Specialty gastroenterology ICD-9-CM 578.9 MedlinePlus 003133 | ICD-10 K92.2 DiseasesDB 19317 eMedicine med/3565 | |
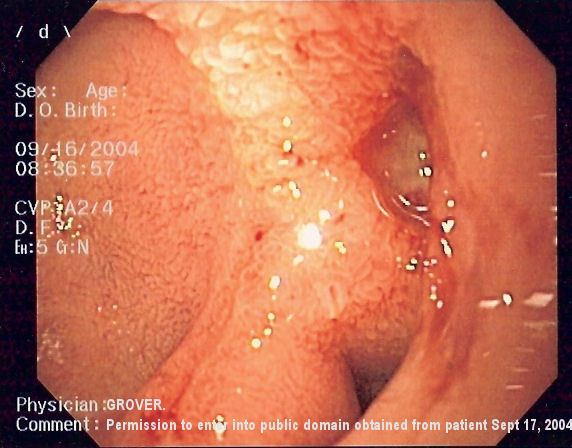 | ||
Upper gastrointestinal bleeding (sometimes upper GI, UGI bleed, Upper gastrointestinal hemorrhage, gastrorrhagia) is gastrointestinal bleeding in the upper gastrointestinal tract, commonly defined as bleeding arising from the esophagus, stomach, or duodenum. Blood may be observed in vomit (hematemesis) or in altered form in the stool (melena). Depending on the severity of the blood loss, there may be symptoms of insufficient circulating blood volume and shock. As a result, upper gastrointestinal bleeding is considered a medical emergency and typically requires hospital care for urgent diagnosis and treatment. Upper gastrointestinal bleeding can be caused by peptic ulcers, gastric erosions, esophageal varices, and some rarer causes such as gastric cancer.
Contents
- Signs and symptoms
- Causes
- Diagnosis
- Diagnostic testing
- Bayesian calculations
- Treatment
- Peptic ulcers
- Variceal bleeding
- Blood products
- Procedures
- Epidemiology
- References
The initial assessment includes measurement of the blood pressure and heart rate, as well as blood tests to determine hemoglobin concentration. In significant bleeding, fluid replacement is often required, as well as blood transfusion, before the source of bleeding can be determined by endoscopy of the upper digestive tract with an esophagogastroduodenoscopy. Depending on the source, endoscopic therapy can be applied to reduce rebleeding risk. Specific medical treatments (such as proton pump inhibitors for peptic ulcer disease) or procedures (such as TIPS for variceal hemorrhage) may be used. Recurrent or refractory bleeding may lead to need for surgery, although this has become uncommon as a result of improved endoscopic and medical treatment.
Upper gastrointestinal bleeding affects around 50-150 people per 100,000 annually. Depending on its severity, it carries an estimated mortality risk of 11%
Signs and symptoms
Persons with upper GI hemorrhage often present with hematemesis, coffee ground vomiting, melena, or hematochezia (maroon coloured stool) if the hemorrhage is severe. The presentation of bleeding depends on the amount and location of hemorrhage.
A person with an upper GI hemorrhage may also present with complications of anemia, including chest pain, syncope, fatigue and shortness of breath.
The physical examination performed by the physician concentrates on the following things:
Laboratory findings include anemia, coagulopathy, and an elevated BUN-to-creatinine ratio.
Causes
A number of medications increase the risk of bleeding including NSAIDs and SSRIs. SSRIs double the rate of upper gastrointestinal bleeding.
There are many causes for upper GI hemorrhage. Causes are usually anatomically divided into their location in the upper gastrointestinal tract.
People are usually stratified into having either variceal or non-variceal sources of upper GI hemorrhage, as the two have different treatment algorithms and prognosis.
The causes for upper GI hemorrhage include the following:
Diagnosis
The diagnosis of upper GI bleeding is assumed when hematemesis is documented. In the absence of hematemesis, an upper source for GI bleeding is likely in the presence of at least two factors among: black stool, age < 50 years, and blood urea nitrogen/creatinine ratio 30 or more. In the absence of these findings, consider a nasogastric aspirate to determine the source of bleeding. If the aspirate is positive, an upper GI bleed is greater than 50%, but not high enough to be certain. If the aspirate is negative, the source of a GI bleed is likely lower. The accuracy of the aspirate is improved by using the Gastroccult test.
Diagnostic testing
According to a study by Witting, the strongest predictors were of an upper GI bleed are black stool, age <50 years, and blood urea nitrogen/creatinine ratio 30 or more. Out of 325 persons studied, seven (5%) of 151 with none of these factors had an upper GI tract bleed, versus 63 (93%) of 68 with 2 or 3 factors.
