pedicle skin or abdominal skin for the lining of the created vagina. The skin is cut to form an appropriate-sized flap. The skin flap is sometimes combined with a scrotal or urethral flap. Sex reassignment therapy is often part of the treatment plan.
Elective vaginoplasty
Critics have labeled such surgery as the "designer vagina". The American College of Obstetricians and Gynecologists issued a warning against these procedures in 2007 as did the Royal Australian College of Gynaecologists, and a commentary in the British Medical Journal strongly criticized the "designer vagina" in 2009. The Society of Obstetricians and Gynaecologists of Canada published a policy statement against elective vaginoplasty based upon the risks associated with unnecessary cosmetic surgery in 2013.
The World Health Organization describes any medically unnecessary surgery to the vaginal tissue and organs as female genital mutilation.
Vaginal rejuvenation is a form of elective plastic surgery. Its purpose is to restore or enhance the vagina's cosmetic appearance.
Labiaplasty
Labiaplasty can be performed as a discrete surgery, or as a subordinate procedure within a vaginoplasty. Some surgeries may be needed for discomfort occurring from chronic labial irritation that develops from tight clothing, sex, sports, or other physical activities.
Hymen surgical procedures
An imperforate hymen is the presence of tissue that completely covers the vaginal opening. It is cut to allow menstrual flow to exit during a short surgical procedure. A hymenorrhaphy is the surgical procedure that reconstructs the hymen.
Balloon vaginoplasty
In this procedure, a Foley catheter is laparoscopically inserted to the rectouterine pouch whereupon gradual traction and distension are applied to create a neovagina.
Pull through or Vecchietti procedure
In treating Müllerian agenesis, the Vecchietti procedure is a laparoscopic surgical technique that produces a vagina of dimensions (depth and width) comparable to those of a normal vagina (ca. 8.0 cm. deep). A small, plastic sphere (“olive”) is threaded (sutured) against the vaginal area; the threads are drawn though the vaginal skin, up through the abdomen, and through the navel. There, the threads are attached to a traction device, and then daily are drawn tight so that the “olive” is pulled inwards and stretches the vagina, by approximately 1.0 cm. per day, thereby creating a vagina, approximately 7.0 cm. deep by 7.0 cm. wide, in 7 days. The mean operating room (OR) time for the Vecchietti vaginoplasty is approximately 45 minutes; yet, depending upon the patient and her indications, the procedure might require more time. The outcomes of Vecchietti technique via the laparoscopic approach are found to be comparable to the procedure using laparotomy. In vaginal hypoplasia, traction vaginoplasty such as the Vecchietti technique seems to have the highest success rates both anatomically (99%) and functionally (96%) among available treatments.
Wilson Method
The penile-inversion technique of the Wilson Method is different from the traditional penile-inversion technique in that it is a three-stage surgery, comprising a two-stage initial vaginoplasty. The Wilson Method surgery is initially performed like a traditional penile inversion, until the vaginal-vault creation step, in which the vault of the vagina is left unfinished, as a raw surface, and is packed with a sterile stent, which, after 5–7 days, then is lined with a skin graft harvested from the buttocks. The penile skin is used to create the labia minora, clitoral hooding, and the anterior fourchette (frenulum); the glans penis is used to create the clitoris, and the scrotum is used to create the labia majora.
