Kingdom Fungi Higher classification Cryptococcus | Phylum Basidiomycota Family Tremellaceae Scientific name Cryptococcus gattii Rank Species | |
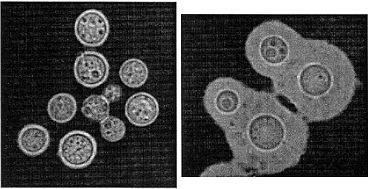 | ||
Similar Cryptococcus, Coccidioides, Candida parapsilosis, Coccidioides immitis, Paracoccidioides brasiliensis | ||
Cryptococcus gattii deadly fungus spreads killing united states canada
Cryptococcus gattii, formerly known as Cryptococcus neoformans var gattii, is an encapsulated yeast found primarily in tropical and subtropical climates. Its teleomorph is Filobasidiella bacillispora, a filamentous fungus belonging to the class Tremellomycetes.
Contents
- Cryptococcus gattii deadly fungus spreads killing united states canada
- Nomenclature
- Disease summary
- Environmental occurrence
- Epidemiology
- Transmission
- Symptoms
- Diagnosis
- Treatment
- References
Cryptococcus gattii causes the human diseases of pulmonary cryptococcosis (lung infection), basal meningitis, and cerebral cryptococcomas. Occasionally, the fungus is associated with skin, soft tissue, lymph node, bone, and joint infections. In recent years, it has appeared in British Columbia, Canada and the Pacific Northwest. It has been suggested that global warming may have been a factor in its emergence in British Columbia. From 1999 through to early 2008, two hundred and sixteen people in British Columbia have been infected with C. gattii, and eight died from complications related to it. The fungus also infects animals, such as dogs, koalas and dolphins. In 2007, the fungus appeared for the first time in the United States, in Whatcom County, Washington and in April 2010 had spread to Oregon. The most recently identified strain, designated VGIIc, is particularly virulent, having proved fatal in 19 out of 218 known cases.
Nomenclature
Cryptococcus gattii has recently been divided into five species. These are C. gattii, C. bacillisporus, C. deuterogattii, C. tetragattii and C. decagattii.
Disease summary
Cryptococcal disease is a very rare disease that can affect the lungs (pneumonia) and nervous system (causing meningitis and focal brain lesions called cryptococcomas) in humans. The main complication of lung infection is respiratory failure. Central nervous system infection may lead to hydrocephalus, seizures and focal neurological deficit.
Environmental occurrence
Soil debris associated with certain tree species has been found frequently to contain C. gattii VGIII MATα and MATa, and less commonly VGI MATα, in Southern California. These isolates were fertile, were found to be indistinguishable from the human isolates by genome sequence, and were virulent in in vitro and animal tests. Isolates were found associated with Canary Island pine (Pinus canariensis), American sweetgum (Liquidambar styraciflua) and Pohutukawa tree (Metrosideros excelsa). Leading up to the study one of the authors, Scott Filler, sent his daughter Elan to obtain and culture fungal samples in the greater Los Angeles area; one of these turned out to be C. gattii. Her work was presented at the Los Angeles County Science Fair, and she was credited as an author on the publication.
Lead author Deborah Springer said, "Just as people who travel to South America are told to be careful about drinking the water, people who visit other areas like California, the Pacific Northwest and Oregon need to be aware that they are at risk for developing a fungal infection, especially if their immune system is compromised."
Epidemiology
The highest incidences of C. gattii infections occur in Papua New Guinea and Northern Australia. Cases have also been reported in other regions, indicating its spread to India, Brazil, Vancouver Island in Canada, Washington State, and Oregon in the United States.
Unlike Cryptococcus neoformans, C. gattii is not particularly associated with human immunodeficiency virus infection or other forms of immunosuppression. The fungus can cause disease in healthy people, potentially due to its ability to grow extremely rapidly within white blood cells.
In the United States, C. gattii serotype B, subtype VGIIa, is largely responsible for clinical cases. The VGIIa subtype was responsible for the outbreaks in Canada; it then appeared in the U.S. Pacific Northwest.
According to a CDC summary, from 2004 to 2010, 60 cases were identified in the U.S.: 43 in Oregon, 15 from Washington, and one each from Idaho and California. Slightly more than half of these case were immunocompromised. 92% of all isolates were of the VGIIa subtype. In 2007, the first case in North Carolina was reported, subtype VGI, which is identical to the isolates found in Australia and California. In 2009, one case was identified in Arkansas.
Transmission
The infection is caused by inhaling yeasts or spores. The fungus is not transmitted from person to person or from animal to person. A person with cryptococcal disease is not contagious.
Symptoms
Most people who are exposed to the fungus do not become ill. In people who become ill, symptoms appear many weeks to months after exposure. Symptoms of cryptococcal disease include:
Diagnosis
Culture of sputum, bronchoalveolar lavage, lung biopsy, cerebrospinal fluid or brain biopsy specimens on selective agar allows differentiation between the five members of the C. gattii species complex and the two members of the C. neoformans species complex.
Molecular techniques may be used to speciate Cryptococcus from specimens that fail to culture.
Cryptococcal antigen testing from serum or CSF is a useful preliminary test for Cryptococcal infection, and has high sensitivity for disease. It does not distinguish between different species of Cryptococcus.
Treatment
Medical treatment consists of prolonged intravenous therapy (for 6–8 weeks or longer) with the anti-fungal drug Amphotericin B, either in its conventional or lipid formulation. The addition of oral or intravenous flucytosine improves response rates. Oral fluconazole is then administered for six months or more.
Antifungals alone are often insufficient to cure C. gattii infections, and surgery to resect infected lung (lobectomy) or brain is often required. Ventricular shunts and Ommaya reservoirs are sometimes employed in the treatment of central nervous system infection.
