 | ||
Cardiac contractility modulation (CCM) is a treatment for patients with moderate to severe left ventricular systolic heart failure (NYHA class II–IV). The short- and long-term use of this therapy enhances both the strength of ventricular contraction and the heart’s pumping capacity by modulating (adjusting) the myocardial contractility. The CCM mechanism is based on stimulation of the cardiac muscle by non-excitatory electrical signals (NES). CCM treatment is delivered by a pacemaker-like device that applies the NES, adjusted to and synchronized with the electrical action in the cardiac cycle.
Contents
- Approval
- Indication
- Therapeutic gap
- Recommendations
- Efficacy
- Meta analyses
- Long Term Survival Studies
- General
- Contraindications
- Side effects
- Precautions
- Mechanism of action
- Composition
- CCM signals
- Implantation
- Maintenance
- Interactions with other electrical stimulation treatments
- Referral and Reimbursement
- History
- Research
- References
In CCM therapy, electrical stimulation is applied to the cardiac muscle during the absolute refractory period. In this phase of the cardiac cycle, electrical signals cannot trigger new cardiac muscle contractions, hence this type of stimulation is known as a non-excitatory stimulation. However, the electrical CCM signals increase the influx of calcium ions into the cardiac muscle cells (cardiomyocytes). In contrast to other electrical stimulation treatments for heart failure, such as pacemaker therapy or implantable cardioverter defibrillators (ICD), CCM does not affect the cardiac rhythm directly. Rather, the aim is to enhance the heart’s natural contraction (the native cardiac contractility) sustainably over long periods of time. Furthermore, unlike most interventions that increase cardiac contractility, CCM is not associated with an unfavorable increase in oxygen demand by the heart (measured in terms of Myocardial Oxygen Consumption or MVO2). This may be explained by the beneficial effect CCM has in improving cardiac efficiency. A meta-analysis in 2014 and an overview of device-based treatment options in heart failure in 2013 concluded that CCM treatment is safe, that it is generally beneficial to patients and that CCM treatment increases the exercise tolerance (ET) and quality of life (QoL) of patients. Furthermore, preliminary long-term survival data shows that CCM is associated with lower long-term mortality in heart failure patients when compared with expected rates among similar patients not treated with CCM.
Approval
Based on the results of clinical trials, CCM devices are approved and available for clinical use in all European Union countries and in Australia, Turkey, India and Hong Kong, as well as in other countries that recognize CE marking for medical devices.
At the present time, CCM therapy is not approved for clinical use in the United States. However, a study has been initiated in order to obtain FDA approval.
Indication
Based on the approval of CCM devices, cardiac contractility modulation is a treatment option for patients that are at least 18 years old who suffer from heart failure symptoms due to left ventricular systolic dysfunction (LVSD) despite adequate medical treatment. Further clinical research is required to identify which patient group within the scope of the device approval benefits most from CCM treatment.
Criteria for the classification of patients with left ventricular systolic heart failure include the severity of the disease based on functional parameters (NYHA classification), the average percentage of blood volume ejected by the left ventricle with each heart beat (left ventricular ejection fraction or LVEF) and the duration of the QRS complex seen in the electrocardiogram (ECG). Most clinical studies on CCM therapy have involved heart failure patients who were classified initially as NYHA Class II, III or IV and had a normal QRS duration (QRS duration ≤ 120 ms). The efficacy of CCM on patients in an earlier stage of heart failure has not yet been studied.
A subsequent evaluation study (subgroup analysis) has already suggested a particular patient group that responds exceptionally well to CCM therapy. The patients were characterized by a disease severity of NYHA class III and a left ventricular ejection fraction of ≥ 25%.
Although studies on CCM therapy have focused on patients with a normal QRS duration (i.e. ≤ 120 ms), it is possible to use CCM in patients who meet the treatment indication but who do not have a normal QRS duration. A preliminary study has previously shown that CCM may be safe and effective in such patients who have not responded to cardiac resynchronization therapy (CRT).
Therapeutic gap
Cardiac resynchronization therapy (CRT; also known as biventricular pacing) has proven to be an effective treatment in heart failure. However, CRT is generally recommended exclusively for patients with a preserved sinus rhythm and a prolonged QRS complex (≥ 120 ms) who also suffer from left bundle branch block (LBBB), or for patients without left bundle branch block but who have a preserved sinus rhythm and a QRS complex with a width of ≥ 150 ms. However, only 30-40% of all heart failure patients show such a prolonged QRS complex, and therefore the 60-70% of patients who have a normal QRS complex cannot be treated with CRT. In addition, around 30% of the patients eligible for CRT treatment do not respond to CRT.
