MeSH D006965 | MedlinePlus 003441 | |
 | ||
Hyperplasia (from ancient Greek ὑπέρ huper, "over" + πλάσις plasis, "formation"), or hypergenesis, is an increase in the amount of organic tissue that results from cell proliferation. It may lead to the gross enlargement of an organ and the term is sometimes confused with benign neoplasia or benign tumor.
Contents
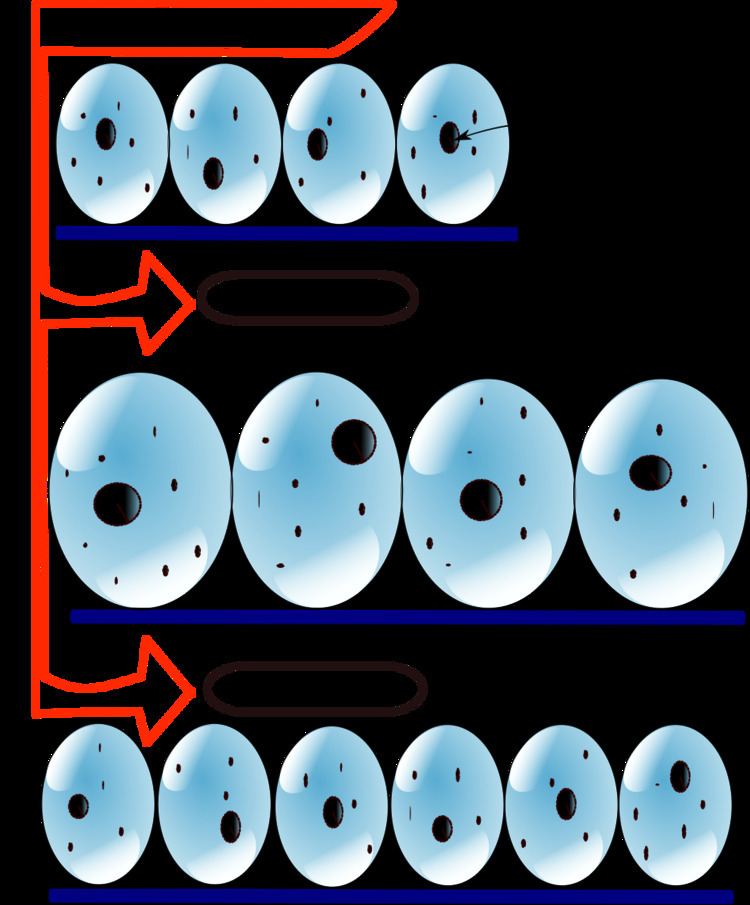
Hyperplasia is a common preneoplastic response to stimulus. Microscopically, cells resemble normal cells but are increased in numbers. Sometimes cells may also be increased in size (hypertrophy). Hyperplasia is different from hypertrophy in that the adaptive cell change in hypertrophy is an increase in the size of cells, whereas hyperplasia involves an increase in the number of cells.
Signs and symptoms
Hyperplasia is considered to be a physiological (normal) response to a specific stimulus, and the cells of a hyperplastic growth remain subject to normal regulatory control mechanisms. However, hyperplasia can also occur as a pathological response, if an excess of hormone or growth factor is responsible for the stimuli. Similarly to physiological hyperplasia, cells that undergo pathologic hyperplasia are controlled by growth hormones, and cease to proliferate if such stimuli are removed. This differs from neoplasia (the process underlying cancer and benign tumors), in which genetically abnormal cells manage to proliferate in a non-physiological manner which is unresponsive to normal stimuli. That being said, the effects caused by pathologic hyperplasia can provide a suitable foundation from which neoplastic cells may develop.
Examples
Some of the more commonly known clinical forms of hyperplasia, or conditions leading to hyperplasia, are:
Causes
Hyperplasia may be due to any number of causes, including increased demand (for example, proliferation of basal layer of epidermis to compensate skin loss), chronic inflammatory response, hormonal dysfunctions, or compensation for damage or disease elsewhere. Hyperplasia may be harmless and occur on a particular tissue. An example of a normal hyperplastic response would be the growth and multiplication of milk-secreting glandular cells in the breast as a response to pregnancy, thus preparing for future breast feeding.
Perhaps the most interesting and potent effect IGF has on the human body is its ability to cause hyperplasia, which is an actual splitting of cells. By contrast, hypertrophy is what occurs, for example, to skeletal muscle cells during weight training and steroid use and is simply an increase in the size of the cells. With IGF use, one is able to cause hyperplasia which actually increases the number of muscle cells present in the tissue. Weight training with or without anabolic steroid use enables these new cells to mature in size and strength. It is theorized that hyperplasia may also be induced through specific power output training for athletic performance, thus increasing the number of muscle fibers instead of increasing the size of a single fiber.
Diagnosis
In the case of endometrial hyperplasia usually a Pap smear is done, also a biopsy during the pelvic examination, may be done of the individuals endometrial tissue. You may want to consult your doctor for further examination. In regards to Cushing's disease, the diagnosis of salivary cortisol in an elevated level around "late-night" is a way to detect it in many patients.
Treatment
The treatment of hyperplasia would consist upon which; in the case of benign prostate hyperplasia the combination of alpha-1-receptor blockers and 5-alpha-reductase inhibitors are effective.
