 | ||
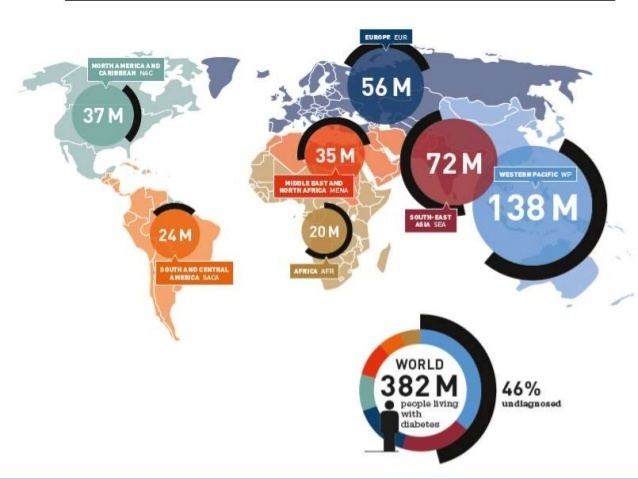
Globally, an estimated 422 million adults are living with diabetes mellitus, according to the latest 2016 data from the World Health Organization (WHO). Diabetes prevalence is increasing rapidly; previous 2013 estimates from the International Diabetes Federation put the number at 381 million people having diabetes. The number is projected to almost double by 2030. Type 2 diabetes makes up about 85-90% of all cases. Increases in the overall diabetes prevalence rates largely reflect an increase in risk factors for type 2, notably greater longevity and being overweight or obese.
Contents
Diabetes mellitus occurs throughout the world, but is more common (especially type 2) in the more developed countries. The greatest increase in prevalence is, however, occurring in low- and middle-income countries including in Asia and Africa, where most patients will probably be found by 2030. The increase in incidence in developing countries follows the trend of urbanization and lifestyle changes, including increasingly sedentary lifestyles, less physically demanding work and the global nutrition transition, marked by increased intake of foods that are high energy-dense but nutrient-poor (often high in sugar and saturated fats, sometimes referred to as the Western pattern diet). The risk of getting type 2 diabetes has been widely found to be associated with lower socio-economic position across countries.
The WHO estimates that diabetes resulted in 1.5 million deaths in 2012, making it the 8th leading cause of death. However another 2.2 million deaths worldwide were attributable to high blood glucose and the increased risks of associated complications (e.g. heart disease, stroke, kidney failure), which often result in premature death and are often listed as the underlying cause on death certificates rather than diabetes.
China
Almost one Chinese adult in ten has diabetes. A 2010 study estimated that more than 92 million Chinese adults have the disease, with another 150 million showing early symptoms. The incidence of the disease is increasing rapidly: a reported 30% increase in 7 years. Indigenous nomadic peoples like Tibetans and Mongols are at much higher susceptibility than Han Chinese.
India
Until recently, India had more diabetics than any other country in the world, according to the International Diabetes Foundation, although the country has now been surpassed in the top spot by China. Diabetes currently affects more than 62 million Indians, which is more than 7.1% of the adult population. The average age on onset is 42.5 years. Nearly 1 million Indians die due to diabetes every year.
According to the Indian Heart Association, India is projected to be home to 109 million individuals with diabetes by 2035. A study by the American Diabetes Association reports that India will see the greatest increase in people diagnosed with diabetes by 2030. The high incidence is attributed to a combination of genetic susceptibility plus adoption of a high-calorie, low-activity lifestyle by India's growing middle class.
United Kingdom
About 3.8 million people in the United Kingdom have diabetes mellitus, but the charity Diabetes U.K. have made predictions that could become high as 6.2 million by 2035/2036. The NHS spent a daily average of £2.2m (€2.6m; $3.7m) in 2013 on prescriptions for managing diabetes in primary care, and about 10% of the primary care prescribing budget is spent on treating diabetes. Diabetes U.K. have also predicted that the National Health Service could be spending as much as 16.9 billion pounds on diabetes mellitus by 2035, a figure that means the NHS could be spending as much as 17% of its budget on diabetes treatment by 2035.
Canada
Almost 2.4 million Canadians (6.8%) have been diagnosed with type 1 or type 2 diabetes, based on 2009 chronic disease surveillance data. Prevalence is higher among males (7.2%) than females (6.4%). However these numbers are likely an underestimate, as data obtained from blood samples indicate about 20% of diabetes cases remain undiagnosed.
Accounting for the younger age structure in Aboriginal populations, the prevalence of diabetes is 2-3 times higher among First Nations and Métis, compared to the non-Aboriginal population.
