Kingdom Bacteria Order Actinomycetales Genus Propionibacterium Higher classification Propionibacterium | Phylum Actinobacteria Family Propionibacteriaceae Scientific name Propionibacterium acnes Rank Species | |
 | ||
Similar Propionibacterium, Bacteria, Fusobacterium, Haemophilus, Moraxella | ||
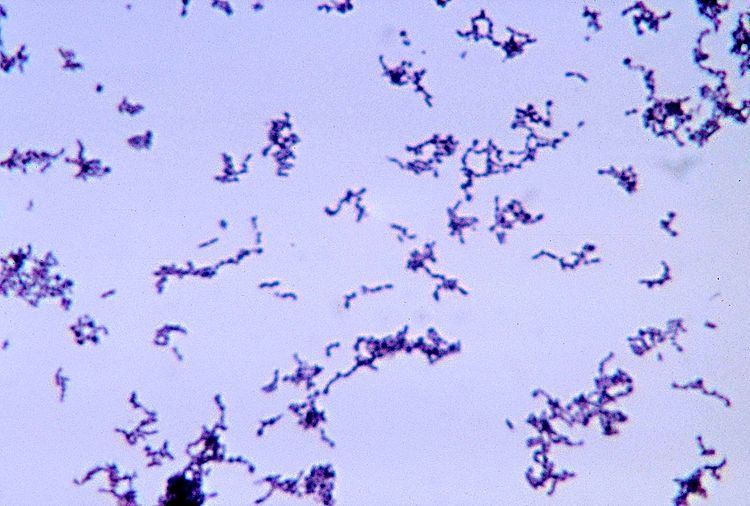
Propionibacterium acnes
Propionibacterium acnes is the relatively slow-growing, typically aerotolerant anaerobic, Gram-positive bacterium (rod) linked to the skin condition of acne; it can also cause chronic blepharitis and endophthalmitis, the latter particularly following intraocular surgery. The genome of the bacterium has been sequenced and a study has shown several genes can generate enzymes for degrading skin and proteins that may be immunogenic (activating the immune system).
Contents
- Propionibacterium acnes
- Handwritten tutiorial acn por propionibacterium acnes
- Role in disease
- Antimicrobial susceptibility
- Photosensitivity
- Other habitats
- References
This bacterium is largely commensal and part of the skin flora present on most healthy adult humans' skin. It is usually just barely detectable on the skin of healthy preadolescents. It lives primarily on, among other things, fatty acids in sebum secreted by sebaceous glands in the follicles. It may also be found throughout the gastrointestinal tract in humans and many other animals.
It is named after its ability to generate propionic acid.
Handwritten tutiorial acn por propionibacterium acnes
Role in disease
P. acnes bacteria live deep within follicles and pores, away from the surface of the skin. In these follicles, P. acnes bacteria use sebum, cellular debris and metabolic byproducts from the surrounding skin tissue as their primary sources of energy and nutrients. Elevated production of sebum by hyperactive sebaceous glands (sebaceous hyperplasia) or blockage of the follicle can cause P. acnes bacteria to grow and multiply.
P. acnes bacteria secrete many proteins, including several digestive enzymes. These enzymes are involved in the digestion of sebum and the acquisition of other nutrients. They can also destabilize the layers of cells that form the walls of the follicle. The cellular damage, metabolic byproducts and bacterial debris produced by the rapid growth of P. acnes in follicles can trigger inflammation. This inflammation can lead to the symptoms associated with some common skin disorders, such as folliculitis and acne vulgaris.
The damage caused by P. acnes and the associated inflammation make the affected tissue more susceptible to colonization by opportunistic bacteria, such as Staphylococcus aureus. Preliminary research shows healthy pores are only colonized by P. acnes, while unhealthy ones universally include the nonpore-resident Staphylococcus epidermidis, amongst other bacterial contaminants. Whether this is a root causality, just opportunistic and a side effect, or a more complex pathological duality between P. acnes and this particular Staphylococcus species is not known.
