Type Whole antibody Target TNF CAS ID 170277-31-3 | AHFS/Drugs.com Monograph Molar mass 144,190.3 g/mol | |
 | ||
Trade names Remicade, Remsima, Inflectra Pregnancycategory AU: CUS: B (No risk in non-human studies) | ||
New toolsets for drug level testing of the tnf inhibitors adalimumab infliximab and etanercept
Infliximab (trade names Remicade among others) is a chimeric monoclonal antibody biologic drug that works against tumor necrosis factor alpha (TNF-α) and is used to treat autoimmune diseases. Infliximab was approved by the U.S. Food and Drug Administration (FDA) for the treatment of Crohn's disease, ulcerative colitis, psoriasis, psoriatic arthritis, ankylosing spondylitis, and rheumatoid arthritis. It is used off-label outside its FDA approval for Behçet's disease and other conditions. Infliximab is administered by intravenous infusion, typically at six- to eight-week intervals. It cannot be given by mouth because the digestive system would destroy the drug.
Contents
- New toolsets for drug level testing of the tnf inhibitors adalimumab infliximab and etanercept
- Chronic inflammation in ibd and how anti tnf therapy works
- Crohns disease
- Fistulizing disease
- Inflammatory disease
- Ulcerative colitis
- Psoriatic arthritis
- Other
- Adverse effects
- Pharmacology
- History
- Marketing
- Biosimilars
- Availabilityaffordability
- References
Infliximab works by binding to TNF-α. TNF-α is a chemical messenger (cytokine) and a key part of the autoimmune reaction. In rheumatoid arthritis, infliximab seems to work by preventing TNF-α from binding to its receptor in the cell.
Infliximab is an artificial antibody. It was originally developed in mice as a mouse antibody. Because humans have immune reactions to mouse proteins, the mouse common domains were replaced with similar human antibody domains. They are monoclonal antibodies and have identical structures and affinities to the target. Because they are a combination of mouse and human antibody amino acid sequences, they are called a "chimeric monoclonal antibody". In the United States, Remicade/infliximab can cost $19,000 to $22,000 a year per patient, according to Centocor in 2007.
Infliximab biosimilars have been approved in the EU (2013), Japan (2014), and USA (2016).
Chronic inflammation in ibd and how anti tnf therapy works
Crohn's disease
Three phenotypes, or categories of disease, are present in Crohn's disease: stricturing disease (which causes narrowing of the bowel), penetrating disease (which causes fistulae or abnormal connections of the bowel), and inflammatory disease (which primarily causes inflammation).
Fistulizing disease
Infliximab was first used for closure of fistulae in Crohn's disease in 1999. In a 94-patient, phase II clinical trial, the researchers showed Infliximab was effective in closing fistulae between the skin and bowel in 56-68% of patients. A large, 296-patient, Phase III clinical trial called the ACCENT 2 trial, showed infliximab was additionally beneficial in maintaining closure of fistulae, with almost two-thirds of all patients treated with the three initial doses of infliximab having a fistula response after 14 weeks, and 36% of patients maintaining closure of fistulae after a year, compared with 19% who received placebo therapy. This final trial resulted in the FDA approval of the drug to treat fistulizing disease.
Inflammatory disease
Infliximab has been used to induce and maintain remission in inflammatory Crohn's disease. The ACCENT 1 trial, a large, multicentre trial, found 39 to 45% of patients treated with infliximab, who had an initial response to it, maintained remission after 30 weeks, compared with 21% who received placebo treatment. It also showed a mean maintenance of remission from 38 to 54 weeks compared with 21 weeks for patients who received placebo treatment.
Crohn's patients have flares of their disease between periods of disease quiescence. Severe flares are usually treated with steroid medications to obtain remission, but steroids have many undesirable side effects, so some gastroenterologists are now advocating the use of infliximab as the first drug to try to get patients into remission. This has been called the top-down approach to treatment.
Ulcerative colitis
Infliximab targets TNF, thought to be more related to Th1 cytokines. Ulcerative colitis was thought to be a Th2 disease, and infliximab would be of limited use. However, patients with ulcerative colitis have begun to be treated with infliximab on the basis of two large clinical trials conducted in 2005 by Paul Rutgeerts and William Sandborn. The Acute ulcerative Colitis Treatment trials (ACT1 and ACT2) to evaluate the utility of infliximab in ulcerative colitis showed 44-45% of patients treated with infliximab for a year maintained a response to the medication, compared with 21% of patients who were treated with placebo medication. At two months, the response was 61-69% for patients treated with infliximab, and 31% for those treated with placebo.
