ICD-9-CM 67.5 eMedicine 1848163 | MeSH D023802 | |
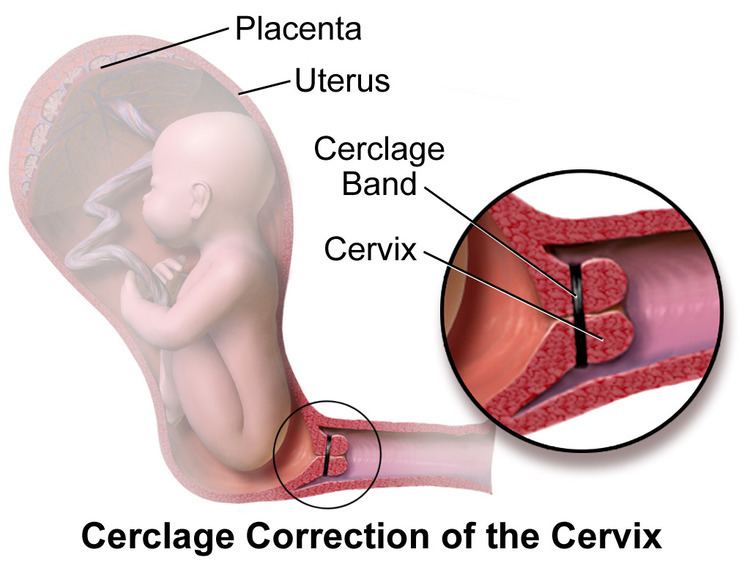 | ||
Cervical cerclage, also known as a cervical stitch, is a treatment for cervical incompetence or insufficiency, when the cervix starts to shorten and open too early during a pregnancy causing either a late miscarriage or preterm birth. Usually the treatment is done in the second trimester of pregnancy, for a woman who had either one or more late miscarriages in the past.
Contents
The treatment consists of a strong suture being inserted into and around the cervix early in the pregnancy, usually between weeks 12 to 14, and then removed towards the end of the pregnancy when the greatest risk of miscarriage has passed.
In women with a prior spontaneous preterm birth and who are pregnant with one baby, and have shortening of the cervical length less than 25 mm, a cerclage prevents a preterm birth and reduces death and illness in the baby. There is no evidence that cerclage is effective in a multiple gestation pregnancy for preventing preterm births and reducing perinatal deaths or neonatal morbidity.
Types
There are three types of cerclage:
Aftercare
After the cerclage has been placed, the patient will be observed for at least several hours (sometimes overnight) to ensure that she does not go into premature labor. The patient will then be allowed to return home, but will be instructed to remain in bed or avoid physical activity (to include coitus) for two to three days, or up to two weeks. Follow-up appointments will usually take place so that her doctor can monitor the cervix and stitch and watch for signs of premature labor.
Risks
While cerclage is generally a safe procedure, there are a number of potential complications that may arise during or after surgery. These include:
Results
The success rate for cervical cerclage is approximately 80-90% for elective cerclages, and 40-60% for emergency cerclages. A cerclage is considered successful if labor and delivery is delayed to at least 37 weeks (full term).
For women who are pregnant with one baby (a singleton pregnancy) and at risk for a preterm birth, when cerclage is compared with no treatment, despite there being a reduction in preterm birth, there is no reduction in deaths of the baby before or after birth, or reduction in illness in the baby after birth. There is no evidence that cerclage is effective in a multiple gestation pregnancy for preventing preterm births and reducing perinatal deaths or neonatal morbidity.
