 | ||
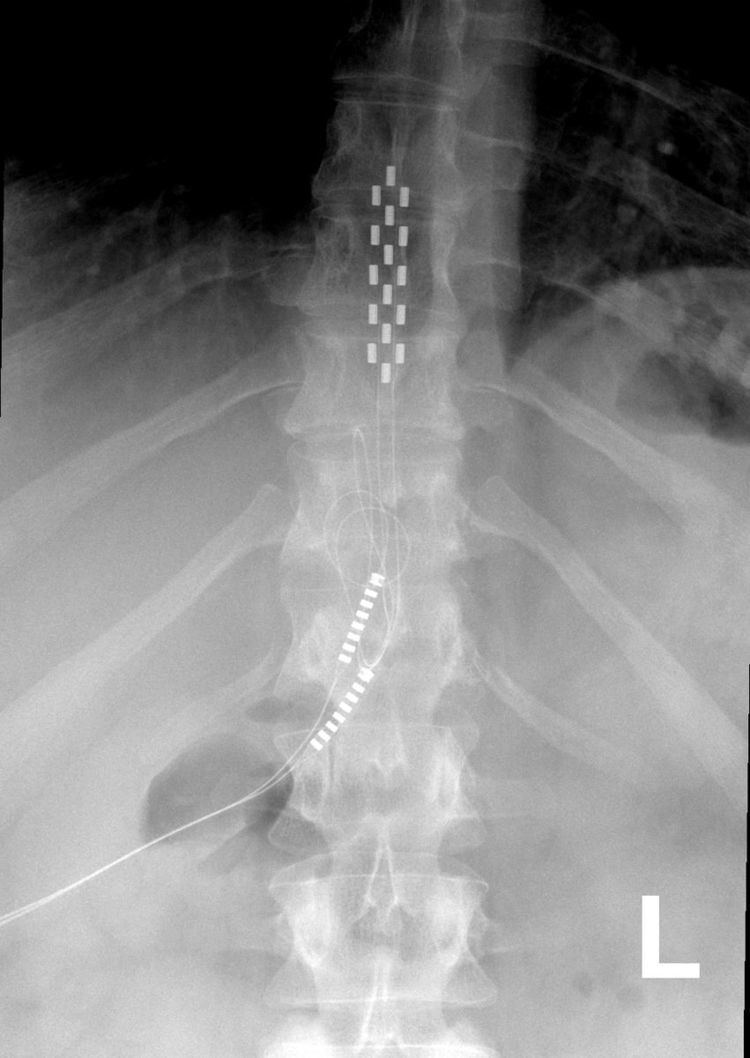
A spinal cord stimulator is a device used to apply pulsed electrical signals to the spinal cord. It is mostly used to control chronic pain, but can also be used to control spinal spasticity or to augment standing and stepping capabilities. The simplest spinal cord stimulator consists of: stimulating electrodes implanted in the epidural space; an electrical pulse generator implanted in the lower abdominal area or gluteal region; conducting wires connecting the electrodes to the generator; and the generator remote control. Spinal cord stimulation (SCS) can produce substantial analgesia (relief from pain), and is currently used mostly in the treatment of failed back surgery syndrome, complex regional pain syndrome and refractory pain due to ischemia.
Contents
Medical uses
The most common use of SCS is failed back surgery syndrome (FBSS) in the United States and peripheral ischemic pain in Europe.
FBSS, classified as mixed pain syndrome (neuropathic and nociceptive), is persistent or recurrent pain mainly involving the lower back and/or legs after successful spinal surgery. It affects about 40% of patients who undergo spinal surgeries. Several studies have shown that SCS is effective for FBSS.
SCS is also indicated in the treatment of inoperable ischemic limb pain. It can also modulate the function of the sympathetic nervous system and increase norepinephrine release in refractory angina pectoris, decreasing the probability of angina attack. SCS has also been used to treat patients with frequent migraines, using electrodes implanted in the bilateral suboccipital region. See and for a more complete list and references of further applications.
Advantages and disadvantages
SCS is analgesia on demand. It is a useful option when other forms of therapy fail. It reduces pain medication and side effects. It is effective in about 50–70% cases. It is an invasive procedure, so it can have associated complications such as infection, bleeding, and dural puncture. It has the risk of disconnection or equipment failure.
SCS interaction with diathermy, pacemakers, MRI and therapeutic ultrasound can result in unexpected changes in stimulation, serious patient injury or death. It can also lead to failure of the device.
Complications
Complications with SCS range from simple easily correctable problems to devastating paralysis, nerve injury and death. However, in a 7-year follow-up, the overall complication rate was 5-18%. The most common complications include lead migration, lead breakage, and infection. Other complications include haematomas (subcutaneous or epidural), cerebrospinal fluid (CSF) leak, post dural puncture headache, discomfort at pulse generator site, seroma and transient paraplegia. Hardware-related complications such as electrode migration, fractured electrodes, and rotation of pulse generator are also reported.
Mechanism of action
The neurophysiologic mechanisms of action of spinal cord stimulation are not completely understood. Linderoth and others have noted that the mechanism of analgesia when SCS is applied in neuropathic pain states may be very different from that involved in analgesia due to limb ischemia. In neuropathic pain states, experimental evidence show that SCS alters the local neurochemistry in dorsal horn, suppressing the hyperexcitability of the neurons. Specifically, there is some evidence for increased levels of GABA release, serotonin, and perhaps suppression of levels of some excitatory amino acids, including glutamate and aspartate. In the case of ischemic pain, analgesia seems to derive from restoration of the oxygen demand supply. This effect could be mediated by inhibition of the sympathetic system, although vasodilation is another possibility. It is also probable that a combination of the two above mentioned mechanisms is involved.