Psoriatic arthritis
In psoriatic arthritis (PsA), inhibitors of TNF, such as infliximab, improve the signs and symptoms. Several therapies with modest efficacy have been studied in nail psoriasis. Among available agents, higher quality data are available to support the efficacy of cyclosporine and infliximab. Based on studies in AS, the results suggest infliximab, etanercept, and adalimumab have the potential to reduce the signs and symptoms of moderate to severely active axial involvement in PsA in patients who have had an inadequate response to NSAID (level 1a, grade A). The anti-TNF agents (infliximab and etanercept; level 1b, grade A) are more effective for the treatment of enthesitis than traditional agents. Results suggest infliximab is effective for the treatment of dactylitis in PsA.
Other
It was approved for treating ankylosing spondylitis, psoriatic arthritis, psoriasis, rheumatoid arthritis. Infliximab is also prescribed (out of indication) for the treatment of Behçet's disease.
Infliximab is the most frequently used biological agent in treating relapsing polychondritis. Half of the patients saw benefit from this treatment, and a few other patients experienced infections that in some cases lead to death.
There have been numerous case reports of the efficacy of infliximab in various inflammatory skin conditions diseases; the FDA approved infliximab for chronic severe plaque psoriasis in adults in September 2006.
Infliximab has been tested in COPD but there was no evidence of benefit with the possibility of harm.
Adverse effects
Infliximab has adverse effects, some life-threatening, common to drugs in the class of TNF inhibiting immunosuppressants (which also includes etanercept (Enbrel) and adalimumab (Humira)). Some of the most severe are:
Cases of leukopenia, neutropenia, thrombocytopenia, and pancytopenia (some fatal) have been reported with infliximab. The FDA issued a warning to doctors appearing in the respective product labeling of infliximab instructing them to screen and monitor potential patients more carefully. The FDA issued a warning to doctors that there is an increased risk of lymphoma and other cancers associated with the use of infliximab and other tumor necrosis factor blockers in children and adolescents.
Maintenance therapy with the drug (versus intermittent or sporadic therapy) lessens the likelihood of developing antibodies to infliximab which are known to reduce the efficacy of the drug. Combination treatment with methotrexate (an antifolate drug which suppresses the immune system) has been shown to reduce the formation of these antibodies in patients with rheumatoid arthritis and combination therapy with other immunosuppressants has been shown to reduce the likelihood of these antibodies being formed in Crohn's disease. The use of immunosuppressants may not be necessary in all diseases for which infliximab is indicated, and indiscriminant uses of these other immunosuppressants carry their own risks. Infliximab was studied in monotherapy (without concomitant immunosuppressants such as methotrexate or azathioprine) in psoriasis, psoriatic arthritis, and ankylosing spondylitis. Only its use in rheumatoid arthritis requires the concomitant use of methotrexate by FDA product labeling; however, the concomitant use of methotrexate in other disease states may help to reduce the body's immune response to the infliximab and increase its duration of efficacy.
Pharmacology
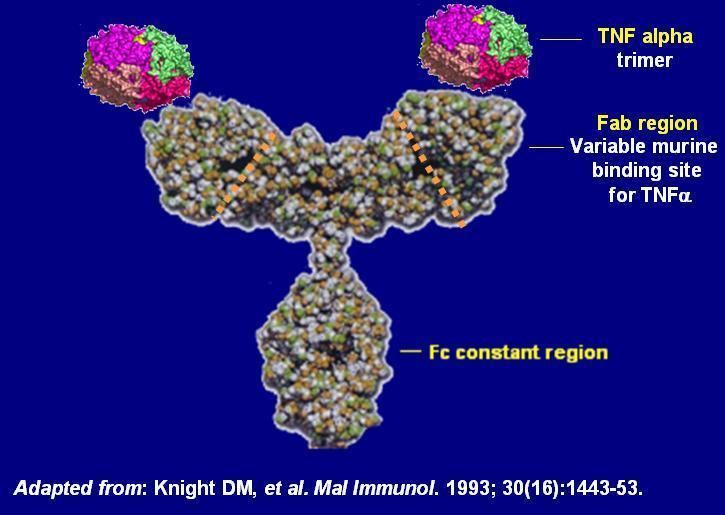
Infliximab is a purified, recombinant DNA-derived chimeric human-mouse IgG monoclonal antibody that consists of mouse heavy and light chain variable regions combined with human heavy and light chain constant regions. It has a serum half-life of 9.5 days and can be detected in serum 8 weeks after infusion treatment.
