Specialty dermatology ICD-9-CM 686.01 eMedicine article/1123821 | ICD-10 L88 DiseasesDB 11064 MeSH D017511 | |
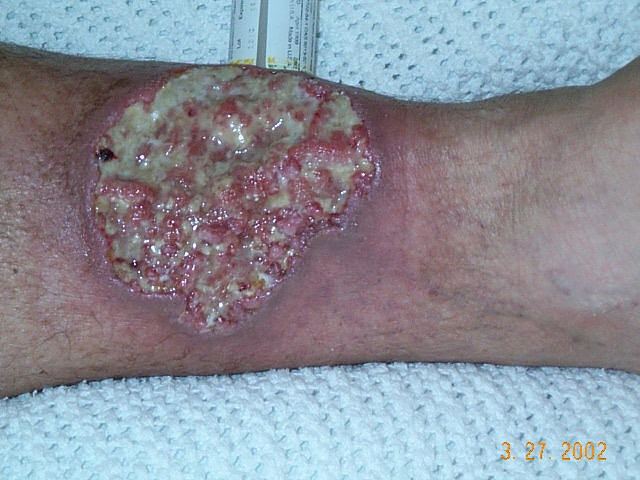 | ||
Pyoderma gangrenosum is a condition that causes tissue to become necrotic, causing deep ulcers that usually occur on the legs. When they occur, they can lead to chronic wounds. Ulcers usually initially look like small bug bites or papules, and they progress to larger ulcers. Though the wounds rarely lead to death, they can cause pain and scarring.
Contents
The disease was identified in 1930. It affects approximately 1 person in 100,000 in the population. Though it can affect people of any age, it mostly affects people in their 40s and 50s.
Types
There are two main types of pyoderma gangrenosum:
Other variations are:
Causes
Though the cause is not well understood, the disease is thought to be due to immune system dysfunction, and particularly improper functioning of neutrophils. In support of an immune cause, a variety of immune mediators such as IL-8, IL-1β, IL-6, interferon (IFN)-γ, G-CSF, TNF, matrix metallopaptidase (MMP)-9, MMP-10, and Elafin have all been reported to be elevated in patients with pyoderma gangrenosum.
Also in support of an immune cause is the finding that at least half of all pyoderma gangrenosum patients suffer from immune-mediated diseases. For instance, ulcerative colitis, rheumatoid arthritis, and multiple myeloma (MM) have all been associated with pyoderma gangrenosum. It can also be part of a syndromes such as PAPA syndrome.
One hallmark of pyoderma gangrenosum is pathergy, which is the appearance of new lesions at sites of trauma.
Associations
The following are conditions commonly associated with pyoderma gangrenosum:
Treatment
First-line therapy for disseminated or localized instances of pyoderma gangrenosum is systemic treatment by corticosteroids and ciclosporin. Topical application of clobetasol, mupirocin, and gentamicin alternated with tacrolimus can be effective.
Papules that begin as small "spouts" can be treated with Dakins Solution to prevent infection and wound clusters also benefit from this disinfectant. Wet to dry applications of Dakins can defeat spread of interior infection. Heavy drainage can be offset with Coban dressings. Grafting is not recommended due to tissue necrosis.
If ineffective, alternative therapeutic procedures include systemic treatment with corticosteroids and mycophenolate mofetil; mycophenolate mofetil and ciclosporin; tacrolimus; thalidomide; infliximab; or plasmapheresis.
There is currently a phase III trial for the use of the IL-1B modulating agent gevokizumab in treating the ulcers of pyoderma gangrenosum.
