ICD-10 T33-T35 DiseasesDB 31167 | ICD-9-CM 991.0-991.3 MedlinePlus 000057 | |
 | ||
Specialty Emergency medicine, orthopedics eMedicine emerg/209 med/2815 derm/833 ped/803 | ||
Frostbite is when exposure to cold temperatures causes freezing to the skin or other tissues. It most commonly affects the hand, feet, and face. The longer areas are exposed to cold, typically the worse the frostbite. Frostbite is classified by degrees of severity, with first degree being superficial damage to surface skin and fourth degree involving bone, muscle and tendon. This causes irreversible damage and often requires amputation.
Contents
- Signs and symptoms
- First degree
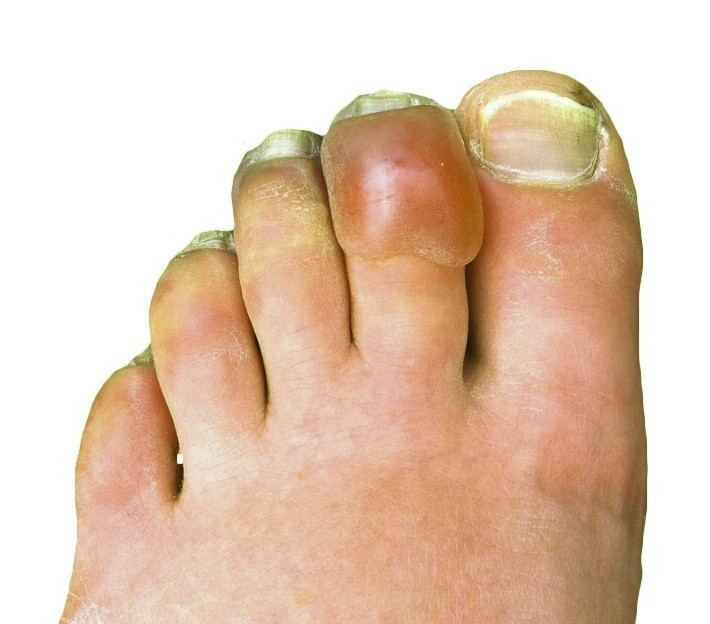
- Second degree
- Third degree
- Fourth degree
- Risk factors
- Freezing
- Rewarming
- Non freezing cold injury
- Diagnosis
- Prevention
- Pre hospital care
- Hospital management
- Thrombolysis
- Vasodilators
- Surgery
- Prognosis
- Grades
- Epidemiology
- History
- Society and culture
- Research directions
- References
People who are exposed to cold temperatures for prolonged periods are at greatest risk of frostbite, such as winter sports enthusiasts, military personnel, and homeless individuals. People with conditions that impair circulation of blood or ability to seek shelter are also at increased risk. These groups include people with diabetes and people who use alcohol. Cold temperatures cause blood vessels to narrow, slowing the flow of warm blood from the core of the body to the extremities. With prolonged exposure to cold, ice crystals form in tissues. These ice crystals, in turn, damage cells and blood vessels. Specific tests are not typically required for diagnosis. The person's history and physical exam are sufficient. Frostnip, pernio and trench foot can look similar to frostbite.
Frostbite is preventable. The Wilderness Medical Society recommends avoiding temperatures below 15C, covering the body properly and avoiding situations that increase heat loss such as starvation, exhaustion and intoxication. Treatment by rewarming, though necessary, also causes damage to tissues. Non-freezing cold injury causes inflammation of tissues without the formation of ice crystals. Treatment consists of rewarming, when refreezing is not a concern. Increasing the core temperature to above 35C is of critical importance as hypothermia is life-threatening. Aspirin and ibuprofen may prevent damaging inflammation. Wound care, antibiotics, tetanus toxoid, and pain management are often needed. Surgical debridement or amputation are sometimes necessary in severe frostbite, however, these should be delayed for several weeks until the extent of the permanent damage is known.
