Latin nervus facialis Dorlands/Elsevier n_05/12565770 FMA 50868 | MeSH A08.800.800.120.250 TA A14.2.01.099 | |
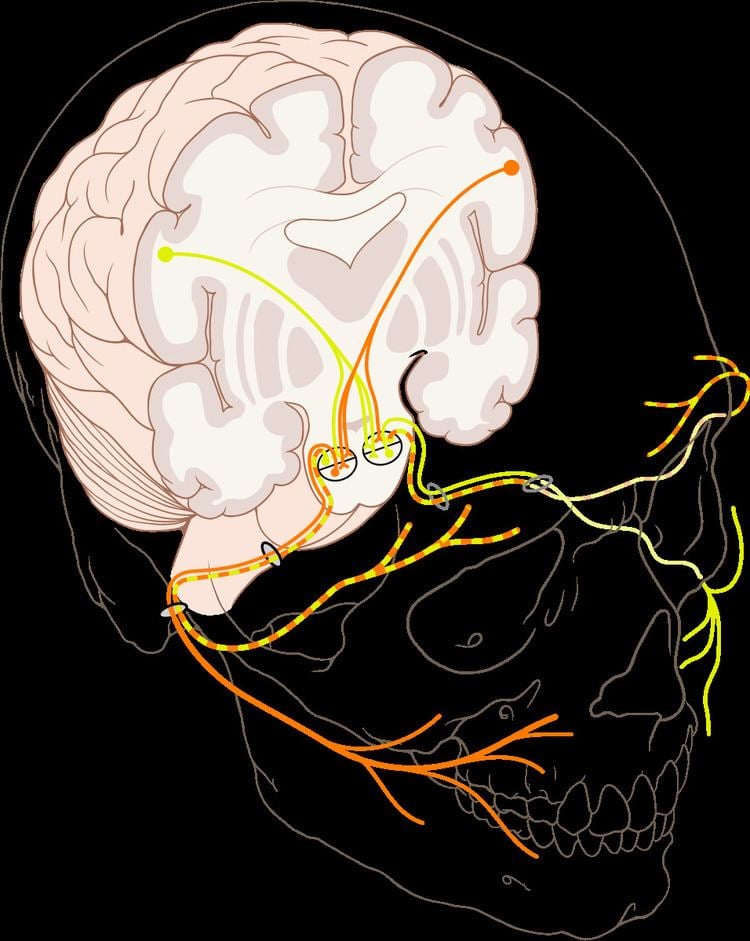 | ||
The facial nerve is the seventh cranial nerve, or simply cranial nerve VII. It emerges from the brainstem between the pons and the medulla, controls the muscles of facial expression, and functions in the conveyance of taste sensations from the anterior two-thirds of the tongue and oral cavity. It also supplies preganglionic parasympathetic fibers to several head and neck ganglia.
Contents
Structure
The path of the facial nerve can be divided into six segments.
- intracranial (cisternal) segment
- meatal segment (brainstem to internal auditory canal)
- labyrinthine segment (internal auditory canal to geniculate ganglion)
- tympanic segment (from geniculate ganglion to pyramidal eminence)
- mastoid segment (from pyramidal eminence to stylomastoid foramen)
- extratemporal segment (from stylomastoid foramen to post parotid branches)
- The motor part of the facial nerve arises from the facial nerve nucleus in the pons while the sensory and parasympathetic parts of the facial nerve arise from the intermediate nerve.
- From the brain stem, the motor and sensory parts of the facial nerve join together and traverse the posterior cranial fossa before entering the petrous temporal bone via the internal auditory meatus. Upon exiting the internal auditory meatus, the nerve then runs a tortuous course through the facial canal, which is divided into the labyrinthine, tympanic, and mastoid segments.
- The labyrinthine segment is very short, and ends where the facial nerve forms a bend known as the geniculum of the facial nerve ("genu" meaning knee), which contains the geniculate ganglion for sensory nerve bodies. The first branch of the facial nerve, the greater superficial petrosal nerve, arises here from the geniculate ganglion. The greater petrosal nerve runs through the pterygoid canal and synapses at the pterygopalatine ganglion. Post synaptic fibers of the greater petrosal nerve innervate the lacrimal gland.
- In the tympanic segment, the facial nerve runs through the tympanic cavity, medial to the incus.
- The pyramidal eminence is the second bend in the facial nerve, where the nerve runs downward as the mastoid segment. In the temporal part of the facial canal, the nerve gives rise to the stapedius and chorda tympani. The chorda tympani supplies taste fibers to the anterior two thirds of the tongue, and also synapses with the submandibular ganglion. Postsynaptic fibers from the submandibular ganglion supply the sublingual and submandibular glands.
- Upon emerging from the stylomastoid foramen, the facial nerve gives rise to the anterior auricular branch. The facial nerve then passes through the parotid gland, which it does not innervate, to form the parotid plexus, which splits into five branches innervating the muscles of facial expression (temporal, zygomatic, buccal, marginal mandibular, cervical).
Intracranial branches
Extracranial branches
Distal to stylomastoid foramen, the following nerves branch off the facial nerve:
Intra operatively the facial nerve is recognized at 3 constant landmarks:
- At the tip of tragal cartilage where the nerve is 1cm deep and inferior
- At the posterior belly of digastric by tracing this backwards to the tympanic plate the nerve can be found between these two structures
- By locating the posterior facial vein at the inferior aspect of the gland where the marginal branch would be seen crossing it.
- lateral semicircular canal
- foot of incus
Nucleus
The cell bodies for the facial nerve are grouped in anatomical areas called nuclei or ganglia. The cell bodies for the afferent nerves are found in the geniculate ganglion for taste sensation. The cell bodies for muscular efferent nerves are found in the facial motor nucleus whereas the cell bodies for the parasympathetic efferent nerves are found in the superior salivatory nucleus.
