 | ||
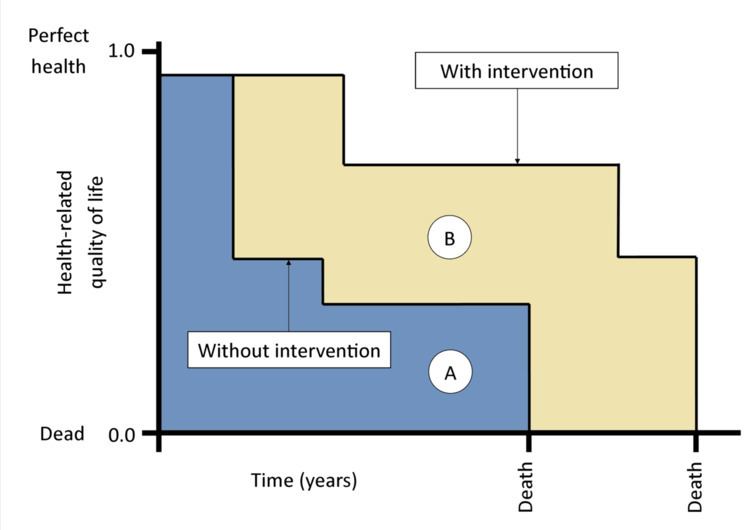
The quality-adjusted life year or quality-adjusted life-year (QALY) is a generic measure of disease burden, including both the quality and the quantity of life lived. It is used in economic evaluation to assess the value for money of medical interventions. One QALY equates to one year in perfect health. If an individual's health is below this maximum, QALYs are accrued at a rate of less than 1 per year. To be dead is associated with 0 QALYs, and in some circumstances it is possible to accrue negative QALYs to reflect health states deemed 'worse than dead'.
Contents
Use
The QALY is often used in cost-utility analysis in order to estimate the cost-per-QALY associated with a health care intervention. This incremental cost-effectiveness ratio (ICER) can then be used to allocate healthcare resources, often using a threshold approach.
In the United Kingdom, the National Institute for Health and Care Excellence, which advises on the use of health technologies within the National Health Service, has since at least 2013 used "£ per QALY" to evaluate their utility.
Meaning
The concept of the QALY is credited to work by Klarman and later Fanshel and Bush and Torrance who suggested the idea of length of life adjusted by indices of functionality or health. It was officially named the QALY in print in an article by Zeckhauser and Shepard It was later promoted through medical technology assessment conducted by the US Congress Office of Technology Assessment.
Then, in 1980, Pliskin proposed a justification of the construction of the QALY indicator using the multiattribute utility theory: if a set of conditions pertaining to agent preferences on life years and quality of life are verified, then it is possible to express the agent’s preferences about couples (number of life years/health state), by an interval (Neumannian) utility function. This utility function would be equal to the product of an interval utility function on « life years », and an interval utility function on « health state ». According to Pliskin et al., The QALY model requires utility independent, risk neutral, and constant proportional tradeoff behaviour. Because of these theoretical assumptions, the meaning and usefulness of the QALY is debated. Perfect health is hard, if not impossible, to define. Some argue that there are health states worse than being dead, and that therefore there should be negative values possible on the health spectrum (indeed, some health economists have incorporated negative values into calculations). Determining the level of health depends on measures that some argue place disproportionate importance on physical pain or disability over mental health.
Calculation
The QALY is a measure of the value of health outcomes. Since health is a function of length of life and quality of life, the QALY was developed as an attempt to combine the value of these attributes into a single index number. The basic idea underlying the QALY is simple: it assumes that a year of life lived in perfect health is worth 1 QALY (1 Year of Life × 1 Utility value = 1 QALY) and that a year of life lived in a state of less than this perfect health is worth less than 1. In order to determine the exact QALY value, it is sufficient to multiply the utility value associated with a given state of health by the years lived in that state. QALYs are therefore expressed in terms of "years lived in perfect health": half a year lived in perfect health is equivalent to 0.5 QALYs (0.5 years × 1 Utility), the same as 1 year of life lived in a situation with utility 0.5 (e.g. bedridden) (1 year × 0.5 Utility). QALYs can then be incorporated with medical costs to arrive at a final common denominator of cost/QALY. This parameter can be used to develop a cost-effectiveness analysis of any treatment. Data is collected through use of surveys such as EQ-5D.
Weighting
The "weight" values between 0 and 1 are usually determined by methods such as those proposed in the Journal of Health Economics:
Another way of determining the weight associated with a particular health state is to use standard descriptive systems such as the EuroQol Group's EQ-5D questionnaire, which categorises health states according to five dimensions: mobility, self-care, usual activities (e.g. work, study, homework or leisure activities), pain/discomfort and anxiety/depression.
Debate
The method of ranking interventions on grounds of their cost per QALY gained ratio (or ICER) is controversial because it implies a quasi-utilitarian calculus to determine who will or will not receive treatment. However, its supporters argue that since health care resources are inevitably limited, this method enables them to be allocated in the way that is approximately optimal for society, including most patients. Another concern is that it does not take into account equity issues such as the overall distribution of health states – particularly since younger, healthier cohorts have many times more QALYs than older or sicker individuals. As a result, QALY analysis may undervalue treatments which benefit the elderly or others with a lower life expectancy. Also, many would argue that all else being equal, patients with more severe illness should be prioritised over patients with less severe illness if both would get the same absolute increase in utility. In 2013 the results of a European Commission Project, ECHOUTCOME recommended to not use QALYs in health decision making after surveying 1361 subjects in the UK, Belgium, France and Italy and establishing that the four theoretical assumptions underlying QALYs are invalid (quality of life should be measured in consistent intervals; life years and QOL should be independent; people should be neutral about risk; and willingness to sacrifice life years should be constant over time), explaining why divergent QALY results can be generated using the same dataset. In response, Dr Andrew Walker from the University of Glasgow said that these problems with QALYs were already widely acknowledged but that the study's suggested alternatives were not well specified and did not take budgetary constraints into consideration.
Future development
The UK Medical Research Council is exploring including other wellbeing factors (not just health) in future measures.
