 | ||
Female hysteria was once a common medical diagnosis, reserved exclusively for women, that is no longer recognized by medical authorities as a medical disorder. Its diagnosis and treatment were routine for hundreds of years in Western Europe. Hysteria of both genders was widely discussed in the medical literature of the nineteenth century. Women considered to have had it exhibited a wide array of symptoms, including faintness, nervousness, sexual desire, insomnia, fluid retention, heaviness in the abdomen, shortness of breath, irritability, loss of appetite for food or sex, and a "tendency to cause trouble".
Contents
In extreme cases, the woman may have been forced to enter an insane asylum or to have undergone surgical hysterectomy.
Early history
The history of hysteria can be traced to ancient times. In ancient Greece, it was described in the gynecological treatises of the Hippocratic Corpus, which dates back to the 5th and 4th centuries BC. Plato's dialogue Timaeus compares a woman's uterus to a living creature that wanders throughout a woman's body, "blocking passages, obstructing breathing, and causing disease". The concept of a pathological wandering womb was later viewed as the source of the term hysteria, which stems from the Greek cognate of uterus, ὑστέρα (hystera).
Another cause was thought to be the retention of a supposed female semen, thought to have mingled with male semen during intercourse. The female semen was believed to have been stored in the womb. Hysteria was referred to as "the widow's disease", because the female semen was believed to turn venomous if not released through regular climax or intercourse.
Nineteenth century
In 1859, a physician named George Taylor claimed that a quarter of all women suffered from hysteria. George Beard, a physician who catalogued seventy-five pages of possible symptoms of hysteria and yet called his list incomplete, claimed that almost any ailment could fit the diagnosis. Physicians thought that the stress associated with the typical female life at the time caused civilized women to be both more susceptible to nervous disorders and to develop faulty reproductive tracts. In the United States, such diagnosed disorders in women provided a step forward for the US to be medically on the same advancement level as Europe. One American physician expressed pleasure in the fact that the country was "catching up" to Europe in the prevalence of hysteria.
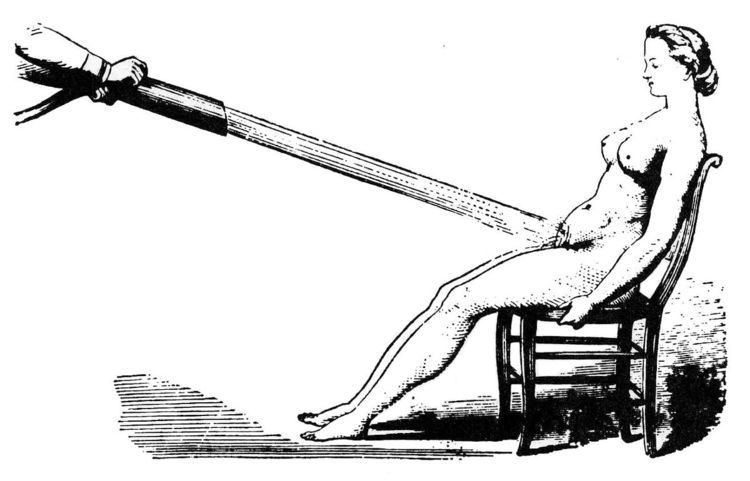
Rachel Maines hypothesized that doctors from the classical era up until the early 20th century commonly treated hysteria by masturbating female patients to orgasm (termed "hysterical paroxysm"), and that the inconvenience of this may have driven the early development of and the market for the vibrator. Although Maines's theory that hysteria was treated by masturbating female patients to orgasm is widely repeated in the literature on female anatomy and sexuality, some historians dispute Maines's claims about the prevalence of this treatment for hysteria and about its relevance to the invention of the vibrator, describing them as a distortion of the evidence or that it was only relevant to an extremely narrow group. Maines has said that her theory should be treated as a hypothesis rather than a fact.
Decline
During the early twentieth century, the number of women diagnosed with female hysteria sharply declined. This decline has been attributed to many factors. Some medical authors claim that the decline was due to laypeople gaining a greater understanding of the psychology behind conversion disorders such as hysteria.
With so many possible symptoms, hysteria was often considered a catchall diagnosis where any unidentifiable ailment could be assigned. As diagnostic techniques improved, the number of ambiguous cases that might have been attributed to hysteria declined. For instance, before the introduction of electroencephalography, epilepsy was frequently confused with hysteria. Many cases that had previously been labeled hysteria were reclassified by Sigmund Freud as anxiety neuroses.
Today, female hysteria is no longer a recognized illness, but different manifestations of hysteria are recognized in other conditions such as schizophrenia, borderline personality disorder, conversion disorder, and anxiety attacks.