Embryology
The facial nerve is developmentally derived from the second pharyngeal arch, or branchial arch. The second arch is called the hyoid arch because it contributes to the formation of the lesser horn and upper body of the hyoid bone (the rest of the hyoid is formed by the third arch). The facial nerve supplies motor and sensory innervation to the muscles formed by the second pharyngeal arch, including the muscles of facial expression, the posterior belly of the digastric, stylohyoid and stapedius. The motor division of the facial nerve is derived from the basal plate of the embryonic pons, while the sensory division originates from the cranial neural crest.
Although the anterior two thirds of the tongue are derived from the first pharyngeal arch, which gives rise to cranial nerve V, not all innervation of the tongue is supplied by CN V. The lingual branch of the mandibular division (V3) of CN V supplies non-taste sensation (pressure, heat, texture) from the anterior part of the tongue via general visceral afferent fibers. Nerve fibers for taste are supplied by the chorda tympani branch of cranial nerve VII via special visceral afferent fibers.
Facial expression
The main function of the facial nerve is motor control of all of the muscles of facial expression. It also innervates the posterior belly of the digastric muscle, the stylohyoid muscle, and the stapedius muscle of the middle ear. All of these muscles are striated muscles of branchiomeric origin developing from the 2nd pharyngeal arch.
Facial sensation
In addition, the facial nerve receives taste sensations from the anterior two-thirds of the tongue via the chorda tympani; taste sensation is sent to the gustatory portion (superior part) of the solitary nucleus. General sensation from the anterior two-thirds of tongue are supplied by afferent fibers of the third division of the fifth cranial nerve (V-3). These sensory (V-3) and taste (VII) fibers travel together as the lingual nerve briefly before the chorda tympani leaves the lingual nerve to enter the tympanic cavity (middle ear) via the petrotympanic fissure. It joins the rest of the facial nerve via the canaliculus for chorda tympani. The facial nerve then forms the geniculate ganglion, which contains the cell bodies of the taste fibers of chorda tympani and other taste and sensory pathways. From the geniculate ganglion, the taste fibers continue as the intermediate nerve which goes to the upper anterior quadrant of the fundus of the internal acoustic meatus along with the motor root of the facial nerve. The intermediate nerve reaches the posterior cranial fossa via the internal acoustic meatus before synapsing in the solitary nucleus.
The facial nerve also supplies a small amount of afferent innervation to the oropharynx below the palatine tonsil. There is also a small amount of cutaneous sensation carried by the nervus intermedius from the skin in and around the auricle (outer ear).
Other
The facial nerve also supplies parasympathetic fibers to the submandibular gland and sublingual glands via chorda tympani. Parasympathetic innervation serves to increase the flow of saliva from these glands. It also supplies parasympathetic innervation to the nasal mucosa and the lacrimal gland via the pterygopalatine ganglion. The parasympathetic fibers that travel in the facial nerve originate in the superior salivary nucleus.
The facial nerve also functions as the efferent limb of the corneal reflex.
Functional components
The facial nerve carries axons of type GSA, general somatic afferent, to skin of the posterior ear.
The facial nerve also carries axons of type GVE, general visceral efferent, which innervate the sublingual, submandibular, and lacrimal glands, also mucosa of nasal cavity.
Axons of type SVE, special visceral efferent, innervate muscles of facial expression, stapedius, the posterior belly of digastric, and the stylohyoid.
The axons of type SVA, special visceral afferent, provide taste to the anterior two-thirds of tongue via chorda tympani.
Finally, the facial nerve also carries axons of type GVA, general visceral afferent, which provide sensation to the soft palate and parts of the nasal cavity.
Palsy
People may suffer from acute facial nerve paralysis, which is usually manifested by facial paralysis. Bell's palsy is one type of idiopathic acute facial nerve paralysis, which is more accurately described as a multiple cranial nerve ganglionitis that involves the facial nerve, and most likely results from viral infection and also sometimes as a result of Lyme disease. Iatrogenic Bell's Palsy may also be as a result of an incorrectly placed dental local-anesthetic (Inferior alveolar nerve block). Although giving the appearance of a hemi-plegic stroke, effects dissipate with the drug. When the facial nerve is permanently damaged due to a birth defect, trauma, or other disorder, surgery including a cross facial nerve graft or masseteric facial nerve transfer may be performed to help regain facial movement. Facial nerve decompression surgery is also sometimes carried out in certain cases of facial nerve compression.
Examination
Voluntary facial movements, such as wrinkling the brow, showing teeth, frowning, closing the eyes tightly (inability to do so is called lagophthalmos) , pursing the lips and puffing out the cheeks, all test the facial nerve. There should be no noticeable asymmetry.
In an UMN lesion, called central seven, only the lower part of the face on the contralateral side will be affected, due to the bilateral control to the upper facial muscles (frontalis and orbicularis oculi).
Lower motor neuron lesions can result in a CNVII palsy (Bell's palsy is the idiopathic form of facial nerve palsy), manifested as both upper and lower facial weakness on the same side of the lesion.
Taste can be tested on the anterior 2/3 of the tongue. This can be tested with a swab dipped in a flavoured solution, or with electronic stimulation (similar to putting your tongue on a battery).
Corneal reflex. The afferent arc is mediated by the General Sensory afferents of the Trigeminal Nerve. The efferent arc occurs via the Facial Nerve. The reflex involves consensual blinking of both eyes in response to stimulation of one eye. This is due to the Facial Nerve's innervation of the muscles of facial expression, namely Orbicularis oculi, responsible for blinking. Thus, the corneal reflex effectively tests the proper functioning of both Cranial Nerves V and VII.