Until recently, the only other available device-based treatment was the left ventricular assist device (LVAD). LVAD therapy is indicated in patients with severe illness and is associated with several hours of surgery (involving a cardiopulmonary bypass). It is usually considered as a therapy providing a “bridge to transplant” for heart failure patients classified as NYHA class IV, and is intended to support heart function until a heart transplant is received. Current research results suggest that the therapeutic gap described above could now be closed by CCM therapy. Additionally, a long-term study on CCM showed that the therapy was able to stop the common and prognostically unfavorable long-term prolongation of QRS duration in heart failure patients. This result was interpreted as signaling the safety of the treatment and as an indicator that patients could benefit from CCM therapy in the long term. If the QRS-stabilizing effect were to be confirmed in further studies, CCM would become the first device-based treatment for heart failure with the potential to halt QRS prolongation, a factor associated with a poor prognosis.
Recommendations
As of February 2015, no recommendations concerning the use of CCM in the treatment of heart failure are available from either national or international medical societies. This includes the guidelines issued by the European Society of Cardiology (ESC), which were most recently updated in 2012 and in most cases are endorsed by national cardiac societies in individual countries within the European Union.
This deficiency has been criticized by experts and has served as one of two cases brought forward in a request to discuss the assessment criteria of the ESC.
Efficacy
Cardiac contractility modulation has proven to be effective and safe in randomized controlled trials involving several hundred patients.
The nature and extent of the effect of CCM have been the subject of numerous investigations. Although various individual publications, as well as one of two meta-analyses, have presented CCM‘s efficacy and significant potential in treatment of heart failure, medical evaluation of the therapy efficacy is not yet complete. Scientists point out, however, that this was also the case for CRT therapy when it was first introduced, advocating the provision of CCM to suitable patients before further studies are completed.
To date (February 2015), there are at least two meta-analyses studying the efficacy of CCM therapy on heart failure, a large number of review articles (e.g.) and at least two survey articles on device-based treatments of advanced heart failure which address cardiac contractility modulation. Furthermore, there are more than 70 individual publications focusing specifically on CCM.
Further randomized controlled trials studying the effect of CCM on the progression of heart failure have been initiated and are currently (as of Feb 2015) recruiting patients.
Meta-analyses
Giallauria et al. evaluated the three randomized controlled trials (RCTs) currently available on CCM as a treatment for heart failure patients. The three trials included a total of 641 patients and assessed the effect of CCM either in comparison to a sham treatment or in comparison to the best medical treatment. In contrast to an earlier meta-analysis by Kwong et al. the study did not evaluate the data based on summarized results alone, but on the basis of the individual data sets of the 641 enrolled patients.
The study concluded that CCM significantly improved important markers of cardiac performance. These included the maximal oxygen uptake (peak VO2 or pVO2 – measured by ventilatory parameters during a cardiopulmonary exercise test), which is indicative of improved survival, and the 6-minute walk test. The quality of life of participating patients, measured by the Minnesota Living with Heart Failure Questionnaire (MLWHFQ), also improved significantly. However, both meta-analyses demanded additional and larger randomized controlled trials in order to evaluate the effect of CCM more precisely.
Giallauria et al. describe the success of cardiac contractility modulation and the further potential of the therapy. Particular emphasis is given to the possibility that CCM therapy may close the therapeutic gap in heart failure treatment if previous study outcomes are confirmed.
Long-Term Survival Studies
As of February 2015, the effect of CCM therapy on the long-term mortality rates of heart failure patients has not been studied in a randomized controlled trial. Some preliminary single-center studies have been reported though. Kuschyk et al. evaluated the long-term efficacy and survival of patients with CCM. Their analysis included 81 patients with a disease severity of NYHA class II, III or IV and a mean follow-up of around 3 years. The analysis compared the observed mortality rate with the prediction of the Meta-analysis Global Group in Chronic Heart Failure (MAGGIC) model which is based on the records of over 39,000 heart failure patients. Unlike a previous long-term outcome study of CCM, this study was not limited by a widely heterogeneous group of patients.
Following long-term observation, the study concluded that CCM improved quality of life, exercise tolerance, NYHA class, left ventricular ejection fraction (LVEF) and brain natriuretic peptide (BNP) levels. Mortality rates were significantly lower than predicted at year 1, and lower than predicted but not statistically significant at year 3.
General
Heart failure is a chronic disease that usually progresses gradually. The rate of progression and the degree of symptoms of the disease varies between different patients. CCM therapy aims to treat heart failure through a medium- to long-term treatment, over the course of weeks and months.
