Trade names Propecia, Proscar MedlinePlus a698016 CAS ID 98319-26-7 Bioavailability 63% | AHFS/Drugs.com Monograph Routes ofadministration Oral Molar mass 372.549 g/mol | |
 | ||
Pregnancycategory X (will cause birth defects in a fetus) ATC code G04CB01 (WHO) D11AX10 (WHO) | ||
Pros cons of propecia finasteride thinning hair
Finasteride, sold under the brand names Proscar and Propecia among others, is a medication used for the treatment of benign prostatic hyperplasia (enlarged prostate) and pattern hair loss. It is a type II and type III 5α-reductase inhibitor; 5α-reductase, an enzyme, converts testosterone to dihydrotestosterone (DHT).
Contents
- Pros cons of propecia finasteride thinning hair
- The lifelong duration of finasteride and minoxidil hair loss treatment and a one time alternative
- Prostate enlargement
- Pattern hair loss
- Excessive hair growth
- Transgender women
- Contraindications
- Adverse effects
- Sexual function
- Mechanism of action
- Chemistry
- History
- Society and culture
- Athletics
- Brand names
- Controversy
- References
The lifelong duration of finasteride and minoxidil hair loss treatment and a one time alternative
Prostate enlargement
Physicians use finasteride for the treatment of BPH, informally known as an enlarged prostate. Finasteride may improve the symptoms associated with BPH such as difficulty urinating, getting up during the night to urinate, hesitation at the start of urination, and decreased urinary flow. It provides less symptomatic relief than alpha-1 blockers such as tamsulosin and symptomatic relief is slower in onset (six months or more of treatment with finasteride may be required to determine the therapeutic results of treatment). Symptomatic benefits are mainly seen in those with prostate volume > 40 cm3. In long-term studies finasteride but not alpha-1 inhibitors reduce the risk of acute urinary retention (−57% at 4 years) and the need for surgery (−54% at 4 years). If the drug is discontinued, any therapeutic benefits reverse within about 6–8 months.
Pattern hair loss
Finasteride is used to treat pattern hair loss (androgenetic alopecia) in men only. Treatment slows further hair loss and provides about 30% improvement in hair loss after six months of treatment, with effectiveness only persisting as long as the drug is taken. Finasteride has also been tested for pattern hair loss in women; the results were no better than placebo.
Excessive hair growth
Finasteride has been found to be effective in the treatment of hirsutism (excessive facial and/or body hair growth) in women. In a study of 89 women with hyperandrogenism due to persistent adrenarche syndrome, finasteride produced a 93% reduction in facial hirsutism and a 73% reduction bodily hirsutism after 2 years of treatment. Other studies using finasteride for hirsutism have also found it to be clearly effective.
Transgender women
Finasteride is sometimes used in hormone replacement therapy for transgender women in combination with a form of estrogen due to its antiandrogen properties. However, little clinical research of finasteride use for this purpose has been conducted and evidence of efficacy is limited.
Contraindications
Finasteride is not approved for use in women, especially due to risks of birth defects in a fetus. It is classified in the FDA pregnancy category X.
Adverse effects
A 2010 Cochrane review concluded that side effects from finasteride are rare when used for BPH. Compared with placebo, men taking finasteride are; however, at increased risk for impotence, erectile dysfunction, decreased libido, and ejaculation disorder for the first year of treatment. In this review the rates of these effects became indistinguishable from placebo after 2–4 years and these side effects usually got better over time. Another 2010 review found that when used for hair loss finasteride increased rates of sexual problems.
In men with prostatic hyperplasia the use of both a 5α-reductase inhibitor and a α2 adrenergic receptor blocker resulted in a greater risk of erectile dysfunction compared to either agent alone.
The FDA has added a warning to 5α-reductase inhibitors concerning an increased risk of high-grade prostate cancer, as the treatment of BPH lowers PSA (prostate-specific antigen), which could mask the development of prostate cancer. Although overall incidence of male breast cancer in clinical trials for finasteride 5 mg was not increased, there are post-marketing reports of breast cancer in association with its use. Available evidence does not provide clarity as to whether there is a causative relationship between finasteride and these cancers.
