Specialty emergency medicine ICD-9-CM 831 MeSH D012783 | ICD-10 S43.0 DiseasesDB 31231 | |
 | ||
eMedicine orthoped/440 radio/630 sports/152 | ||
A dislocated shoulder occurs when the humerus separates from the scapula at the shoulder joint (glenohumeral joint). The shoulder joint has the greatest range of motion of any joint, at the cost of low joint stability, and it is therefore particularly susceptible to subluxation (partial dislocation) and dislocation. Approximately half of major joint dislocations seen in emergency departments involve the shoulder.
Contents
Signs and symptoms
Diagnosis
A diagnosis of shoulder dislocation is often suspected based on patient history and physical examination. Radiographs are made to confirm the diagnosis. Most dislocations are apparent on radiographs showing incongruence of the glenohumeral joint. Posterior dislocations may be hard to detect on standard AP radiographs, but are more readily detected on other views. After reduction, radiographs are usually repeated to confirm successful reduction and to detect bony damage. After repeated shoulder dislocations, an MRI scan may be used to assess soft tissue damage. In regards to recurrent dislocations, the supine apprehension test is a useful test in determining athletes who are predisposed to future dislocations.
There are three main types of dislocations: anterior, posterior, and inferior.
Anterior (forward)
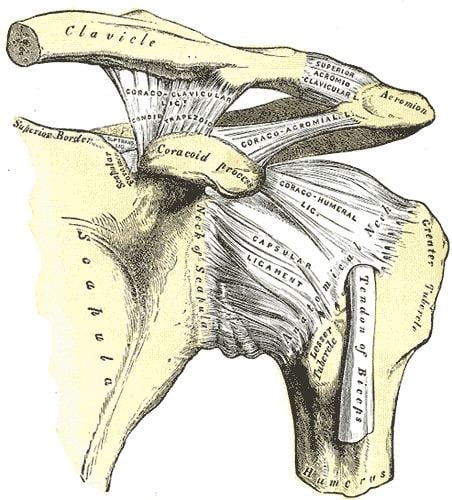
In over 95% of shoulder dislocations, the humerus is displaced anteriorly. In most of those, the head of the humerus comes to rest under the coracoid process, referred to as sub-coracoid dislocation. Sub-glenoid, subclavicular, and, very rarely, intrathoracic or retroperitoneal dislocations may also occur.
Anterior dislocations are usually caused by a direct blow to, or fall on, an outstretched arm. The patient typically holds his/her arm externally rotated and slightly abducted.
Damage to the axillary artery and axillary nerve (C5,C6) may result. The axillary nerve is injured in 37% making it the most commonly injured structure with this type of injury. Other common, associated, nerve injuries include injury to the suprascapular nerve (29%) and the radial nerve (22%). Axillary nerve damage results in a weakened or paralyzed deltoid muscle and as the deltoid atrophies unilaterally, the normal rounded contour of the shoulder is lost. A patient with injury to the axillary nerve will have difficulty in abducting the arm from approximately 15° away from the body. The supraspinatus muscle initiates abduction from a fully adducted position.
Posterior (backward)
Posterior dislocations are occasionally due to the muscle contraction from electric shock or seizure and may be caused by strength imbalance of the rotator cuff muscles. Patients typically present holding their arm internally rotated and adducted, and exhibiting flattening of the anterior shoulder with a prominent coracoid process.
Posterior dislocations may go unrecognized, especially in an elderly patient and in the unconscious trauma patient. An average interval of 1 year was noted between injury and diagnosis in a series of 40 patients.
Inferior (downward)
Inferior dislocation is the least likely, occurring in less than 1%. This condition is also called luxatio erecta because the arm appears to be permanently held upward or behind the head. It is caused by a hyper abduction of the arm that forces the humeral head against the acromion. Such injuries have a high complication rate as many vascular, neurological, tendon, and ligament injuries are likely to occur from this mechanism of injury.
Treatment
Prompt medical treatment should be sought for suspected dislocation. Usually, the shoulder is kept in its current position by use of a splint or sling (however, see below). A pillow between the arm and torso may provide support and increase comfort. Strong analgesics are needed to allay the pain of a dislocation and the distress associated with it.