According to large implanting clinics, after the implantation wound is healed, the lifestyle of a patient is not restricted by the implanted device. Leisure, travel (by car, train, ship or plane), hobbies and sex life will not be restricted. The patient may perceive an improved capacity for these activities and overall enhanced performance and exercise capacity in response to the actual therapy.
Contraindications
The most important contraindication in CCM treatment is permanent and long-standing persistent atrial fibrillation. The signal application in current CCM devices is timed and triggered according to the electrical activity of the atrium. In atrial fibrillation, electrical activity in the atrium is severely disturbed and is therefore not a reliable basis for the triggering of CCM signals. This also applies to other diseases involving severe disturbance in electrical atrial sensing. Requests have been raised in scientific literature for an improved CCM algorithm which would allow CCM therapy to be delivered independently from any atrial signal. A pioneering study has already shown that an improved CCM algorithm could make CCM an effective treatment for patients with persistent atrial fibrillation.
Other irregular rhythms, including frequent premature ventricular contractions (ventricular extra systoles) or a distinct signal transduction disorder in the heart (untreated AV block of more than 300 ms), may also represent contraindications. CRT treatment should be considered in lieu of CCM in patients with left bundle branch block (LBBB) and a QRS duration of over 120 ms, or when the QRS duration is greater than 150 ms and independent of LBBB.
As with conventional pacemaker therapy, the CCM device cannot be implanted if the leads cannot be positioned appropriately in the heart. In cases where there is an artificial heart valve between the right atrium and ventricle (a mechanical prosthetic tricuspid valve), the valve function could be greatly affected by the ventricular leads. In some instances it may be impossible to guide the leads thorough the main veins in the upper half of the body to the heart due to venous thrombosis, for example VVI pacemakers, in the case of 100% stimulation, are also contraindicated.
Side effects
The most frequently encountered adverse events related to CCM therapy are lead fracture or lead dislodgement. Other reported complications include:
These side effects are similar to those that occur with other electrical stimulation therapies, such as pacemakers, CRT devices or ICD devices. Furthermore, recorded complications did not differ between patients with activated CCM devices and patients with deactivated CCM devices.
Overall, CCM treatment was demonstrated to have no negative impact on health markers.
Precautions
Similarly to patients with other electrical stimulation devices, patients with a CCM device must follow certain precautions arising from the device implantation and its function.
Mechanism of action
The mechanism of action of CCM has been subject to continuous research since its initial discovery. Based on animal testing and experiments on human myocardial tissue obtained by biopsies, essential parts of the mechanism of action have been identified. According to current understanding (as of February 2015), the mechanism of action of CCM may be summarized in the following manner: The CCM signals applied during the electrical non-excitatory state of the cardiac muscle cells (the absolute refractory period) cause an increase in myocyte calcium in the cytosol during systole. This increases the muscle contraction strength. Additionally, within minutes, cell metabolism and gene expression, which are typically abnormal in heart failure, improve towards their normal state. This beneficial effect occurs initially only in the area adjacent to the electrodes, but with time also spreads to remote areas of the cardiac muscle. CCM therefore restores the structure and function of damaged cells back towards their normal state. In some cases, disease-related changes in the ventricular heart structure can be partially reversed by CCM through a process known as reverse remodeling of the heart.
Composition
CCM devices are similar in structure to other implantable devices used for electrical stimulation of the heart, such as pacemakers or implantable cardioverter defibrillators (ICDs). The currently available CCM system (as of February 2015) consists of four components, as described below.
CCM signals
Cardiac contractility modulation (CCM) acts on the cardiac muscle during the absolute refractory period via specific electrical signals generated by the pulse generator. Signals are applied approximately 30 ms after onset of the QRS complex (normal total QRS duration: ≤ 120 ms). The signal consists of two bi-phasic pulses with an amplitude of ± 7.7 V and with a total signal duration of about 20 ms.
Since CCM signals are delivered during the absolute refractory period of the cardiac cycle, they neither trigger muscle contractions nor cause activation of additional muscle fibers. Accordingly, the heart’s electrical and mechanical activation sequence remains unchanged. As CCM signals contain around 50-100 times more energy than signals from conventional pacemakers, their peaks can easily be recognized in an electrocardiogram (ECG).
Implantation
The implantation of the pulse generator (IPG) and the corresponding CCM delivery leads is comparable to a pacemaker implantation. This sort of intervention is carried out approximately one million times per year worldwide. The implantation procedure is minimally invasive, lasts roughly 40 minutes and is usually carried out under local anesthesia. However, patients should fast ahead of the implantation due to possible complications which may result in a longer procedure and/or require longer anesthesia.
