Rank Species | ||
 | ||
Scientific name Staphylococcus saprophyticus Similar Bacteria, Staphylococcus haemolyticus, Staphylococcus hominis, Proteus, Morganella morganii | ||
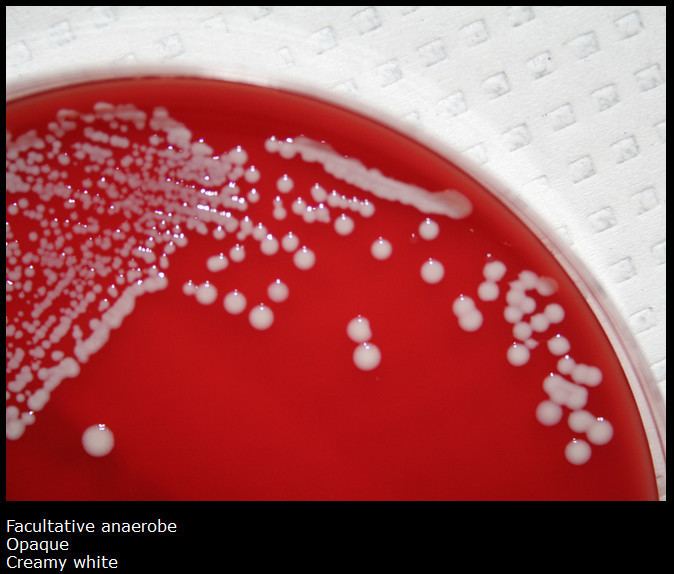
Staphylococcus saprophyticus is a Gram-positive coccus belonging to the coagulase-negative Staphylococcus genus. S. saprophyticus is a common cause of community-acquired urinary tract infections.
Contents
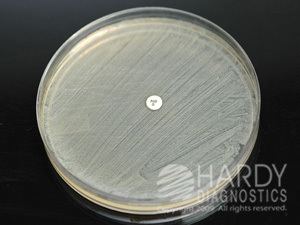
- Staphylococcus saprophyticus on blood agar with a nb disc
- History
- Epidemiology and pathogenesis
- Clinical features
- Laboratory diagnosis
- Treatment
- Different subspecies
- References
Staphylococcus saprophyticus on blood agar with a nb disc
History
S. saprophyticus was not recognized as a cause of urinary tract infections until the early 1970s, more than 10 years after its original demonstration in urine specimens. Prior to this, the presence of coagulase-negative staphylococci (CoNS) in urine specimens was dismissed as contamination.
Epidemiology and pathogenesis

In humans, S. saprophyticus is found in the normal flora of the female genital tract and perineum. It has been isolated from other sources, too, including meat and cheese products, vegetables, the environment, and human and animal gastrointestinal tracts. S. saprophyticus causes 10–20% of urinary tract infections (UTIs). In females 17–27 years old, it is the second-most common cause of community-acquired UTIs, after Escherichia coli. Sexual activity increases the risk of S. saprophyticus UTIs because bacteria are displaced from the normal flora of the vagina and perineum into the urethra. Most cases occur within 24 hours of sex, earning this infection the nickname "honeymoon cystitis". S. saprophyticus has the capacity to selectively adhere to human urothelium. The adhesin for S. saprophyticus is a lactosamine structure. S. saprophyticus produces no exotoxins.
Clinical features
Patients with urinary tract infections caused by S. saprophyticus usually present with symptomatic cystitis. Symptoms include a burning sensation when passing urine, the urge to urinate more often than usual, a 'dripping effect' after urination, weak bladder, a bloated feeling with sharp razor pains in the lower abdomen around the bladder and ovary areas, and razor-like pains during sexual intercourse. Signs and symptoms of renal involvement are also often registered.
Laboratory diagnosis
The urine sediment of a patient with a S. saprophyticus urinary tract infection has a characteristic appearance under the microscope manifesting leukocytes, erythrocytes, and clumping due to cocci adhering to cellular elements. Chemical screening methods for bacteriuria, such as, urine nitrate and glucose do not always detect S. saprophyticus infection. This is because unlike Gram-negative Enterobacteriaceae urinary tract infections, S. saprophyticus does not reduce nitrate and has a longer generation time, thus does not consume glucose as rapidly. Even when such an infection occurs above the neck of the bladder, low numbers of colony-forming units (less than 105 cfu/ml) are often present.
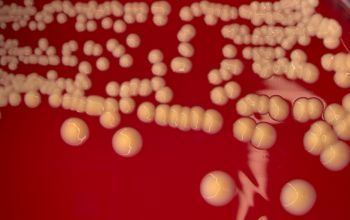
S. saprophyticus is identified as belonging to the Staphylococcus genus using the Gram stain and catalase test. It is identitified as a species of coagulase-negative staphylococci (CoNS) using the coagulase test. Lastly, S. saprophyticus is differentiated from S. epidermidis, another species of pathogenic CoNS, by testing for susceptibility to the antibiotic novobiocin. S. saprophyticus is novobiocin-resistant, whereas S. epidermidis is novobiocin-sensitive.
Treatment
S. saprophyticus urinary tract infections are usually treated with trimethoprim-sulfamethoxazole or with a quinolone such as norfloxacin.
The many home remedies or natural treatments for urinary tract infections are not clinically proven, such as cranberry juice, alkalinization, and many types of common herbs and spices. Some show promise, such as to affect the formation of biofilms on surfaces or medical equipment, and in other in vitro situations.
Different subspecies
Two subspecies of S. saprophyticus exist: S. s. bovis and S. s. saprophyticus, the latter more commonly found in human UTIs. S. s. saprophyticus is nitrate-reductase negative and pyrrolidonyl-arylamidase negative, while S. saprophyticus bovis is nitrate-reductase positive and pyrolidonyl-arylamidase negative.