Signs and symptoms
Areas that are usually affected include cheeks, ears, nose and fingers and toes. Frostbite is often preceded by frostnip. The symptoms of frostbite progress with prolonged exposure to cold. Historically, frostbite has been classified by degrees according to skin and sensation changes, similar to burn classifications. However, the degrees do not correspond to the amount of long term damage. A simplification of this system of classification is superficial (first or second degree) or deep injury (third or fourth degree).
First degree
Second degree
Third degree
Fourth degree
Risk factors
The major risk factor for frostbite is exposure to cold through geography, occupation and/or recreation. Inadequate clothing and shelter are major risk factors. Frostbite is more likely when the body's ability to produce or retain heat is impaired. Physical, behavioral, and environmental factors can all contribute to the development of frostbite. Immobility and physical stress (such as malnutrition or dehydration) are also risk factors. Disorders and substances that impair circulation contribute, including diabetes, Raynaud's phenomenon, tobacco and alcohol use. Homeless individuals and individuals with some mental illnesses may be at higher at risk.
Freezing
In frostbite, cooling of the body causes narrowing of the blood vessels (vasoconstriction). Temperatures below -4C or lower are required to form ice crystals in the tissues. the process of freezing causes ice crystals to form in tissue, which causes damage at the cellular level. Ice crystals can damage cell membranes directly. In addition, ice crystals can damage small blood vessels at the site of injury. Scar tissue forms when fibroblasts replace the dead cells.
Rewarming
Rewarming causes tissue damage through reperfusion injury, which involves vasodilation, swelling (edema), and poor blood flow (stasis). Platelet aggregation is another possible mechanism of injury. Blisters and spasm of blood vessels (vasospasm) can develop after rewarming.
Non-freezing cold injury
The process of frostbite differs from the process of non-freezing cold injury (NFCI). In NFCI, temperature in the tissue decreases gradually. This slower temperature decrease allows the body to try to compensate through alternating cycles of closing and opening blood vessels (vasoconstriction and vasodilation). If this process continues, inflammatory mast cells act in the area. Small clots (microthrombi) form and can cut off blood to the affected area (known as ischemia) and damage nerve fibers. Rewarming causes a series of inflammatory chemicals such as prostaglandins to increase localized clotting.
Diagnosis
Frostbite is diagnosed based on signs and symptoms as described above, and by patient history. Other conditions that can have a similar appearance or occur at the same time include:
People who have hypothermia often have frostbite as well. Since hypothermia is life-threatening this should be treated first. Technetium-99 or MR scans are not required for diagnosis, but might be useful for prognostic purposes.
Prevention
The Wilderness Medical Society recommends covering the skin and scalp, taking in adequate nutrition, avoiding constrictive footwear and clothing, and remaining active without causing exhaustion. Supplemental oxygen might also be of use at high elevations. Additional measures to prevention frostbite include:
Pre-hospital care
Individuals with frostbite or potential frostbite should go to a protected environment and get warm fluids. If there is no risk of re-freezing, the extremity can be exposed and warmed in the groin or underarm of a companion. If the area is allowed to refreeze, there can be worse tissue damage. If the area cannot be reliably kept warm, the person should be brought to a medical facility without rewarming the area. Rubbing the affected area can also increase tissue damage. Aspirin and ibuprofen can be given in the field to prevent clotting and inflammation.
Hospital management
The first priority in people with frostbite should be to assess for hypothermia and other life-threatening complications of cold exposure. Before treating frostbite, the core temperature should be raised above 35C. Oral or intravenous (IV) fluids should be given.
