Latin synovia FMA 12277 | TA A03.0.00.031 | |
 | ||
Synovia, more often called synovial fluid,[help 1] is a viscous, non-Newtonian fluid found in the cavities of synovial joints. With its egg white–like consistency, the principal role of synovial fluid is to reduce friction between the articular cartilage of synovial joints during movement.
Contents
Structure
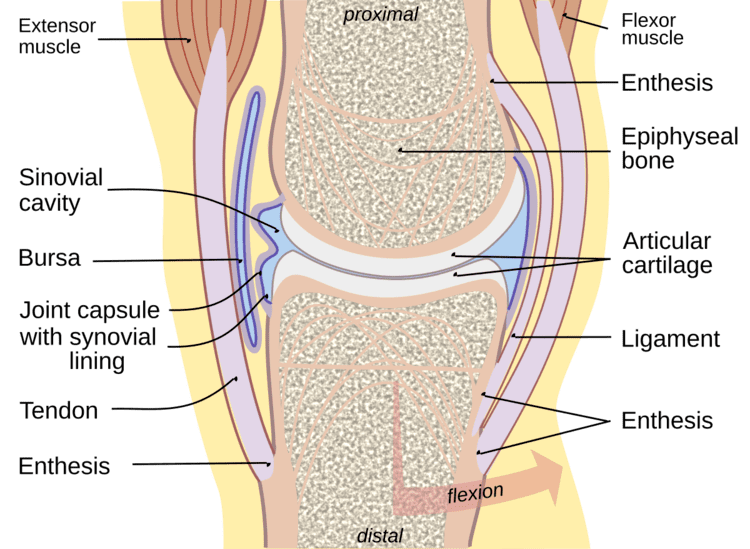
The inner membrane of synovial joints is called the synovial membrane and secretes synovial fluid into the joint cavity. Synovial fluid is an ultrafiltrate from plasma, and contains proteins derived from the blood plasma and proteins that are produced by cells within the joint tissues. The fluid contains hyaluronan secreted by fibroblast-like cells in the synovial membrane, lubricin (proteoglycan 4; PRG4) secreted by the surface chondrocytes of the articular cartilage and interstitial fluid filtered from the blood plasma. This fluid forms a thin layer (roughly 50 μm) at the surface of cartilage and also seeps into microcavities and irregularities in the articular cartilage surface, filling all empty space. The fluid in articular cartilage effectively serves as a synovial fluid reserve. During movement, the synovial fluid held in the cartilage is squeezed out mechanically to maintain a layer of fluid on the cartilage surface (so-called weeping lubrication). The functions of the synovial fluid include:
Composition
Synovial tissue is sterile and composed of vascularized connective tissue that lacks a basement membrane. Two cell types (type A and type B) are present: Type A is derived from blood monocytes, and it removes the wear-and-tear debris from the synovial fluid. Type B produces hyaluronan. Synovial fluid is made of hyaluronic acid and lubricin, proteinases, and collagenases. Synovial fluid exhibits non-Newtonian flow characteristics; the viscosity coefficient is not a constant and the fluid is not linearly viscous. Synovial fluid has rheopexy characteristics; viscosity increases and the fluid thickens over a period of continued stress. Normal synovial fluid contains 3–4 mg/ml hyaluronan (hyaluronic acid), a polymer of disaccharides composed of D-glucuronic acid and D-N-acetylglucosamine joined by alternating beta-1,4 and beta-1,3 glycosidic bonds. hyaluronan is synthesized by the synovial membrane and secreted into the joint cavity to increase the viscosity and elasticity of articular cartilages and to lubricate the surfaces between synovium and cartilage.
Synovial fluid contains lubricin (also known as PRG4) as a second lubricating component, secreted by synovial fibroblasts. Chiefly, it is responsible for so-called boundary-layer lubrication, which reduces friction between opposing surfaces of cartilage. There also is some evidence that it helps regulate synovial cell growth.
It also contains phagocytic cells that remove microbes and the debris that results from normal wear and tear in the joint.
Collection
Synovial fluid may be collected by syringe in a procedure termed arthrocentesis, also known as joint aspiration.
Classification
Synovial fluid may be classified into normal, noninflammatory, inflammatory, septic, and hemorrhagic:
Glucose (mg/dl) concentration in synovial fluid is nearly equal to serum.
Normal:
Normal or decreased:
Decreased:
Pathology
Many synovial fluid types are associated with specific diagnoses:
Analysis
Glucose (mg/dl) concentration in synovial fluid is nearly equal to serum.
The cytological and biochemical analysis of human synovial fluid began around 1940 using cadaver-derived fluid and comparing characteristics to those of, for instance, bovine synovial fluid.
Chemistry
The mucin clot test is a very old approach to determining if an inflammatory infiltrate is present. In this test, acetic acid is added to the synovial fluid specimen. In a normal specimen, this should lead to a congealing of the hyaluronic acid, forming a 'mucin clot.' If inflammation is present, a mucin clot is not formed (the hyaluronic acid is degraded).
Lactate is elevated in septic arthritis, usually above 250 mg/dL.
Complement factors are decreased in rheumatoid arthritis and lupus arthritis.
Microscopy
Microscopic analysis of synovial fluid is performed to evaluate for cell count and crystals. Crystals include monosodium urate, calcium pyrophosphate, hydroxyapatite and corticosteroid crystals.
Monosodium urate crystals are seen in gout or gouty arthritis and appear as needle-shaped negatively birefringent crystals varying in length from 2 to 20 µm. With negative birefringence, the crystals appear yellow in parallel light and blue with perpendicular light.
Calcium pyrophosphate crystals are seen in pseudogout (also known as calcium pyrophosphate deposition disease or, CPPD). These crystals are rod-shaped or rhomboids varying in length from 2 to 20 µm and with positive birefringence (blue with parallel light, yellow with perpendicular light).
Hydroxyapatite crystals are small and negatively birefringent. They are usually only detectable with an Alizarin Red S stain.
Corticosteroid crystals may be seen following therapeutic corticosteroid injection into the joint space. They appear blunt, jagged, and show variable birefringence.
Cracking joints
When the two articulating surfaces of a synovial joint are separated from one other, the volume within the joint capsule increases and a negative pressure results. The volume of synovial fluid within the joint is insufficient to fill the expanding volume of the joint and gases dissolved in the synovial fluid (mostly carbon dioxide) are liberated and quickly fill the empty space, leading to the rapid formation of a bubble. This process is known as cavitation. Cavitation in synovial joints results in a high frequency 'cracking' sound.
Etymology and pronunciation
The word synovia (/sᵻˈnoʊviə/) came to English from New Latin, where it was coined by Paracelsus. Several dictionaries indicate that the -ov- syllable of the word reflects the Greek ᾠόν and Latin ovum, cognates that both mean "egg" (which seems appropriate given the egg white–like nature of synovial fluid)—thus syn- + oo-/ovo- + -ia—although several others omit that aspect of the etymology, and one states, "probably formed arbitrarily by Paracelsus." Whether true or false, the connection to ovum is still helpful to students as a memory device.
Somewhat confusingly, the inflected form synovia can be either a principal (and uncountable) declined form referring to synovial fluid (synovia) or a second declined form as the plural of synovium (thus "synovial membranes", synovia). The avoidance of this ambiguity drives the use of the term synovial fluid to be more common than the use of its synonym synovia.
