Specialty endocrinology ICD-9-CM 267 DiseasesDB 13930 | ICD-10 E54 OMIM 240400 | |
 | ||
Synonyms Moeller's disease, Cheadle's disease, scorbutus, Barlow's disease, hypoascobemia | ||
Scurvy is a disease resulting from a lack of vitamin C. Early symptoms include weakness, feeling tired, curly hair, and sore arms and legs. Without treatment, decreased red blood cells, gum disease, and bleeding from the skin may occur. As scurvy worsens there can be poor wound healing, personality changes, and finally death from infection or bleeding.
Contents
- Signs and symptoms
- Cause
- Pathogenesis
- Prevention
- History
- Early modern era
- 18th century
- 19th century
- 20th century
- 21st century
- Human trials
- Other animals
- Name
- References
Scurvy is caused by not enough vitamin C in the diet. It typically takes at least a month of little to no vitamin C before symptoms occur. In modern times, it occurs most commonly in people with mental disorders, unusual eating habits, alcoholism, and old people who live alone. Other risk factors include intestinal malabsorption and dialysis. Humans and certain other animals require vitamin C in their diets to make the building blocks for collagen. Diagnosis is typically based on physical signs, X-rays, and improvement after treatment.
Treatment is with vitamin C supplements taken by mouth. Improvement often begins in a few days with complete recovery in a few weeks. Sources of vitamin C in the diet include citrus fruit and a number of vegetables such as tomatoes and potatoes. Cooking often decreases vitamin C in foods.
Scurvy is currently rare. It occurs more often in the developing world in association with malnutrition. Rates among refugees are reported at 5% to 45%. Scurvy was described as early as the time of ancient Egypt. It was a limiting factor in long distance sea travel, often killing large numbers of people. A Scottish surgeon in the Royal Navy, James Lind, was the first to prove it could be treated with citrus fruit in a 1753 publication. His experiments represented the first controlled trial. It took another 40 years before the British Navy began giving out lemon juice routinely.
Signs and symptoms
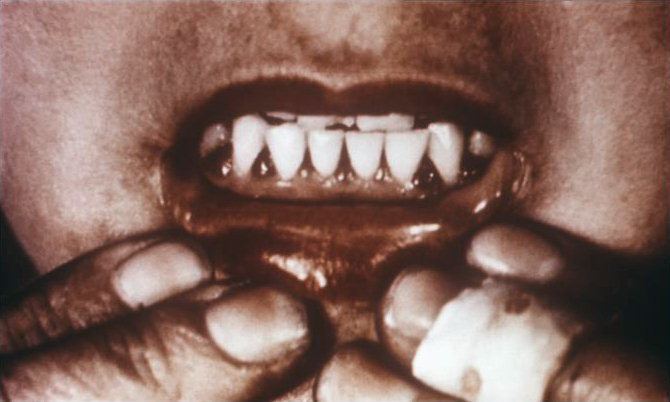
Early symptoms are malaise and lethargy. Even earlier might be a pain in a section of the gums which interferes with digestion. After 1–3 months, patients develop shortness of breath and bone pain. Myalgias may occur because of reduced carnitine production. Other symptoms include skin changes with roughness, easy bruising and petechiae, gum disease, loosening of teeth, poor wound healing, and emotional changes (which may appear before any physical changes). Dry mouth and dry eyes similar to Sjögren's syndrome may occur. In the late stages, jaundice, generalized edema, oliguria, neuropathy, fever, convulsions, and eventual death are frequently seen.
Cause
Scurvy or subclinical scurvy is caused by the lack of vitamin C. In modern Western societies, scurvy is rarely present in adults, although infants and elderly people are affected. Virtually all commercially available baby formulas contain added vitamin C. Human breast milk contains sufficient vitamin C, if the mother has an adequate intake.
Scurvy is one of the accompanying diseases of malnutrition (other such micronutrient deficiencies are beriberi or pellagra) and thus is still widespread in areas of the world depending on external food aid. Though rare, there are also documented cases of scurvy due to poor dietary choices by people living in industrialized nations.
Pathogenesis
Ascorbic acid is needed for a variety of biosynthetic pathways, by accelerating hydroxylation and amidation reactions. In the synthesis of collagen, ascorbic acid is required as a cofactor for prolyl hydroxylase and lysyl hydroxylase. These two enzymes are responsible for the hydroxylation of the proline and lysine amino acids in collagen. Hydroxyproline and hydroxylysine are important for stabilizing collagen by cross-linking the propeptides in collagen. Defective collagen fibrillogenesis impairs wound healing. Collagen is an important part of bone, so bone formation is affected. Defective connective tissue leads to fragile capillaries, resulting in abnormal bleeding. Untreated scurvy is invariably fatal.