A 2015 meta analysis found that none of the clinical trials testing finasteride in hair loss had adequate safety reporting and did not provide sufficient information to establish the safety profile for finasteride as a treatment for hair loss. The study concluded the existing clinical trials of finasteride for hair loss provide very limited information on toxicity, are of poor quality, and seem to be systematically biased toward under-detection of adverse events. Moreover, the trials submitted to the FDA for approval for hair loss excluded most men who would normally be prescribed finasteride for androgenic alopecia.
Sexual function
Whether finasteride causes long-term sexual dysfunction in some men after stopping drug treatment is unclear. There are case reports of persistent diminished libido or erectile dysfunction after stopping the drug and the FDA has updated the label to inform people of these reports. A 2010 review found moderate quality evidence that finasteride increased the risk of sexual dysfunction, but not that people stopped using it because of sexual side effects.
When finasteride was originally approved for hair loss in 1997, the FDA approval review reported that it appears well tolerated, with the most common side effects being related to sexual function. In many people these side effects resolve if the medication is stopped and occasionally resolve even if the medication is continued. They additionally state "the sexual functioning questionnaire seems to have given a sensitive reflection of the disturbance on sexual functioning".
Mechanism of action
Finasteride is a 5α-reductase inhibitor, specifically the type II and III isoenzymes. By inhibiting 5α-reductase, finasteride prevents conversion of testosterone to dihydrotestosterone (DHT) by the type II and III isoenzymes, resulting in a decrease in serum DHT levels by about 65–70% and in prostate DHT levels by up to 85–90%, where expression of the type II isoenzyme predominates. Unlike triple inhibitors of all three isoenzymes of 5α-reductase like dutasteride which can reduce DHT levels in the entire body by more than 99%, finasteride does not completely suppress DHT production because it lacks significant inhibitory effects on the 5α-reductase type I isoenzyme, with 100-fold less affinity for I as compared to II.
By blocking DHT production, finasteride reduces androgen activity in the scalp. In the prostate, inhibition of 5α-reductase reduces prostate volume, which improves BPH and reduces risk of prostate cancer. Inhibition of 5α-reductase also reduces epididymal weight, and decreases motility and normal morphology of spermatozoa in the epididymis. Neurosteroids like 3α-androstanediol and allopregnanolone activate the GABAA receptor; because finasteride prevents the formation of neurosteroids, it may contribute to a reduction of GABAA activity (see also neurosteroidogenesis inhibitor). Reduction of GABAA receptor activation by these neurosteroids has been implicated in depression, anxiety, and sexual dysfunction.
In addition to inhibiting 5α-reductase, finasteride has also been found to competitively inhibit 5β-reductase (AKR1D1), although its affinity for the enzyme is substantially less than for 5α-reductase (an order of magnitude less than 5α-reductase type I) and hence is unlikely to be of clinical significance.