Rewarming
If the area is still partially or fully frozen, it should be rewarmed in the hospital with a warm bath with povidone iodine or chlorhexidine antiseptic. Active rewarming seeks to warm the injured tissue as quickly as possible without burning. The faster tissue is thawed, the less tissue damage occurs. According the Handford and colleagues, "The Wilderness Medical Society and State of Alaska Cold Injury Guidelines recommend a temperature of 37°C–39°C, which decreases the pain experienced by the patient whilst only slightly slowing rewarming time." Warming takes 15 minutes - 1 hour. Rewarming can be very painful, so pain management is important.
Other considerations for standard hospital management include:
Thrombolysis
People with potential for large amputations and who present within 24 hours of injury can be given TPA with heparin or enoxaparin. These medications should be withheld if there are any contraindications. Bone scans or CT angiography can be done to assess damage.
Vasodilators
Blood vessel dilating (vasodilating) medications such as iloprost may prevent blood vessel blockage. This treatment might be appropriate in grades 2-4 frostbite, when people get treatment within 48 hours.
Surgery
Various types of surgery might be indicated in frostbite injury, depending on the type and extent of damage. Debridement or amputation of necrotic tissue is usually delayed unless there is gangrene or systemic infection (sepsis). This has led to the adage "Frozen in January, amputate in July". If symptoms of compartment syndrome develop, fasciotomy can be done to attempt to preserve blood flow.
Prognosis
Tissue loss and autoamputation are potential consequences of frostbite. Permanent nerve damage including loss of feeling can occur. It can take several weeks to know what parts of the tissue will survive. Time of exposure to cold is more predictive of lasting injury than temperature the individual was exposed to. The classification system of grades, based on the tissue response to initial rewarming and other factors is designed to predict degree of longterm recovery.
Grades
Grade 1: if there is no initial lesion on the area, no amputation or lasting effects are expected
Grade 2: if there is an lesion on the distal body part, tissue and fingernails can be destroyed
Grade 3: if there is a lesion on the intermediate or near body part, autoamputation and loss of function can occur
Grade 4: if there is a lesion very near the body (such as the carpals of the hand), the limb can be lost. Sepsis and/or other systemic problems are expected.
A number of long term sequelae can occur after frostbite. These include transient or permanent changes in sensation, paresthesia, increased sweating, cancers, and bone destruction/arthritis in the area affected.
Epidemiology
There is a lack of comprehensive statistics about the epidemiology of frostbite. In the United States, frostbite is more common in northern states. In Finland, annual incidence was 2.5 per 100,000 among civilians, compared with 3.2 per 100,000 in Montreal. Research suggests that men ages 30–49 are at highest risk, possibly due to occupational or recreational exposures to cold.
History
Frostbite has been described in military history for millennia. The Greeks encountered and discussed the problem of frostbite as early as 4000 BCE. Researchers have found evidence of frostbite in humans dating back 5,000 years, in an Andean mummy. Napoleon's Army was the first documented instance of mass cold injury in the early 1800s. According to Zafren, nearly 1 million combatants fell victim to frostbite in the First and Second World Wars, and the Korean War.
Society and culture
Notable cases of frostbite include Captain Lawrence Oates, an English army captain and Antarctic explorer, who died of complications of frostbite in 1912. In 1982, noted American rock climber, Hugh Herr lost both legs below the knee to frostbite after being stranded on Mount Washington in a blizzard. In addition, many Mount Everest explorers have lost digits and limbs to frostbite. Beck Weathers, a survivor of the 1996 Everest disaster, lost his nose and hands to frostbite. In 1999, Scottish mountaineer, Jamie Andrew had all four limbs amputated due to sepsis from frostbite sustained climbing the Mont Blanc massif.
Research directions
Evidence is insufficient to determine whether or not hyperbaric oxygen therapy as an adjunctive treatment can assist in tissue salvage. Cases have been reported, but no randomized control trial has been performed on humans.
Medical sympathectomy using intravenous reserpine has also been attempted with limited success. Studies have suggested that administration of tissue plasminogen activator (tPa) either intravenously or intra-arterially may decrease the likelihood of eventual need for amputation.