Prevention
Scurvy can be prevented by a diet that includes vitamin C-rich foods such as sweet peppers, guava, blackcurrants, parsley, broccoli, and kiwifruit. Other sources rich in vitamin C are fruits such as papaya, strawberries and oranges or lemons. It is also found in vegetables, such as brussels sprouts, cabbage, spinach, and potatoes. Some fruits and vegetables not high in vitamin C may be pickled in lemon juice, which is high in vitamin C. Though redundant in the presence of a balanced diet, various nutritional supplements are available that provide ascorbic acid well in excess of that required to prevent scurvy.
Some animal products, including liver, Muktuk (whale skin), oysters, and parts of the central nervous system, including the brain, spinal cord, and adrenal medulla, contain large amounts of vitamin C, and can even be used to treat scurvy. Fresh meat from animals which make their own vitamin C (which most animals do) contains enough vitamin C to prevent scurvy, and even partly treat it. In some cases (notably in French soldiers eating fresh horse meat), it was discovered that meat alone, even partly cooked meat, could alleviate scurvy. In other cases, a meat-only diet could cause scurvy.
Scott's 1902 expedition used lightly fried seal meat and liver, whereby complete recovery from incipient scurvy was reported to take less than two weeks.
History
Scurvy was documented as a disease by Hippocrates, and Egyptians have recorded its symptoms as early as 1550 BCE. The knowledge that consuming foods containing vitamin C is a cure for scurvy has been repeatedly rediscovered and forgotten into the early 20th century.
Early modern era
In the 13th century, the Crusaders frequently suffered from scurvy. In the 1497 expedition of Vasco de Gama, the curative effects of citrus fruit were already known and confirmed by Pedro Álvares Cabral and his crew in 1507.
The Portuguese also planted fruit trees and vegetables in Saint Helena, a stopping point for homebound voyages from Asia, and left their sick, suffering from scurvy and other ailments to be taken home, if they recovered, by the next ship.
In 1500 one of the pilots of Cabral's fleet bound for India noted that in Malindi, its king offered the expedition fresh supplies such as lambs, chickens, and ducks, along with lemons and oranges, due to which "some of our ill were cured of scurvy".
Unfortunately, these travel accounts have not stopped further maritime tragedies caused by scurvy, first because of the lack of communication between travelers and those responsible for their health and also because fruits and vegetables could not be kept for long on ships.
In 1536, the French explorer Jacques Cartier, exploring the St. Lawrence River, used the local natives' knowledge to save his men who were dying of scurvy. He boiled the needles of the arbor vitae tree (Eastern White Cedar) to make a tea that was later shown to contain 50 mg of vitamin C per 100 grams. Such treatments were not available aboard ship, where the disease was most common.
During the Age of Exploration between 1500 and 1800, it has been estimated that scurvy killed at least two million sailors. Jonathan Lamb wrote: "In 1499, Vasco da Gama lost 116 of his crew of 170; In 1520, Magellan lost 208 out of 230;...all mainly to scurvy."
In 1593, Admiral Sir Richard Hawkins advocated drinking orange and lemon juice as a means of preventing scurvy.
In 1614 John Woodall, Surgeon General of the East India Company, published "The Surgion's Mate" as a handbook for apprentice surgeons aboard the company's ships. He repeated the experience of mariners that the cure for scurvy was fresh food or, if not available, oranges, lemons, limes and tamarinds. He was, however, unable to explain the reason why and his assertion had no impact on the opinion of the influential physicians who ran the medical establishment that it was a digestive complaint.
18th century
A 1707 handwritten book by Mrs. Ebot Mitchell discovered in a house in Hasfield, Gloucestershire, contains a "Recp.t for the Scurvy" that consisted of extracts from various plants mixed with a plentiful supply of orange juice, white wine or beer.
In 1734, the Leiden-based physician Johann Bachstrom published a book on scurvy in which he stated that "scurvy is solely owing to a total abstinence from fresh vegetable food, and greens; which is alone the primary cause of the disease" and urged the use of fresh fruit and vegetables as a cure.
