Scientific name Campylobacter Rank Genus Order Campylobacterales | Family Campylobacteraceae Higher classification Campylobacteraceae Phylum Proteobacteria | |
 | ||
Lower classifications Campylobacter coli, Campylobacter fetus, Campylobacter jejuni, Campylobacter rectus, Campylobacter concisus | ||
Campylobacter introduction
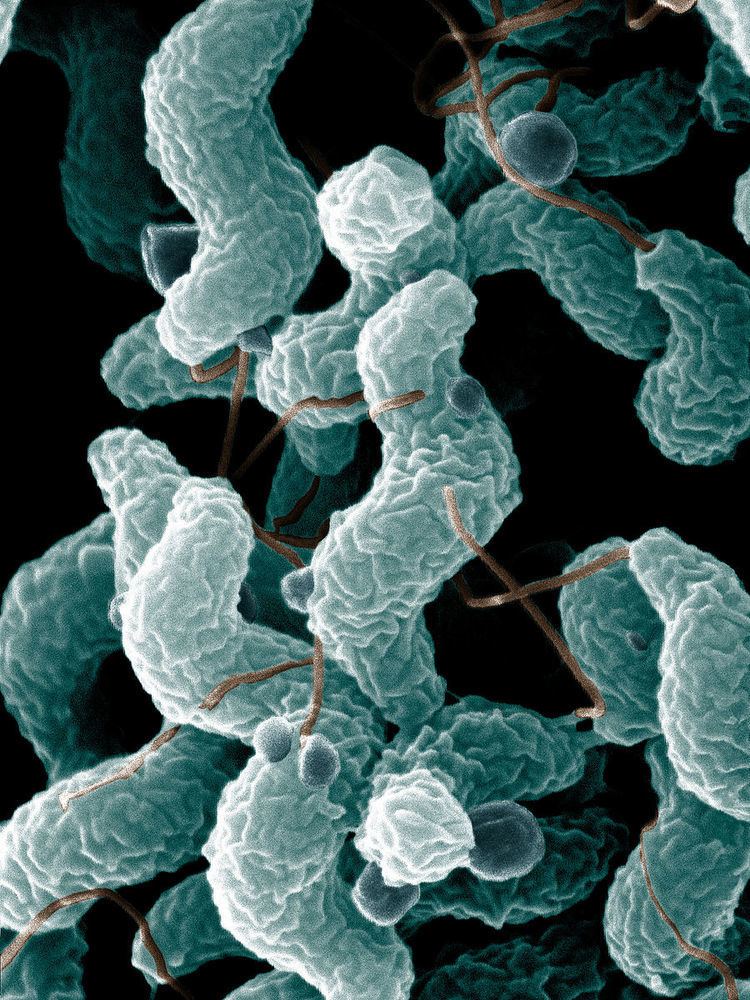
Campylobacter (meaning "curved bacteria") is a genus of Gram-negative bacteria. Campylobacter typically appear comma or s-shaped and motile.
Contents
- Campylobacter introduction
- Campylobacter
- Description
- History
- Genetics
- Bacteriophage
- Pathogenesis
- Treatment
- UK
- USA
- Canada
- New Zealand
- References
Most Campylobacter species can cause disease and can infect humans and other animals. The bacterium's main reservoir is poultry; humans can contract the disease from eating food contaminated with Campylobacter species. Another source of infection is contact with infected animals, which often carry Campylobacter asymptomatically. At least a dozen species of Campylobacter have been implicated in human disease, with C. jejuni and C. coli being the most common. C. jejuni is now recognized as one of the main causes of bacterial foodborne disease in many developed countries. C. jejuni infection can also spread to the blood in individuals with AIDS, while C. lari is a known cause of recurrent diarrhea in children. C. fetus is a cause of spontaneous abortions in cattle and sheep, as well as an opportunistic pathogen in humans.
Campylobacter
Description
Campylobacter generally appear curved or comma-shaped, and are able to move via unipolar or bipolar flagella. They generally survive in environments with low oxygen. When exposed to atmospheric oxygen, C. jejuni is able to change into a coccal form They are positive by the oxidase test and catalase test. Campylobacter are nonfermentative. Campylobacters are best cultured at 42°C .
History
The symptoms of Campylobacter infections were described in 1886 in infants by Theodor Escherich. These infections were named cholera infantum, or summer complaint. The genus was first described in 1963; however, the organism was not isolated until 1972 in Brussels, Belgium .
Genetics
The genomes of several Campylobacter species have been sequenced, beginning with C. jejuni in 2000. These genome studies have identified molecular markers specific to members of Campylobacter. Additionally, several markers were found in all Campylobacter species except for C. fetus, the most distantly-related species. Many markers were also found which were conserved only between C. jejuni and C. coli, indicating a close relationship between these two species.