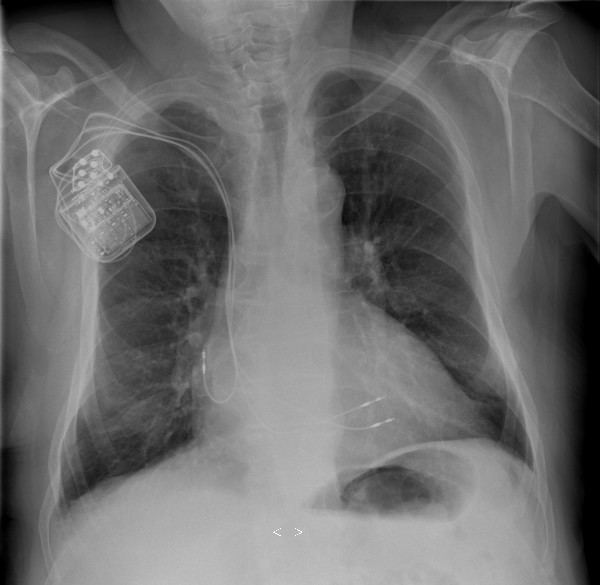
First, the doctor checks the function of the pulse generator and the leads, before positioning the leads in the heart. The positioning of the leads is verified by X-ray imaging and by the measurement of voltage and electric current through the leads (lead impedance).
Following successful positioning, the leads are connected to the pulse generator. A pocket is formed under the skin or chest muscle below the clavicle of the patient in order to implant the pulse generator. The IPG is inserted in the pocket and its function is tested. If the patient happens to have a pacemaker or implantable cardioverter defibrillator, the doctor and/or a trained technician ensures that there is no interference between the two devices by performing a “crosstalk check”. Finally, the pocket is sutured and the wound is bandaged.
Following implantation, patients are usually monitored for a period of time to ensure that the CCM device functions properly before being discharged from hospital. Once the healing process is complete, there is no need for any precautionary measures concerning water contact with the device as it is completely under the skin. It is not problematic for patients to shower or swim with the device, providing their health condition permits these activities.
After discharge, treatment is continued under the care of an outpatient cardiologist. Check-ups are carried out after a few days, after a few weeks and then following the treating cardiologist’s recommendation.
Maintenance
Aside from periodic battery charging (charging takes approximately 1 hour per week) and the surgical replacement needed after expiration of its battery life, CCM devices are maintenance-free. Nevertheless, the settings and function of the system must be checked and may be adjusted by a cardiologist from time to time. Battery chargers are equipped with a patient alert system which warns the patient to contact a physician in case of device malfunction or other functional abnormalities, such as low therapy delivery.
Interactions with other electrical stimulation treatments
Adverse interactions between CCM therapy and other electrical stimulation therapies have not been observed to date. Studies have shown that CCM therapy can be carried out simultaneously with a pacemaker and/or CRT treatment, and with or without an implantable cardioverter defibrillator (ICD), without causing disturbance to the individual therapies. As a result of these findings, the development of devices combining CCM and cardioverter defibrillation has been requested by some physicians in order to spare patients from the need for additional separate electrical stimulation devices and implantation procedures.
Referral and Reimbursement
CCM treatment is usually recommended by a cardiologist and the device may be implanted by a cardiac electrophysiologist. The treatment cost is covered both by statutory as well as private health insurance in Germany, Switzerland, Italy and Austria. The appropriate comparator for CCM therapy is failed Optimal Medical Therapy (OMT).
History
Development of cardiac contractility modulation began in the late 1990s. Studies on individual cardiac muscle cells using a patch-clamp technique had already shown, in 1969, that a voltage applied during the absolute refractory period through leads between the interior of the cell and its outside environment increased the calcium influx through the cell membrane and improved the contraction of cardiac muscle cells. In 2001, scientists observed that a similar effect occurs even if the voltage is applied exclusively outside the cardiac muscle cells. Additionally, it was observed that therapeutically useful effects on the cardiac muscle were achieved if the electrical signals were applied not only to single cells but to large areas using larger leads, as used in conventional cardiac pacemakers. The contractility of both a healthy heart and a damaged heart could be increased through application of appropriate signals during the absolute refractory period of the cardiac muscle cells.
An implantable CCM device was received by a patient for the first time in 2001. The first study on the therapeutic effects of CCM in humans was presented in 2004. To date, more than 2,000 heart failure patients have been treated with CCM worldwide, including 641 patients under the study conditions recommended by the Cochrane Collaboration as being necessary for inclusion in a meta-analysis.
Research
CCM technology does not only affect the function of cardiac tissue, but can also be used to affect the function of other muscle tissue. Approval has already been given for clinical use of the technology in treatment of the stomach to support weight loss and better control of sugar metabolism in obese patients with diabetes mellitus type 2.