However, it was not until 1747 that James Lind formally demonstrated that scurvy could be treated by supplementing the diet with citrus fruit, in the first ever clinical trial. In 1753, Lind published A Treatise of the Scurvy, in which he explained the details of his clinical trial, but it occupied only a few paragraphs in a work that was long and complex and had little impact. In fact, Lind himself never actively promoted lemon juice as a single ‘cure’. He shared medical opinion at the time that scurvy had multiple causes – notable hard work, bad water and the consumption of salt meat in a damp atmosphere which inhibited healthful perspiration and normal excretion - and therefore required multiple solutions. He was also side-tracked by the possibilities of producing a concentrated ‘rob’ of lemon juice by boiling it. Unfortunately this process destroyed the vitamin C and was unsuccessful.
During the 18th century, disease killed more British sailors than enemy action. It was mainly by scurvy that George Anson, in his celebrated voyage of 1740–1744, lost nearly two-thirds of his crew (1300 out of 2000) within the first ten months of the voyage. The Royal Navy enlisted 184,899 sailors during the Seven Years' War; 133,708 of these were "missing" or died by disease, and scurvy was the leading cause.
Although throughout this period sailors and naval surgeons were increasingly convinced that citrus fruits could cure scurvy, the classically trained physicians who ran the medical establishment dismissed this evidence as mere anecdote which did not conform to current theories of disease. Literature championing the cause of citrus juice therefore had no practical impact. Medical theory was based on the assumption that scurvy was a disease of internal putrefaction brought on by faulty digestion caused by the hardships of life at sea and the naval diet. Although this basic idea was given different emphases by successive theorists, the remedies they advocated (and which the navy accepted) amounted to little more than the consumption of ‘fizzy drinks’ to activate the digestive system, the most extreme of which was the regular consumption of ‘elixir of vitriol’ – sulphuric acid taken with spirits and barley water and laced with spices.
In 1764, a new variant appeared. Advocated by Dr David McBride and Sir John Pringle, Surgeon General of the Army and later President of the Royal Society, this idea was that scurvy was the result of a lack of ‘fixed air’ in the tissues which could be prevented by drinking infusions of malt and wort whose fermentation within the body would stimulate digestion and restore the missing gases. These ideas receiving wide and influential backing, when James Cook set off to circumnavigate the world (1768–1771) in HM Bark Endeavour, malt and wort were top of the list of the remedies he was ordered to investigate. The others were beer, sour crout and Lind's ‘rob’. The list did not include lemons.
Cook did not lose a single man to scurvy, and his report came down in favour of malt and wort, although it is now clear that the reason for the health of his crews on this and other voyages was Cook's regime of shipboard cleanliness, enforced by strict discipline, as well as frequent replenishment of fresh food and green stuffs. Another rule implemented by Cook was his prohibition of the consumption of salt fat skimmed from the ship's copper boiling pans, then a common practice in the Navy. In contact with air the copper formed compounds that prevented the absorption of vitamins by the intestines.
The first major long distance expedition that experienced virtually no scurvy was that of the Spanish naval officer Alessandro Malaspina, 1789–1794. Malaspina's medical officer, Pedro González, was convinced that fresh oranges and lemons were essential for preventing scurvy. Only one outbreak occurred, during a 56-day trip across the open sea. Five sailors came down with symptoms, one seriously. After three days at Guam all five were healthy again. Spain's large empire and many ports of call made it easier to acquire fresh fruit.
Although towards the end of the century MacBride's theories were being challenged, the medical establishment in Britain remained wedded to the notion that scurvy was a disease of internal ‘putrefaction’ and the Sick and Hurt Board, run by administrators, felt obliged to follow its advice. Within the Royal Navy however opinion - strengthened by first-hand experience of the use of lemon juice at the siege of Gibraltar and during Admiral Rodney's expedition to the Caribbean - had become increasingly convinced of its efficacy. This was reinforced by the writings of experts like Gilbert Blane and Thomas Trotter and by the reports of up-and-coming naval commanders.
With the coming of war in 1793, the need to eliminate scurvy acquired a new urgency. But the first initiative came not from the medical establishment but from the admirals. Ordered to lead an expedition against Mauritius, Rear Admiral Gardner was uninterested in the wort, malt and elixir of vitriol which were still being issued to ships of the Royal Navy, and demanded that he be supplied with lemons to counteract scurvy on the voyage. Members of the Sick and Hurt Board, recently augmented by two practical naval surgeons, supported the request and the Admiralty ordered that it be done. There was however a last minute change of plan. The expedition against Mauritius was cancelled. On 2 May 1794, only HMS Suffolk and two sloops under Commodore Peter Rainier sailed for the east with an outward bound convoy, but the warships were fully supplied with lemon juice and the sugar with which it had to be mixed. Then in March 1795, came astonishing news. Suffolk had arrived in India after a four-month voyage without a trace of scurvy and with a crew that was healthier than when it set out.