Similar studies have investigated the genes responsible for motility in Campylobacter species. All Campylobacter species contain two flagellin genes in tandem for motility, flaA and flaB. These genes undergo intergenic recombination, further contributing to their virulence.
There is a growing number of quinolone resistant strains. Evidence suggests this is caused by an overuse of this class of antibiotics in animal agriculture .
Bacteriophage
The confusing taxonomy of Campylobacter over the past decades make it difficult to identify the earliest reports of Campylobacter bacteriophages. Bacteriophages specific to the species now known as C. coli and C. fetus (previously Vibrio coli and V. fetus), were isolated from cattle and pigs during the 1960s.
Pathogenesis
Campylobacter can cause a gastrointestinal infection called campylobacteriosis. The incubation period is 24-72 hours after infection . This is characterized by inflammatory, sometimes bloody diarrhea or dysentery syndrome, mostly including cramps, fever, and pain. The most common routes of transmission are fecal-oral, ingestion of contaminated food or water, and the eating of raw meat. Foods implicated in campylobacteriosis include raw or under-cooked poultry, raw dairy products, and contaminated produce. Campylobacter is sensitive to the stomach's normal production of hydrochloric acid: as a result, the infectious dose is relatively high, and the bacteria rarely cause illness when a person is exposed to less 10,000 organisms. Nevertheless, people taking antacid medication (e. g. people with gastritis or stomach ulcers) are at higher risk of contracting disease from a smaller amount of organisms, since this type of medication inhibits normal gastric acid. The infection is usually self-limiting and, in most cases, symptomatic treatment by liquid and electrolyte replacement is enough in human infections. Symptoms typically last five to seven days. Treatment with antibiotics has little effect and is discouraged except in high-risk patients.
The sites of tissue injury include the jejunum, the ileum, and the colon. Most strains of C jejuni produce a toxin (cytolethal distending toxin) that hinders the cells from dividing and activating the immune system. This helps the bacteria to evade the immune system and survive for a limited time in the cells. A cholera-like enterotoxin was once thought to be also made, but this appears not to be the case. The organism produces diffuse, bloody, edematous, and exudative enteritis. Although rarely has the infection been considered a cause of hemolytic uremic syndrome and thrombotic thrombocytopenic purpura, no unequivocal case reports exist. In some cases, a Campylobacter infection can be the underlying cause of Guillain–Barré syndrome. Gastrointestinal perforation is a rare complication of ileal infection.
Campylobacter has also been associated with periodontitis.
Treatment
Diagnosis of campylobacteriosis is made by testing a specimen of feces. Standard treatment is azithromycin, a macrolide antibiotic, especially for Campylobacter infections in children, although other antibiotics, such as macrolides, quinolones, and tetracycline are sometimes used to treat gastrointestinal Campylobacter infections in adults. In case of systemic infections, other bactericidal antibiotics are used, such as ampicillin, amoxicillin/clavulanic acid, or aminoglycosides. Fluoroquinolone antibiotics, such as ciprofloxacin or levofloxacin, may no longer be effective in some cases due to resistance. In addition to antibiotics, dehydrated children may require intravenous fluid treatment in a hospital.
UK
In January 2013, the UK's Food Standards Agency warned that two-thirds of all raw chicken bought from UK shops was contaminated with Campylobacter, affecting an estimated half a million people annually and killing about 100. In June 2014, the Food Standards Agency started a campaign against washing raw chicken, as washing can spread germs by splashing. In May 2015, cumulative results for samples taken from fresh chickens between February 2014 and February 2015 were published by the FSA and showed 73% of chickens tested positive for the presence of Campylobacter.
USA
Campylobacter infections increased 14% in the United States in 2012 compared to the period from 2006 to 2008. This represents the highest reported number of infections since 2000.
High prevalence of Campylobacter (40% or more) has been reported in raw chicken meat in retail stores in the USA. The reported prevalence in retail chicken meat is higher than the reported prevalence by the microbiology performance standard testing collected by the U. S. Department of Agriculture, and the last quarterly progress report on Salmonella and Campylobacter testing of meat and poultry for July–September 2014, published by the Food Safety and Inspection Service of the U. S. Department of Agriculture, shows a low prevalence of Campylobacter spp. in ground chicken meat, but a larger prevalence (20%) in mechanically separated chicken meat (which is sold only for further processing).
Canada
FoodNet Canada has reported that Campylobacter was the most common pathogen found on packaged chicken breast, with nearly half of all samples testing positive. Additionally, Campylobacter and Salmonella were the most common causes of gastrointestinal illness in Canada
New Zealand
In August 2016, an estimated 4,000+ residents of Havelock North, a town with 13,000 or so residents, had gastric illness after the water supply was thought to be contaminated by Campylobacter.