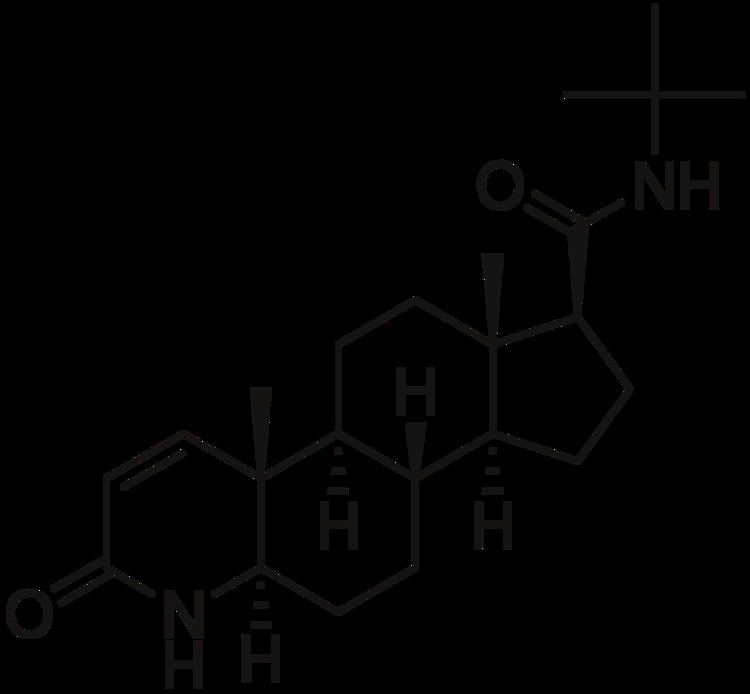
Chemistry
Finasteride is a 4-azasteroid analogue of testosterone and is lipophilic.
History
In 1974, Julianne Imperato-McGinley of Cornell Medical College in New York attended a conference on birth defects. She reported on a group of intersex children in the Caribbean who appeared sexually ambiguous at birth, and were initially raised as girls, but then grew external male genitalia and other masculine characteristic after onset of puberty. Her research group found these children shared a genetic mutation, causing deficiency of the 5α-reductase enzyme and male hormone dihydrotestosterone (DHT), which was found to have been the etiology behind abnormalities in male sexual development. Upon maturation, these individuals were observed to have smaller prostates which were underdeveloped, and were also observed to lack incidence of male pattern baldness.
In 1975, copies of Imperato-McGinley's presentation were seen by P. Roy Vagelos, who was then serving as Merck's basic-research chief. He was intrigued by the notion that decreased levels of DHT led to the development of smaller prostates. Dr. Vagelos then sought to create a drug which could mimic the condition found in these children to treat older men who were suffering from benign prostatic hyperplasia.
Finasteride was developed under the code name MK-906. In 1992, finasteride (5 mg) was approved by the U.S. Food and Drug Administration (FDA) for treatment of BPH, which Merck marketed under the brand name Proscar. In 1997, Merck was successful in obtaining FDA approval for a second indication of finasteride (1 mg) for treatment of MPB, which was marketed under the brand name Propecia.
Society and culture
The Food and Drug Administration advises that donation of blood or plasma be deferred for at least one month after taking the last dose of finasteride.
Harold Bornstein, Donald Trump's personal physician, stated Trump was taking finasteride to promote hair growth.
Athletics
From 2005 to 2009, the World Anti-Doping Agency banned finasteride because it was discovered that the drug could be used to mask steroid abuse. It was removed from the list effective January 1, 2009, after improvements in testing methods made the ban unnecessary. Athletes who used finasteride and were banned from international competition include skeleton racer Zach Lund, bobsledder Sebastien Gattuso, footballer Romário and ice hockey goaltender José Théodore.
Brand names
Drug trade names include Propecia, marketed for male pattern baldness (MPB), and Proscar, for benign prostatic hyperplasia (BPH); both are products of Merck & Co. There is 1 mg of finasteride in Propecia and 5 mg in Proscar. Merck's patent on finasteride for the treatment of BPH expired on June 19, 2006. Merck was awarded a separate patent for the use of finasteride to treat MPB. This patent expired in November 2013.
Controversy
Men in the US and Canada concerned about persistent sexual side effects "coined the phrase 'post finasteride syndrome', which they say is characterized by sexual, neurological, hormonal and psychological side effects that can persist in men who have taken finasteride for hair loss or an enlarged prostate". In 2012, a health advocacy group called the Post-Finasteride Syndrome Foundation was formed with the primary goal of finding a cure for the reported syndrome and a secondary goal of raising awareness. According to the company's 1Q2016 financial filing, Merck is a defendant in 1,385 product liability lawsuits which have been filed by customers alleging they have experienced persistent sexual side effects following cessation of treatment with finasteride.