The effect was immediate. Fleet commanders clamoured also to be supplied with lemon juice and by June the Admiralty acknowledged the groundswell of demand in the navy had agreed to a proposal from the Sick and Hurt Board that lemon juice and sugar should in future be issued as a daily ration to the crews of all warships.
It took a few years before the method of distribution to all ships in the fleet had been perfected and the supply of the huge quantities of lemon juice required to be secured, but by 1800, the system was in place and functioning. This led to a remarkable health improvement among the sailors and consequently played a critical role in gaining the advantage in naval battles against enemies who had yet to introduce the measures.
19th century
The surgeon-in-chief of Napoleon's army at the Siege of Alexandria (1801), Baron Dominique-Jean Larrey, wrote in his memoirs that the consumption of horse meat helped the French to curb an epidemic of scurvy. The meat was cooked but was freshly obtained from young horses bought from Arabs and was nevertheless effective. This helped to start the 19th-century tradition of horse meat consumption in France.
Lauchlin Rose patented a method used to preserve citrus juice without alcohol in 1867, creating a concentrated drink known as Rose's lime juice. The Merchant Shipping Act of 1867 required all ships of the Royal Navy and Merchant Navy to provide a daily lime ration to sailors to prevent scurvy. The product became nearly ubiquitous, hence the term "limey", first for British sailors, then for English immigrants within the former British colonies (particularly America, New Zealand and South Africa), and finally, in old American slang, all British people.
The plant Cochlearia officinalis, also known as "Common Scurvygrass", acquired its common name from the observation that it cured scurvy, and it was taken on board ships in dried bundles or distilled extracts. Its very bitter taste was usually disguised with herbs and spices; however, this did not prevent scurvygrass drinks and sandwiches becoming a popular fad in the UK until the middle of the nineteenth century, when citrus fruits became more readily available.
West Indian limes began to supplement lemons when Spain's alliance with France against Britain in the Napoleonic Wars made the supply of Mediterranean lemons problematic and because they were more easily obtained from Britain's Caribbean colonies and were believed to be more effective because they were more acidic, and it was the acid, not the (then-unknown) Vitamin C that was believed to cure scurvy. In fact, the West Indian limes were significantly lower in Vitamin C than the previous lemons and further were not served fresh but rather as lime juice, which had been exposed to light and air and piped through copper tubing, all of which significantly reduced the Vitamin C. Indeed, a 1918 animal experiment using representative samples of the Navy and Merchant Marine's lime juice showed that it had virtually no antiscorbutic power at all.
The belief that scurvy was fundamentally a nutritional deficiency, best treated by consumption of fresh food, particularly fresh citrus or fresh meat, was not universal in the 19th and early 20th centuries, and thus sailors and explorers continued to suffer from scurvy into the 20th century. For example, the Belgian Antarctic Expedition of 1897–1899 became seriously affected by scurvy when its leader Adrien de Gerlache initially discouraged his men from eating penguin and seal meat.
In the Royal Navy's Arctic expeditions in the 19th century it was widely believed that scurvy was prevented by good hygiene on board ship, regular exercise, and maintaining the morale of the crew, rather than by a diet of fresh food. Navy expeditions continued to be plagued by scurvy even while fresh (not jerked or tinned) meat was well known as a practical antiscorbutic among civilian whalers and explorers in the Arctic. Even cooking fresh meat did not entirely destroy its antiscorbutic properties, especially as many cooking methods failed to bring all the meat to high temperature.
The confusion is attributed to a number of factors:
In the resulting confusion, a new hypothesis was proposed, following the new germ theory of disease – that scurvy was caused by ptomaine, a waste product of bacteria, particularly in tainted tinned meat.
Infantile scurvy emerged in the late 19th century because children were being fed pasteurized cow's milk, particularly in the urban upper class – the pasteurization killed bacteria but also destroyed vitamin C. This was eventually resolved by supplementing with onion juice or cooked potatoes.
20th century
At the time Robert Falcon Scott made his first expedition (1901–1904) to the Antarctic in the early 20th century, the prevailing theory was that scurvy was caused by "ptomaine poisoning", particularly in tinned meat. However, Scott discovered that a diet of fresh meat from Antarctic seals cured scurvy before any fatalities occurred.
