eMedicine med/10 | MeSH D015823 | |
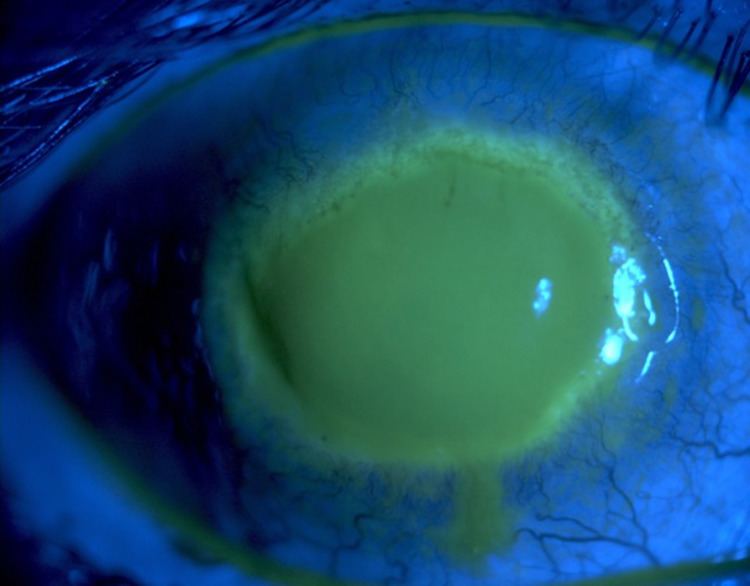 | ||
Acanthamoeba keratitis is a rare disease in which amoebae invade the cornea of the eye. It may result in permanent visual impairment or blindness.
Contents
Life cycle
Species within the genus Acanthamoeba are generally free-living trophozoites. These trophozoites are relatively ubiquitous and can live in, but are not restricted to, tap water, freshwater lakes/rivers and soil. Besides the trophozoite stage, a cyst stage may also be present. Both of these stages are usually uninucleated and reproduce by the means of binary fission. When the environment poses conditions that are not favorable, the trophozoites encyst to produce double-walled cysts.
Causes
In the United States, it is nearly always associated with contact lens use, as Acanthamoeba can survive in the space between the lens and the eye. To prevent the condition, contact lenses must be properly disinfected before wearing, and should be removed when swimming or surfing.
However, there have been many cases of Acanthamoeba in those who don't wear contact lenses, elsewhere in the world.
Diagnosis
To detect Acanthamoeba on a contact lens in a laboratory, the contact lens is placed on a non-nutrient agar saline plate seeded with a gram-negative bacteria such as E. coli. If Acanthamoeba are present, they will reproduce readily and become visible on the plate under 10-20X objective on an inverted microscope. Polymerase chain reaction can also be used to confirm a diagnosis of Acanthamoeba keratitis, especially when contact lenses are not involved. Acanthameoba is also characterized by a brawny edema and hazy view into the anterior chamber. Late stages of the disease also produces a ring shaped corneal ulcer. Signs and symptoms include severe pain, severe keratitis (similar to stromal herpetic disease), corneal perineuritis, and ring ulcer (late in the disease process).
Prevalence
A recently published study was conducted by an institution in Austria. The goal was to diagnose Acanthamoeba keratitis to give an overview of proven cases of Acanthamoeba infections in Austria during the past 20 years. Samples of patients suspected to have Acanthamoeba keratitis were screened by using gram negative bacteria cultures and/or PCR and the detected amoebae were genotyped. Over the course of the testing, a total of 154 cases of Acanthamoeba keratitis were diagnosed. The age of the positive tests ranged from 8 to 82 years old and 58% of the patients were female. More importantly, the data showed that 89% of the infected patients were contact lens wearers and 19% of the patients required a corneal transplant.
Prevention
According to the American Optometric Association, the following steps can be taken to prevent Acanthamoeba keratitis:
Treatment
One treatment used is polyhexamethylene biguanide, PHMB.
Propamidine isethionate has also shown some effectiveness.
Another possible agent is chlorhexidine.
Keratoplasty may sometimes be required.
A combined regimen of propamidine, miconazole nitrate, and neomycin has also been suggested.
A recent Cochrane review found one study that compared the effectiveness of chlorhexidine eye drops against PHMB eye drops, for eyes with Acanthamoeba keratitis. While the differences between treatments were not statistically significant, the review found that 86% of eyes treated with chlorhexidine eye drops reported a resolution of infection, compared to 78% of eyes treated with PHMB eye drops. The study also found that 71% of eyes treated with chlorhexidine eye drops reported improved visual acuity after treatment, compared to 57% of eyes in the PMGB group; these results were also not significant.
