Trade names Micardis MedlinePlus a601249 ATC code C09CA07 (WHO) Molar mass 514.617 g/mol | AHFS/Drugs.com Monograph Routes ofadministration Oral CAS ID 144701-48-4 | |
 | ||
Pregnancycategory AU: DUS: D (Evidence of risk) | ||
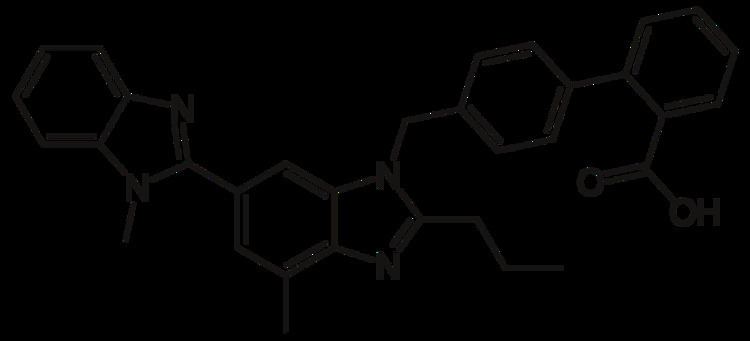
Mechanism of action of telmisartan
Telmisartan (INN) /tɛlmɪˈsɑːrtən/ is an angiotensin II receptor antagonist (angiotensin receptor blocker, ARB) used in the management of hypertension. It was discovered by Boehringer Ingelheim and launched in 1999 as Micardis.
Contents
- Mechanism of action of telmisartan
- Some common side effects of telmisartan
- Medical uses
- Contraindications
- Side effects
- Interactions
- Mechanism of action
- Pharmacokinetics
- ONTARGET
- TRANSCEND
- PRoFESS
- Cancer
- Diabetes type II
- References
In January 2014, Actavis as generic version of Micardis got appoval from FDA.
Some common side effects of telmisartan
Medical uses
Telmisartan is indicated in the treatment of essential hypertension.
Contraindications
Telmisartan is contraindicated during pregnancy. Like other drugs affecting the renin-angiotensin system (RAS), telmisartan can cause birth defects, stillbirths, and neonatal deaths. It is not known whether the drug passes into the breast milk. Also it is contraindicated in bilateral renal artery stenosis in which it can cause renal failure.
Side effects
Side effects are similar to other angiotensin II receptor antagonists and include tachycardia and bradycardia (fast or slow heartbeat), hypotension (low blood pressure), edema (swelling of arms, legs, lips, tongue, or throat, the latter leading to breathing problems), and allergic reactions.
Interactions
Due to its mechanism of action, telmisartan increases blood potassium levels. Combination with potassium preparations or potassium-sparing diuretics could cause hyperkalaemia (excessive potassium levels). Combination with NSAIDs, especially in patients with impaired kidney function, has a risk of causing (usually reversible) kidney failure.
Mechanism of action
Telmisartan is an angiotensin II receptor blocker that shows high affinity for the angiotensin II receptor type 1 (AT1), with a binding affinity 3000 times greater for AT1 than AT2.
In addition to blocking the RAS, telmisartan acts as a selective modulator of peroxisome proliferator-activated receptor gamma (PPAR-γ), a central regulator of insulin and glucose metabolism. It is believed that telmisartan’s dual mode of action may provide protective benefits against the vascular and renal damage caused by diabetes and cardiovascular disease (CVD).
Telmisartan's activity at the peroxisome proliferator-activated receptor delta (PPAR-δ) receptor has prompted speculation around its potential as a sport doping agent as an alternative to GW 501516. Telmisartan activates PPAR-δ receptors in several tissues.
Pharmacokinetics
The substance is quickly but to varying degrees absorbed from the gut. The average bioavailability is about 50% (42–100%). Food intake has no clinically relevant influence on the kinetics of telmisartan. Plasma protein binding is over 99.5%, mainly to albumin and alpha-1-acid glycoprotein. It has the longest half-life of any ARB (24 hours) and the largest volume of distribution among ARBs (500 liters). Less than 3% of telmisatran is inactivated by glucuronidation in the liver, and over 97% are eliminated in unchanged form via bile and faeces.
ONTARGET
The Ongoing Telmisartan Alone and in combination with Ramipril Global Endpoint Trial (ONTARGET) was one of the largest ARB clinical studies ever undertaken; 25,620 patients from 733 centres in 41 countries were randomised for 5.5 years of treatment of either telmisartan, the ACE inhibitor ramipril or a combination of the two. The study aimed to investigate the role of telmisartan in cardiovascular (CV) protection through the primary composite outcome of death from CV causes, myocardial infarction, stroke or hospitalization for heart failure, in high CV risk patients.
The study showed telmisartan was as effective as ramipril but with lower rates of cough and angioedema, which led to fewer discontinuations. The combination group experienced similar efficacy, but with increased risk of hypotensive symptoms. Moreover, in a patient population selected to tolerate ACE inhibitors, telmisartan was shown to be better tolerated and associated with higher treatment compliance than ramipril.
TRANSCEND
As part of the ONTARGET study, patients who could not tolerate ACE inhibitors were randomly assigned to receive either telmisartan or placebo as part of the Telmisartan Randomized Assessment Study in ACE Intolerant Subjects with Cardiovascular Disease (TRANSCEND) study. An accompanying editorial comments: "Overall, data supporting use of angiotensin-receptor blockers to prevent vascular events in various cardiovascular groups, other than heart failure, are incomplete. TRANSCEND's results challenge the non-inferiority shown in ONTARGET and suggest no more than a modest effect, if any at all."
PRoFESS
The Prevention Regimen For Effectively Avoiding Second Strokes (PRoFESS) study investigated therapy with telmisartan initiated soon after an ischemic stroke and continued for 2.5 years. This treatment did not significantly lower the rate of recurrent stroke, major cardiovascular events, or diabetes.
Cancer
Telmisartan has been found to have activity against a variety of cancers in vitro, including prostate, renal, colon, leukemia, and ovarian cancer. The mechanisms of telmisartan's anti-cancer activity have been found to include up-regulation of proliferator-activated-receptor (PPAR) pathway, Bcl-2, and caspase activation.
Diabetes type II
According to a study with 18 patients, telmisartan can replace valsartan and candesartan for hypertensive patients with have also diabetes type II because telmisartan has additional advantages of insulin sensitivity and antiatherosclerosis through probably its effects on PPAR-y.