Infliximab neutralizes the biological activity of TNF-α by binding with high affinity to the soluble (free floating in the blood) and transmembrane (located on the outer membranes of T cells and similar immune cells) forms of TNF-α, and inhibits or prevents the effective binding of TNF-α with its receptors. Infliximab and adalimumab (another TNF antagonist) are in the subclass of "anti-TNF antibodies" (they are in the form of naturally occurring antibodies), and are capable of neutralizing all forms (extracellular-, transmembrane-, and receptor-bound) TNF-α. Etanercept, a third TNF antagonist, is in a different subclass (receptor-construct fusion protein), and, because of its modified form, cannot neutralize receptor-bound TNF-α. Additionally, the anti-TNF antibodies adalimumab and infliximab have the capability of lysing cells involved in the inflammatory process, whereas the receptor fusion protein apparently lacks this capability. Although the clinical significance of these differences have not been absolutely proven, etanercept, has been shown to perform worse than placebo for Crohn's disease. These differences may account for the differential actions of these drugs in both efficacy and side effects.
Infliximab has high specificity for TNF-α, and does not neutralize TNF beta (TNFβ, also called lymphotoxin α), an unrelated cytokine that uses different receptors from TNF-α. Biological activities attributed to TNF-α include induction of proinflammatory cytokines (such as interleukins IL-1 and IL-6), enhancement of leukocyte movement or migration from the blood vessels into the tissues (by increasing the permeability of endothelial layer of blood vessels), and increasing the release of adhesion molecules. Infliximab prevents disease in transgenic mice (a special type of mice biologically engineered to produce a human form of TNF-α and which are used to test the results of these drugs that might be expected in humans). These experimental mice develop arthritis as a result of their production of human TNF-α, and when administered after disease onset, infliximab allows eroded joints to heal.
Other monoclonal antibodies targeting TNF-α are golimumab, adalimumab, and certolizumab pegol. Etanercept also binds and inhibits the action of TNF-α, but is not a monoclonal antibody (it is instead a fusion of TNF-receptor and an antibody constant region).
History
The role of TNF as a key player in the development of rheumatoid arthritis was originally demonstrated by George Kollias and colleagues in proof of principle studies in transgenic animal models.
Infliximab was developed by Junming Le and Jan Vilcek at New York University School of Medicine and developed by Centocor, (now Janssen Biotech, Inc.)
Marketing
Remicade is marketed by Janssen Biotech, Inc. (formerly Centocor Biotech, Inc.) in the USA, Mitsubishi Tanabe Pharma in Japan, Xian Janssen in China, and Schering-Plough (now part of Merck & Co) elsewhere.
Biosimilars
In June 2013, two biosimilar versions (Inflectra and Remsima) were submitted for approval in Europe, by Hospira and Celltrion Healthcare respectively. Both had a positive opinion from European Medicines Agency’s (EMA) Committee for Medicinal Products for Human Use (CHMP) for sale in the European Union (EU). Celltrion obtained marketing authorization approval (MAA) from 27 EU countries and 3 EEA (European Economic Area) countries by Sept 2013.
In Japan, Celltrion has received marketing authorization for Remsima from Japan's Ministry of Health, Labour and Welfare (MHLW) in July 2014.
In India, Epirus Biopharmaceuticals has obtained approval to produce biosimilar infliximab under the brand name "Infimab" (trail name BOW015).
The US FDA approved Pfizer's Inflectra in April 2016. The US FDA approved Celltrion's Remsima in April 2016.
Biogen has released another biosimilar, Flixabi, which has been approved in Germany, the UK, and the Netherlands.
Availability/affordability
Like all of the TNF inhibitors, infliximab is an expensive medication, costing about US$900 for a 100 mg dose, and within the United States is covered by almost every medical insurance plan (though caps on many plans make it possible to be covered for only a subset of treatments in the course of a year). Infliximab is supplied as a sterile, white, lyophilized (freeze-dried) powder, so must be reconstituted and administered by a health care professional, usually in a hospital or office setting. For this reason, it is usually covered under major medical insurance rather than prescription drug coverage. The loading regimen for all approved indications occurs at weeks 0, 2, and 6 at the above dosages.
Infliximab is available from the NHS in the UK for Crohn's disease treatment provided three criteria are met. Patients should have severe active Crohn's disease with a CDAI score of 300 or more, have not responded to immunomodulating drugs and corticosteroids, and for whom surgery is inappropriate. Since February 2015 it is also approved for the treatment of ulcerative colitis where other treatments have not worked.
Infliximab is available through the PBS in Australia for Crohn's disease treatment provided the patient has not responded to conventional treatment and is suffering from a severe case of the condition.
Infliximab is available in the Republic of Ireland through the HSE's Medical Card and Drug Payment Scheme.
Johnson & Johnson reported in its 2013 annual report, "REMICADE® (infliximab), accounted for approximately 9.4% of the Company's total revenues for fiscal 2013."
