 | ||
Mastitis in dairy cattle is the persistent, inflammatory reaction of the udder tissue. Mastitis, a potentially fatal mammary gland infection, is the most common disease in dairy cattle in the United States. It is also the most costly to the dairy industry. Milk from cows suffering from mastitis has an increased somatic cell count.
Contents
Definition
Mastitis occurs when white blood cells (leukocytes) are released into the mammary gland, usually in response to bacteria invading the teat canal. Milk-secreting tissue and various ducts throughout the mammary gland are damaged due to toxins released by the bacteria. Mastitis can also occur as a result of chemical, mechanical, or thermal injury.
Identification
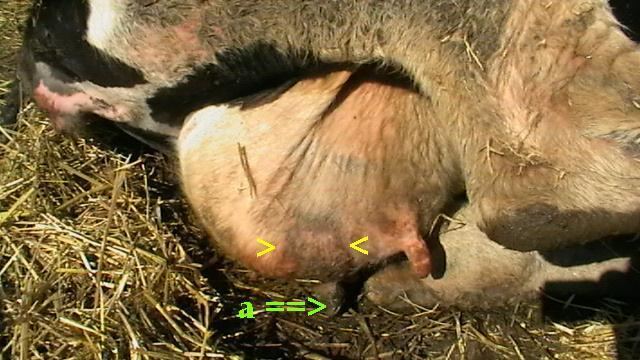
This disease can be identified by abnormalities in the udder such as swelling, heat, redness, hardness, or pain (if it is clinical). Other indications of mastitis may be abnormalities in milk such as a watery appearance, flakes, or clots. When infected with subclinical mastitis, a cow does not show any visible signs of infection or abnormalities.
Mastitis-causing bacteria
Bacteria that are known to cause mastitis include:
Types of mastitis
Mastitis may be classified according two different criteria: either according to the clinical symptoms or depending on the mode of transmission.
Transmission
Mastitis is most often transmitted by repetitive contact with the milking machine, and through contaminated hands or materials.
Effects on milk composition
Mastitis can cause a decline in potassium and lactoferrin. It also results in decreased casein, the major protein in milk. As most calcium in milk is associated with casein, the disruption of casein synthesis contributes to lowered calcium in milk. The milk protein continues to undergo further deterioration during processing and storage. Milk from cows with mastitis also has a higher somatic cell count. Generally speaking, the higher the somatic cell count, the lower the milk quality.
Detection
Cattle affected by mastitis can be detected by examining the udder for inflammation and swelling, or by observing the consistency of the milk, which will often develop clots or change color when a cow is infected.
Another method of detection is the California mastitis test, which is designed to measure the milk's somatic cell count as a means for detecting inflammation and infection of the udder.
Treatment
Treatment is possible with long-acting antibiotics, but milk from such cows is not marketable until drug residues have left the cow's system. Antibiotics may be systemic (injected into the body), or they may be forced upwards into the teat through the teat canal (intramammary infusion). Cows being treated may be marked with tape to alert dairy workers, and their milk is syphoned off and discarded. To test whether whether the antibiotics residues are within regulatory requirements, special tests exists. Vaccinations for mastitis do exist, but as they only reduce the severity of the condition, and do not prevent new infection they should be used in conjunction with a mastitis prevention program.
Control
Practices such as good nutrition, proper milking hygiene, and the culling of chronically infected cows can help. Ensuring that cows have clean, dry bedding decreases the risk of infection and transmission. Dairy workers should wear rubber gloves while milking, and machines should be cleaned regularly to decrease the incidence of transmission.
Prevention
A good milking routine is vital. This usually consists of applying a pre-milking teat dip or spray, such as an iodine spray, and wiping teats dry prior to milking. The milking machine is then applied. After milking, the teats can be cleaned again to remove any growth medium for bacteria. A post milking product such as iodine-propylene glycol dip is used as a disinfectant and a barrier between the open teat and the bacteria in the air. Mastitis can occur after milking because the teat holes close after 15 minutes if the animal sits in a dirty place with feces and urine.
Industry costs
This disease costs the US dairy industry about 1.7 to 2 billion USD each year.