The prevalence of diagnosed diabetes among Canadians increased by 70% over the decade from 1999 to 2009. The greatest relative increase in prevalence was seen younger adults (35 to 44 years), attributable in part to increasing rates of overweight and obesity. The Public Health Agency of Canada estimates that if current trends in diabetes continue, the number of Canadians living with diabetes will reach 3.7 million by 2019.
United States
Diabetes rates in the United States, like across North America and around the world, have been increasing substantially. According to the 2014 Statistics Report done by the CDC it was found that, “Diabetes Mellitus affects an estimated 29.1 million people in the United States and is the 7th leading cause of death. It also increases the chances of mortality, as well as the risk for heart attack, kidney failure, and blindness” While the number of people with diabetes in the US continues to grow, the number of new cases has been declining since 2009, after decades of increases in new cases. In 2014, more than 29 million people had diabetes in the United States, of whom 7 million people remain undiagnosed. As of 2012 another 57 million people were estimated to have prediabetes. There were approximately 12.1 million diabetes-related emergency department (ED) visits in 2010 for adults aged 18 years or older (515 per 10,000 U.S. population), accounting for 9.4 percent of all ED visits.
The Centers for Disease Control and Prevention (CDC) has called the change an epidemic. Geographically, there is a U.S. diabetes belt with high diabetes prevalence estimates, which includes Mississippi and parts of Alabama, Arkansas, Florida, Georgia, Kentucky, Louisiana, North Carolina, Ohio, Pennsylvania, South Carolina, Tennessee, Texas, Virginia, and West Virginia. The National Diabetes Information Clearinghouse estimates diabetes costs $132 billion in the United States alone every year. About 5%–10% of diabetes cases in North America are type 1, with the rest being type 2. The fraction of type 1 in other parts of the world differs. Most of this difference is not currently understood. The American Diabetes Association (ADA) cites the 2003 assessment of the National Center for Chronic Disease Prevention and Health Promotion (Centers for Disease Control and Prevention) that one in three Americans born after 2000 will develop diabetes in their lifetimes. Diabetes is also more prominent in minority groups. For example according to the American Diabetes Association the rates of diagnosed diabetes are 12.8% of Hispanics, 13.2% of Non-Hispanic blacks, 15.9% of American Indians/Alaskan Natives. While Non-Hispanic whites are 7.6% and only 9% of Asian Americans have diagnosed diabetes. 4.9% of American adults had diabetes in 1990. By 1998, that number rose by a third to 6.5%. The prevalence of diabetes increased for both sexes and every racial group. American women have suffered from diabetes at a higher rate than men, with 7.4% of women being diabetic in 1998, as opposed to only 5.5% of men. The increase in diabetes coincides with an increase in average weight across both genders. In the same time frame, average weight in both men and women increased by nearly 4 kilograms. This relates to the fact that the most common form of diabetes, type 2, is strongly associated with unhealthy weight. Older Americans have suffered from diabetes at a much higher rate than younger people, with over 12% of those in their 60s and 70s being diabetic in 1998. In the same year, less than 2% of those under 30 suffered from diabetes. Weight is also a strong factor in one's likelihood of becoming diabetic, with 13.5% of obese Americans in 1998 being diabetic. In the same year, only 3.5% of people at a healthy weight had the disease.
As of 2006, about 18.3% (8.6 million) of Americans age 60 and older had diabetes, according to the ADA. Diabetes mellitus prevalence increases with age, and the numbers of older persons with diabetes are expected to grow as the elderly population increases in number. The National Health and Nutrition Examination Survey (NHANES III) from 1988–1994 demonstrated, in the population over 65 years old, 18% to 20% had diabetes, with 40% having either diabetes or its precursor form of impaired glucose tolerance. Older individuals are also more likely to be seen in the emergency department (ED) for diabetes. A study by the Agency for Healthcare Research and Quality (AHRQ) found that in 2010, diabetes-related ED visit rates were highest for patients aged 65 and older (1,307 per 10,000 population), compared with 45- to 64-year-olds (584 per 10,000 population) and 18- to 44-year-olds (183 per 10,000 population).
A second study by AHRQ found that diabetes with complications was one of the twenty most expensive conditions seen in U.S. inpatient hospitalizations in 2011, with an aggregate cost of nearly $5.4 billion for 561,000 stays. It was among the top five most expensive conditions for uninsured patients, at an aggregate cost of $440 million for 62,000 hospitalizations.
Australia
An estimated 700,000 Australians have diabetes. Indigenous populations in developed countries generally have higher prevalence and incidence of diabetes than their corresponding nonindigenous populations. In Australia, the age-standardised prevalence of self-reported diabetes in indigenous Australians is almost four times that of nonindigenous Australians. Reasons include higher rates of obesity, physical inactivity, and living in poor housing and environments among Indigenous peoples. Preventative community health programs are showing some success in tackling this problem.