Reduction
Emergency department care is focused on returning the shoulder to its normal position, a process known as reduction. Normally, closed reduction, in which the relationship of bone and joint is manipulated externally without surgical intervention, is used. A variety of techniques exist, but some are preferred due to fewer complications or easier execution. In cases where closed reduction is not successful, open, surgical, reduction may be needed. Following reduction, x-ray is often used to confirm success and absence of associated fractures. The arm should be kept in a sling or immobilizer for several days, prior to supervised recovery of motion and strength.
Traditional reduction techniques such as Hippocrates' and Kocher's are rarely used anymore. The traditional 'Hippocratic Reduction' placed the operator's heel in the person's armpit while traction was applied to their arm. Kocher's method, if performed slowly, can be performed without anesthesia. Traction is applied to the arm which is carefully adducted (brought to the mid-line). It is then externally rotated and the arm abducted (brought away from the mid-line) following which it is internally rotated and maintained in position with the help of a sling. Some avoid this technique because of the possibility of neurovascular complications and proximal humerus fracture.
A variety of non-operative reduction techniques are employed. They have certain principles in common including gentle in-line traction, reduction or abolition of muscle spasm, and gentle external rotation. They all strive to avoid inadvertent injury. Two of them, the Milch and Stimson techniques, have been compared in randomized trial. These techniques include:
Post-reduction
There does not appear to be any difference in outcomes when the arm is immobilized in internal versus external rotation following an anterior shoulder dislocation.
A 2008 study of 300 people for almost six years found that conventional shoulder immobilisation in a sling offered no benefit.
Non-operative
Rotator cuff and deltoid strengthening has long been the focus of conservative treatment for the unstable shoulder and in many cases is advocated as a substitute for surgical stabilization. In multidirectional instability patients who have experienced atraumatic subluxation or dislocation events, cohort studies demonstrate good responses to long-term progressive resistance exercises if judged according to function, pain, stability, and motion scores. However, in those experiencing a discrete traumatic dislocation event, responses to non-operative treatment are less than satisfactory, a pattern that inspired the Matsen and Harryman classification of shoulder instability, TUBS (traumatic, unidirectional, Bankart, and usually requiring surgery) and AMBRI (atraumatic, multidirectional, bilateral, rehabilitation, and occasionally requiring an inferior capsular shift). It is thought that traumatic dislocations, as opposed to atraumatic dislocations and instability events, result in a higher incidence of capsuloligamentous injuries that disturb normal anatomy and leave shoulders too structurally compromised to respond to conservative treatment. Pathoanatomic studies of those sustaining a first-time traumatic anterior dislocation and subluxation reveal a high rate of labral lesions including the important injury, in structural terms, to the glenohumeral ligament in the inferior part of the labrum, known as the Bankart lesion.
Surgery
A systematic review of published literature concerning dislocation of the shoulder has indicated that young adults engaged in highly demanding sports or job activities should be considered for operative intervention to achieve optimal outcome. Arthroscopic surgery techniques may be used to repair the glenoidal labrum, capsular ligaments, biceps long head anchor or SLAP lesion and/or to tighten the shoulder capsule.
Arthroscopic stabilization surgery has evolved from the Bankart repair, a time-honored surgical treatment for recurrent anterior instability of the shoulder. However, the failure rate following Bankart repair has been shown to increase markedly in patients with significant bone loss from the glenoid (socket). In such cases, improved results have been reported with some form of bone augmentation of the glenoid such as the Latarjet operation.
Although posterior dislocation is much less common, instability following it is no less challenging and, again, some form of bone augmentation may be required to control instability.
There remains those situations characterized by multidirectional instability, which have failed to respond satisfactorily to rehabilitation, falling under the AMBRI classification previously noted. This is usually due to an overstretched and redundant capsule which no longer offers stability or support. Traditionally, this has responded well to a 'reefing' procedure known as inferior capsular shift. More recently, the procedure has been carried out as an arthroscopic procedure, rather than open surgery, again with comparable results. Most recently, the procedure has been carried out using radio frequency technology to shrink the redundant shoulder capsule, although the long-term results of this development are currently unproven.
Prognosis
After an anterior shoulder dislocation, the risk of a future dislocation is about 20%. This risk is greater in males than females.
