Specialty pediatrics ICD-9-CM 770.7 MedlinePlus 001088 | ICD-10 P27.1 DiseasesDB 1713 eMedicine ped/289 | |
 | ||
Bronchopulmonary dysplasia (BPD; formerly chronic lung disease of infancy) is a chronic lung disorder of infants and children first described in 1967. It is more common in infants with low birth weight and those who receive prolonged mechanical ventilation to treat respiratory distress syndrome (RDS). It results in significant morbidity and mortality. The definition of BPD has continued to evolve since then primarily due to changes in the population, such as more survivors at earlier gestational ages, and improved neonatal management including surfactant, antenatal glucocorticoid therapy, and less aggressive mechanical ventilation.
Contents
Currently the description of BPD includes the grading of its severity into mild, moderate and severe. This correlates with the infant's maturity, growth and overall severity of illness. The new system offers a better description of underlying pulmonary disease and its severity.
Earlier criteria
The classic diagnosis of BPD may be assigned at 28 days of life if the following criteria are met:
- Positive pressure ventilation during the first 2 weeks of life for a minimum of 3 days.
- Clinical signs of abnormal respiratory function.
- Requirements for supplemental oxygen for longer than 28 days of age to maintain PaO2 above 50 mm Hg.
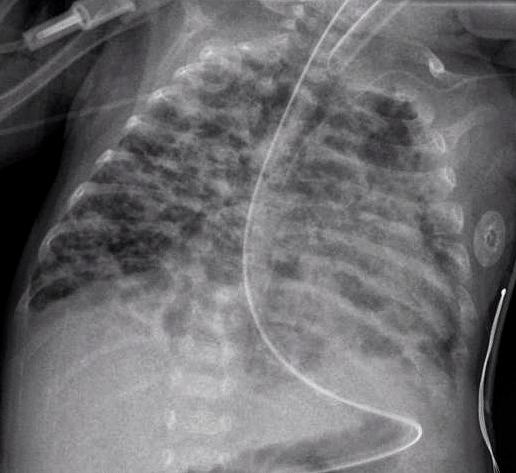
- Chest radiograph with diffuse abnormal findings characteristic of BPD.
Newer criteria
The newer National Institute of Health (US) criteria for BPD (for neonates treated with more than 21% oxygen for at least 28 days) is as follows:,
Cause and manifestations
Prolonged high oxygen delivery in premature infants causes necrotizing bronchiolitis and alveolar septal injury, with inflammation and scarring. This results in hypoxemia. Today, with the advent of surfactant therapy and high frequency ventilation and oxygen supplementation, infants with BPD experience much milder injury without necrotizing bronchiolitis or alveolar septal fibrosis. Instead, there are usually uniformly dilated acini with thin alveolar septa and little or no interstitial fibrosis. It develops most commonly in the first 4 weeks after birth.
Complications
Feeding problems are common in infants with BPD, often due to prolonged intubation. Such infants often display oral-tactile hypersensitivity (also known as oral aversion). Physical findings:
Management
There is evidence to show that steroids given to babies less than 8 days old can prevent bronchopulmonary dysplasia. However, the risks of treatment may outweigh the benefits. It is unclear if starting steroids more than 7 days after birth is harmful or beneficial. It is thus recommended that they only be used in those who cannot be taken off of a ventilator.
Epidemiology
The rate of BPD varies among institutions, which may reflect neonatal risk factors, care practices (e.g., target levels for acceptable oxygen saturation), and differences in the clinical definitions of BPD.