P. acnes has also been found in corneal ulcers, and is a common cause of chronic endophthalmitis following cataract surgery. Rarely, it infects heart valves leading to endocarditis, and infections of joints (septic arthritis) have been reported. Furthermore, Propionibacterium species have been found in ventriculostomy insertion sites, and areas subcutaneous to suture sites in patients who have undergone craniotomy. It is a common contaminant in blood and cerebrospinal fluid cultures.
P. acnes has been found in herniated discs. The propionic acid which it secretes creates micro-fractures of the surrounding bone. These micro-fractures are sensitive and it has been found that antibiotics have been helpful in resolving this type of low back pain.
P. acnes can be found in bronchoalveolar lavage of approximately 70% of patients with sarcoidosis and is associated with disease activity, but it can be also found in 23% of controls. The subspecies of P. acnes that cause these infections of otherwise sterile tissues (prior to medical procedures), however, are the same subspecies found on the skin of individuals who do not have acne-prone skin, so are likely local contaminants. Moderate to severe acne vulgaris appears to be more often associated with virulent strains.
P. acnes is an opportunistic pathogen, causing a range of postoperative and device-related infections e.g., surgery, post-neurosurgical infection, joint prostheses, shunts and prosthetic heart valves. P. acnes may play a role in other conditions, including inflammation of the prostate leading to cancer, SAPHO (Synovitis, Acne, Pustulosis, Hyperostosis, Osteitis) syndrome, sarcoidosis and sciatica.
Antimicrobial susceptibility
P. acnes bacteria are susceptible to a wide range of antimicrobial molecules, from both pharmaceutical and natural sources. Antibiotics are commonly used to treat infections caused by P. acnes. Acne vulgaris is the disease most commonly associated with P. acnes infection. The antibiotics most frequently used to treat acne vulgaris are: erythromycin, clindamycin, doxycycline and minocycline. Several other families of antibiotics are also active against P. acnes bacteria, including quinolones, cephalosporins, pleuromutilins, penicillins and sulfonamides.
The emergence of antibiotic-resistant P. acnes bacteria represents a growing problem worldwide. The problem is especially pronounced in North America and Europe. The antibiotic families that P. acnes are most likely to acquire resistance to are the macrolides (e.g., erythromycin and azithromycin), lincosamides (e.g., clindamycin) and tetracyclines (e.g., doxycycline and minocycline).
However, P. acnes bacteria are susceptible to many types of antimicrobial chemicals found in over-the-counter antibacterial products, including benzoyl peroxide, triclosan, chloroxylenol (PCMX), and chlorhexidine gluconate.
Several naturally occurring molecules and compounds are toxic to P. acnes bacteria. Some essential oils such as rosemary, tea tree oil, clove oil and citrus oils contain antibacterial chemicals.
The elements silver, sulfur, and copper have also been demonstrated to be toxic towards many bacteria, including P. acnes. Natural honey has also been shown to have some antibacterial properties that may be active against P. acnes.
Photosensitivity
P. acnes glows orange when exposed to blacklight, possibly due to the presence of endogenous porphyrins. The bacterium is killed by ultraviolet light. P. acnes is also especially sensitive to light in the 405–420 nanometer (near the ultraviolet) range due to an endogenic porphyrin–coporphyrin III. A total irradiance of 320 J/cm² is found to inactivate this bacterium in vitro. This fact is used in phototherapy. Its photosensitivity can be enhanced by pretreatment with aminolevulinic acid, which boosts production of this chemical, although this causes significant side effects in humans, and in practice was not significantly better than the light treatment alone.
Other habitats
Unexpectedly, P. acnes was found to be an endophyte of plants. Notably, grapevine appears to host an endophytic population of P. acnes that is closely related to the human-associated strains and whose line diverged roughly 7,000 years ago, at about the same time when grapevine agriculture may have been established. This P. acnes subtype was dubbed Zappae in honour of the musician Frank Zappa.
