 | ||
A subcutaneous injection is administered as a bolus into the subcutis, the layer of skin directly below the dermis and epidermis, collectively referred to as the cutis. Subcutaneous injections are highly effective in administering vaccines and medications such as insulin, morphine, diacetylmorphine and goserelin. Subcutaneous, as opposed to intravenous, injection of recreational drugs is referred to as "skin popping". Subcutaneous administration may be abbreviated as SC, SQ, sub-cu, sub-Q, SubQ, or subcut. Subcut is the preferred abbreviation for patient safety.
Contents
Subcutaneous tissue has few blood vessels and so drugs injected here are for slow, sustained rates of absorption. It is slower than Intramuscular injections but still faster than intradermal injections.
Injection sites
Sites include,
Equipment
A 25 to 31 gauge thick, 3/8" to 1" long needle can be used. The size is determined by the amount of subcutaneous tissue present, which is based on patient build. The 3/8" and 5/8" needles are most commonly used. Usually, no more than 1 mL of solution is given, compared to intradermal injections, where no more than 0.5 mL is usually given.
Procedure
Subcutaneous injections are inserted at 45 to 90 degree angles, depending on amount of subcutaneous tissue present and length of needle- a shorter, 3/8" needle is usually inserted 90 degrees and a 5/8" needle is usually inserted at 45 degrees. Medication is administered slowly, about 10 seconds/milliliter.
Subcutaneous insulin injections in diabetes mellitus
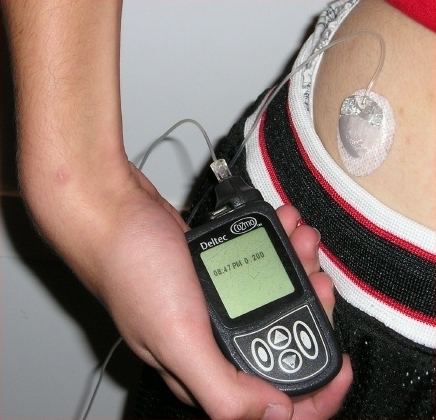
A person with insulin dependent (either Type I or Type II) diabetes mellitus typically injects insulin subcutaneously.
The injection should be given under the skin, into the fat layer.