The nasogastric aspirate can help determine the location of bleeding and thus direct initial diagnostic and treatment plans. Witting found that nasogastric aspirate has sensitivity 42%, specificity 91%, negative predictive value 64%, positive predictive value 92% and overall accuracy of 66% in differentiating upper GI bleeding from bleeding distal to the ligament of Treitz. Thus, in this study a positive aspirate is more helpful than a negative aspirate. In a smaller study, Cuellar found a sensitivity of 79% and specificity of 55%, somewhat opposite results from Witting.
Determining whether blood is in gastric contents, either vomited or aspirated specimens, is difficult. Slide tests are based on orthotolidine (Hematest reagent tablets and Bili-Labstix) or guaiac (Hemoccult and Gastroccult). Rosenthal found orthotolidine-based tests more sensitive than specific; the Hemoccult test's sensitivity reduced by the acidic environment; and the Gastroccult test be the most accurate . Cuellar found the following results:
Holman used simulated gastric specimens and found the Hemoccult test to have significant problems with non-specificity and false-positive results, whereas the Gastroccult test was very accurate. Holman found that by 120 seconds after the developer was applied, the Hemoccult test was positive on all control samples.
In a study published regarding a new scoring system called the Glasgow-Blatchford bleeding score in Lancet on January 3, 2009, 16% of patients presenting with upper GI bleed had GBS score of "0", considered low. Among these patients there were no deaths or interventions needed and the patients were able to be effectively treated in an outpatient setting.
Score is equal to "0" if the following are all present:
- Hemoglobin level >12.9 g/dL (men) or >11.9 g/dL (women)
- Systolic blood pressure >109 mm Hg
- Pulse <100/minute
- Blood urea nitrogen level <18.2 mg/dL
- No melena or syncope
- No past or present liver disease or heart failure
Bayesian calculations
The predictive values cited are based on the prevalences of upper GI bleeding in the corresponding studies. A clinical calculator can be used to generate predictive values for other prevalences.
Treatment
The initial focus is on resuscitation beginning with airway management and fluid resuscitation using either intravenous fluids and or blood. A number of medications may improve outcomes depending on the source of the bleeding. Although proton pump inhibitors are often given in the emergent setting, there is no evidence that these medications decrease death rates, re-bleeding events, or needs for surgical interventions. After the initial resuscitation has been completed, treatment is instigated to limit the likelihood of rebleeds and correct any anaemia that the bleeding may have caused.
Peptic ulcers
Based on evidence from people with other health problems crystalloid and colloids are believed to be equivalent for peptic ulcer bleeding. In people with a confirmed peptic ulcer, there is conflicting evidence if proton pump inhibitors reduce death rates, but PPIs do reduce the risk of re-bleeding and the need for surgery among this group. In those with less severe disease and where endoscopy is rapidly available, they are of less immediate clinical importance. The evidence for the inhibition of fibrinolysis with tranexamic acid is insufficient to recommend it use. But the evidence is promising. Somatostatin and octreotide while recommended for varicial bleeding have not been found to be of general use for non varicial bleeds.
Variceal bleeding
For initial fluid replacement colloids or albumin is preferred in people with cirrhosis. Medications typically includes octreotide or if not available vasopression and nitroglycerin to reduce portal pressures. This is typically in addition to endoscopic banding or sclerotherapy for the varicies. If this is sufficient then beta blockers and nitrates may be used for the prevention of re-bleeding. If bleeding continues then balloon tamponade with a Sengstaken-Blakemore tube or Minnesota tube may be used in an attempt to mechanically compress the varicies. This may then be followed by a transjugular intrahepatic portosystemic shunt.
Blood products
If large amounts of pack red blood cells are used additional platelets and fresh frozen plasma should be administered to prevent coagulopathies. Some evidence supports holding off on blood transfusions in those who have a hemoglobin greater than 7 to 8 g/dL and only moderate bleeding. If the INR is greater than 1.5 to 1.8 correction with fresh frozen plasma, prothrombin complex may decrease mortality.
Procedures
The benefits versus risks of placing a nasogastric tube in those with upper GI bleeding are not determined. Endoscopy within 24 hours is recommended. Prokinetic agents such as erythromycin before endocopy can decrease the amount of blood in the stomach and thus improve the operators view. Early endoscopy decreases hospital time and the amount of blood transfusions needed. Proton pump inhibitors, if they have not been started earlier, are recommended in those in whom high risk signs for bleeding are found. It is also recommended that people with high risk signs are kept in hospital for at least 72 hours. Blood is not recommended to correct anaemia, unless the patient is cardiovascularly unstable as this can worsen outcomes. Oral iron can be used, but this can lead to problems with compliance, tolerance, darkening stools which may mask evidence of rebleeds and tends to be slow, especially if used in conjunction with PPIs. Parenteral Iron is increasingly used in these cases to improve patient outcomes and void blood usage.
Epidemiology
About 75% of patients presenting to the emergency room with GI bleeding have an upper source . The diagnosis is easier when the patient has hematemesis. In the absence of hematemesis, 40% to 50% of patients in the emergency room with GI bleeding have an upper source