Equipment
SCS, in simplest form, consists of a pulse generator with its remote controls, implanted stimulating electrodes and conducting wires connecting the electrodes to the generator.
Generator
The generator is implanted subcutaneously, It can be a complete pulse generator module (an "implantable pulse generator" or IPG) or simply a radio frequency (RF) receiver. The IPG contains a battery; this battery may be rechargeable using an external wireless power charger, so that it does not need to be replaced surgically when it loses charge. The RF receiver is driven by an external transmitter from which it gets its power and pulses. This external transmitter has a battery which can be easily replaced. RF receivers have traditionally been used for patients who require high power settings that would quickly deplete a primary-cell IPG.
Remote Control
The patient is also provided with a remote control to turn on and off the stimulator. Depending on the device and the surgeon’s preference, it may also change the programming of the stimulation patterns. The surgeon has a programming device that could be used to modify a wide range of stimulation settings of the RF generator.
Various current, voltage and waveform configurations are possible. Some stimulators vary voltage to achieve a constant current, while others vary current to achieve a constant voltage.
Electrodes
The electrodes, which consist of an array of leads, can be percutaneous type or paddle type. Percutaneous electrodes are easier to insert than the paddle type, which require an incision over the spinal cord and a laminectomy.
Insertion procedures and techniques
SCS procedure involves careful placement of electrodes in the epidural space, followed by a trial period of 5-7 days. If the pain relief is satisfactory, the electrodes are then anchored to the interspinal ligaments, the pulse generator is positioned and implanted, and the wires are connected. The stimulator is then programmed, and postoperative care performed.
Selecting the level of stimulation
The representation of the dermatomal level in the dorsal columns of the spinal cord is much higher than the corresponding vertebral level. For instance, the sweet spot for sciatic pain (dermatomal level L5/S1) is around T10 nerve. See dermatome and Spinal cord segments.
Electrodes selection
For the SCS to be effective, the area of paresthesia must overlap the area of pain. Selection of leads depends on which arrangement will give the best paresthesia coverage to the painful area.
Generator implant
The IPG or the RF unit is usually implanted in the lower abdominal area or in the posterior superior gluteal region. It should be in a location that patients can access with their dominant hand for adjustment of their settings with the patient-held remote control. The decision to use a fully implantable IPG or an RF unit depends on several considerations. If the patient’s pain pattern requires the use of many electrodes with high power settings, an RF unit should be used. The IPG battery life will largely depend on the power settings utilized, but the newer IPG units will generally last several years at average power settings.
Programming
Programming involves selecting the electrode stimulating configuration, and adjusting the amplitude, width and frequency of electrical pulses. Amplitude (intensity of stimulation) is specified in milliamperes or volts depending on the system used. Lower amplitudes are used for peripheral nerves and paddle leads. Pulse width (the duration of each pulse) usually varies from 100 to 400 us, with wider pulses producing a broader area of paraesthesia. Pulse frequency (number of pulses per second) is usually between 20 and 120 hertz. It is an individual preference: some patients choose low frequency beating sensation whereas others prefer high frequency buzzing.
Selection of lowest possible setting on all parameters is important in conserving battery life in non-rechargeable models of SCS. Cycling of stimulation is also employed to save battery life. Changing of stimulator program may have to be undertaken during the course of therapy and follow-up.
Patient selection
Appropriate patients for neurostimulation implants must meet the following criteria: the patient has a diagnosis amenable to this therapy, the patient has failed conservative therapy, significant psychological issues have been ruled out, and a trial has demonstrated pain relief. A trial period of stimulation over a period of 5–7 days should follow the psychiatric evaluation to demonstrate its effectiveness. This part of the protocol is important because of the cost of the equipment and the invasive nature of the procedure. The trial is considered successful if the patient achieves more than a 50% reduction in pain.
History
Electrotherapy of pain by neurostimulation began shortly after Melzack and Wall proposed the gate control theory in 1965. This theory proposed that nerves carrying painful peripheral stimuli and nerves carrying touch and vibratory sensation both terminate in the dorsal horn (the gate) of spinal cord. It was hypothesized that input to the latter could be manipulated to “close the gate” to the former. As an application of the gate control theory, Shealy et al. implanted the first spinal cord stimulator device directly on the dorsal column for the treatment of chronic pain and in 1971, Shimogi and colleagues first reported the analgesic properties of epidural spinal cord stimulation. Since then this technique has undergone numerous technical and clinical developments.
At this time neurostimulation for the treatment of pain is used with nerve stimulation, spinal cord stimulation, deep brain stimulation, and motor cortex stimulation.
Cost effectiveness
The cost effectiveness of spinal cord stimulation in the treatment of chronic back pain was evaluated by Kumar and colleagues in 2002. They examined 104 patients with failed back surgery syndrome. Of the 104 patients, 60 were implanted with a spinal cord stimulator. Both groups were monitored over a period of five years. The stimulation group annual cost was $29,000 versus $38,000 in the other group. 15% returned to work in the stimulation group versus 0% in the other group. The higher costs in the nonstimulator group were in the categories of medications, emergency center visits, x-rays, and ongoing physician visits. See also for another study of cost effectiveness. See for list of such studies on cost effectiveness in various applications of SCS.
Research
SCS is finding its way to be applied to Parkinson’s disease. Recently, a case study demonstrated the first successful result of this technique in a patient with Parkinson's disease. More complex and power efficient microprocessor based equipment increasing the battery life could be developed. Closed loop bio-feedback systems which communicate and record neural responses following spinal cord stimulation could be applied and utilized In the future, it might be possible to combine SCS with implanted drug delivery systems to produce synergistic effects minimizing side effects and complications. Strong evidence is still lacking for SCS which may emerge in near future following robust research studies complimenting the rapid technological advances that is taking place in the field of SCS.
