 | ||
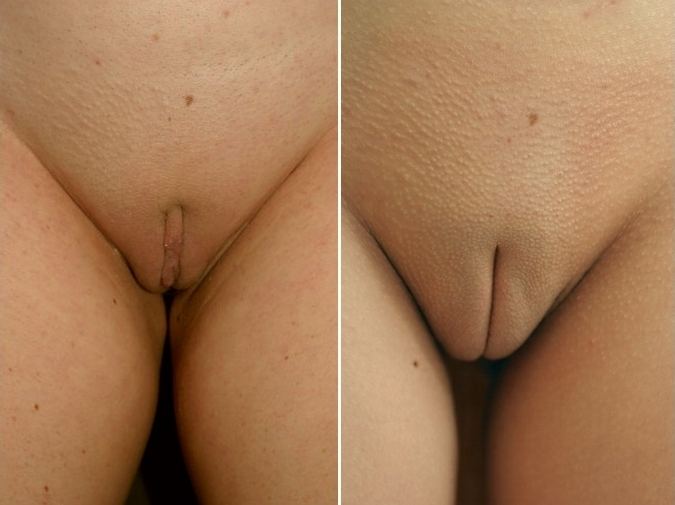
Clitoral hood reduction, also termed clitoral hoodectomy, clitoral unhooding, clitoridotomy,or (partial) hoodectomy, is a plastic surgery procedure for reducing the size and the area of the clitoral hood (prepuce) in order to further expose the clitoral glans of the clitoris.
Contents
It is sometimes done as a form of elective surgery where the therapeutic goal is to improve the sexual functioning of the woman, and the aesthetic refinement of her vulva. It is a form of hoodplasty. The reduction of the clitoral prepuce tissues usually is a sub-ordinate surgery within a labiaplasty procedure for reducing the labia minora; and occasionally within a vaginoplasty procedure.
Surgical procedures
The procedures for labiaplasty occasionally include a clitoral hood reduction. One technique for reducing the clitoral hood is the bilateral excision (cutting) of the prepuce tissues covering the clitoral glans, with especial attention to maintaining the glans in the midline. Another technique cuts away (excises) the redundant folds of clitoral prepuce tissue, with incisions parallel to the long axis of the clitoris.
Clitoral hood reduction can be included in the extended wedge resection labiaplasty technique, wherein the extension of the exterior wedge sections is applied to reducing the prepuce tissues of the clitoral glans. Yet, occasionally excess prepuce-skin, in the center of the clitoral hood, is removed with separate incisions.
Results
The functional corrections and perceived aesthetic improvements to the vulvo-vaginal complex indicate that labiaplasty procedures have a high-rate of patient satisfaction with the surgical outcome, and a low incidence-rate of medical complications. The study Aesthetic Labia Minora and Clitoral Hood Reduction using Extended Central Wedge Resection (2008) reported that of a 407-woman cohort, 98 per cent were satisfied with the labial reduction outcomes; that the average patient satisfaction score was 9.2 points on a 10-point scale; that 95 per cent of the women experienced reduced pudendal discomfort; that 93 per cent of the women experienced improved self esteem; that 71 per cent experienced improved sexual functioning; that 0.6 per cent (one woman) reported lessened sexual functioning; and that 4.4 per cent of the women experienced medical complications.
Moreover, regarding the woman’s satisfaction with the plastic surgical outcome, the study Expectations and Experience of Labial Reduction: A Qualitative Study (2007) reported that the women who underwent labiaplasty had great expectations for the elimination of pubic discomfort and pain, improved cosmetic appearance of the vulva, and improved sexual functioning. Most of the women experienced improved self esteem; yet the study also reported that formal psychological counselling before the surgical operation, about what to expect and what not to expect from a labia minora and a clitoral prepuce reduction procedure, might better serve the woman (as the patient) by assisting her in establishing realistic (feasible) goals for her genital beauty and mental health, which might be derived from a genitoplastic procedure.
Criticism
The American College of Obstetricians and Gynecologists (ACOG) published Committee Opinion No. 378: Vaginal "Rejuvenation" and Cosmetic Vaginal Procedures (2007), the college’s formal policy statement of opposition to the commercial misrepresentations of labiaplasty, and associated vaginoplastic procedures, as medically "accepted and routine surgical practices". The ACOG doubts the medical safety and the therapeutic efficacy of the surgical techniques and procedures for performing vaginoplastic operations such as labiaplasty, vaginal rejuvenation, the designer vagina, revirgination, and G-spot amplification, and recommends that women seeking such genitoplastic surgeries must be fully informed, with the available surgical-safety statistics, of the potential health risks of surgical-wound infection, of pudendal nerve damage (resulting in either an insensitive or an over-sensitive vulva), of dyspareunia (painful coitus), of tissue adhesions (epidermoid cysts), and of painful scars.