In 1907, an animal model which would eventually help to isolate and identify the "antiscorbutic factor" was discovered. Axel Holst and Theodor Frølich, two Norwegian physicians studying shipboard beriberi contracted aboard ship's crews in the Norwegian Fishing Fleet, wanted a small test mammal to substitute for the pigeons then used in beriberi research. They fed guinea pigs their test diet of grains and flour, which had earlier produced beriberi in their pigeons, and were surprised when classic scurvy resulted instead. This was a serendipitous choice of animal. Until that time, scurvy had not been observed in any organism apart from humans and had been considered an exclusively human disease. (Some birds are susceptible to scurvy, but pigeons are unaffected by scurvy, as they produce vitamin C.) Holst and Frølich found they could cure scurvy in guinea pigs with the addition of various fresh foods and extracts. This discovery of an animal experimental model for scurvy, which was made even before the essential idea of "vitamins" in foods had been put forward, has been called the single most important piece of vitamin C research.
Vilhjalmur Stefansson, an arctic explorer who had lived among the Inuit, proved that the all-meat diet they consumed did not lead to vitamin deficiencies. He participated in a study in New York's Bellevue Hospital in February 1928, where he and a companion ate only meat for a year while under close medical observation, yet remained in good health.
In 1927, Hungarian biochemist Szent-Györgyi isolated a compound he called "hexuronic acid". Szent-Györgyi suspected hexuronic acid, which he had isolated from adrenal glands, to be the antiscorbutic agent, but he could not prove it without an animal-deficiency model. In 1932, the connection between hexuronic acid and scurvy was finally proven by American researcher Charles Glen King of the University of Pittsburgh. King's laboratory was given some hexuronic acid by Szent-Györgyi and soon established that it was the sought-after anti-scorbutic agent. Because of this, hexuronic acid was subsequently renamed ascorbic acid.
21st century
In the 2010s scurvy hasn't entirely disappeared from developed countries and rates while still very low, are increasing in the United Kingdom according to NHS Digital. Several cases were also reported in Westmead Hospital, Sydney, Australia.
Human trials
Notable human dietary studies of experimentally induced scurvy have been conducted on conscientious objectors during WWII in Britain and on Iowa state prisoner "volunteers" in the late 1960s. These studies both found that all obvious symptoms of scurvy previously induced by an experimental scorbutic diet with extremely low vitamin C content could be completely reversed by additional vitamin C supplementation of only 10 mg per day. In these experiments, no clinical difference was noted between men given 70 mg vitamin C per day (which produced blood levels of vitamin C of about 0.55 mg/dl, about 1/3 of tissue saturation levels), and those given 10 mg per day (which produced lower blood levels). Men in the prison study developed the first signs of scurvy about 4 weeks after starting the vitamin C-free diet, whereas in the British study, six to eight months were required, possibly because the subjects were pre-loaded with a 70 mg/day supplement for six weeks before the scorbutic diet was fed.
Men in both studies on a diet devoid or nearly devoid of vitamin C had blood levels of vitamin C too low to be accurately measured when they developed signs of scurvy, and in the Iowa study, at this time were estimated (by labeled vitamin C dilution) to have a body pool of less than 300 mg, with daily turnover of only 2.5 mg/day.
Other animals
Scurvy does not occur in most animals as they can make their own vitamin C. However, humans and other higher primates (the simians—monkeys and apes—and tarsiers), guinea pigs, most or all bats, and some species of birds and fish lack an enzyme (L-gulonolactone oxidase) necessary for such synthesis and must obtain vitamin C through their diet. The gene for L-gulonolactone oxidase is still present in the human genome, but deactivated by DNA mutations.
Almost all plant and animal species synthesize vitamin C. Notable mammalian exceptions include most or all of the order Chiroptera (bats), and one of the two major primate suborders, the "Anthropoidea" (Haplorrhini) which include tarsiers, monkeys, and apes, including human beings. The Strepsirrhini (non-tarsier prosimians) can make their own vitamin C, and these include lemurs, lorises, pottos, and galagos. Ascorbic acid is also not synthesized by at least two species of Caviidae, the capybara and the guinea pig. There are known species of birds and fish that do not synthesize their own Vitamin C. All species that do not synthesize ascorbate require it in the diet. Deficiency causes scurvy in humans, and somewhat similar symptoms in other animals.
Name
In babies, scurvy is sometimes referred to as Barlow's disease, named after Thomas Barlow, a British physician who described it in 1883. However, Barlow's disease may also refer to mitral valve prolapse.
