Specialty gastroenterology ICD-9-CM 566 MedlinePlus 001519 | ICD-10 K61.0 DiseasesDB 32048 eMedicine med/2733 emerg/494 | |
 | ||
Anorectal abscess (also known as an anal/rectal abscess, or perianal/perirectal abscess) is an abscess adjacent to the anus. It arises from an infection at one of the anal sinuses which leads to inflammation and abscess formation. Most cases of perianal abscesses are sporadic, though there are certain situations which elevate the risk for developing the disease, such as diabetes mellitus, Crohn's disease, chronic steroid treatment and others. Ischiorectal, inter- and intrasphincteric abscesses have been described.
Contents
Classification
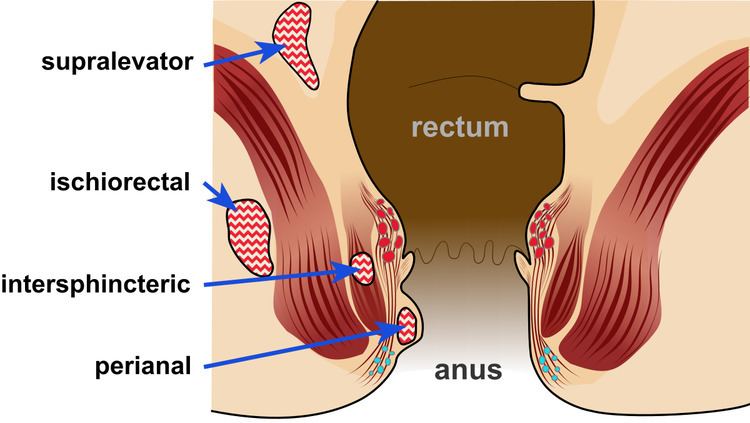
There are four types of anorectal abscesses: perianal, ischiorectal, intersphincteric, and supralevator.
Signs and symptoms
Pain in the perianal area is the most common symptom of an anorectal abscess. The pain may be dull, aching, or throbbing. It is worst when the person sits down and right before a bowel movement. After the individual has a bowel movement, the pain usually lessens. Other signs and symptoms of anorectal abscess include constipation, drainage from the rectum, fever and chills, or a palpable mass near the anus. The condition invariably becomes extremely painful, and usually worsens over the course of just a few days. The pain may be limited and sporadic at first, but invariably worsens to a constant pain which can become very severe when body position is changed (e.g., when standing up, rolling over, and so forth). Depending upon the exact location of the abscess, there can also be excruciating pain during bowel movements, though this is not always the case. This condition may occur in isolation, but is frequently indicative of another underlying disorder, such as Crohn's disease.
Differential diagnosis
This condition is often misdiagnosed initially by the patient as a bad case of hemorrhoids, since this is almost always the cause of any sudden anal discomfort. The presence of the abscess, however, is to be suspected when the pain quickly worsens over one or two days and the usual hemorrhoid treatments are ineffective in bringing relief. Furthermore, any serious abscess will eventually begin to cause signs and symptoms of general infection, including fever and nighttime chills.
A physician can rule out a hemorrhoid with a simple visual inspection, and usually appreciate an abscess by touch.
Cause
Abscesses are caused by a high-density infection of (usually) common bacteria which collect in one place or another for any variety of reasons. Anal abscesses, without treatment, are likely to spread and affect other parts of the body, particularly the groin and rectal lumen. All abscesses can progress to serious generalized infections requiring lengthy hospitalizations if not treated.
Historically, many rectal abscesses are caused by bacteria common in the digestive system, such as E. coli. While this still continues often to be the case, there has recently been an uptick in the causative organism being staphylococcus, as well as the difficult to treat community-acquired methicillin-resistant S. aureus. Because of the increasing appearance of more exotic bacteria in anal abscesses, microbiological examination will always be performed on the surgical exudate to determine the proper course of any antibiotic treatment.
Diagnostic approach
Diagnosis of anorectal abscess begins with a medical history and physical exam. Imaging studies which can help determine the diagnosis in cases of a deep non-palpable perirectal abscess include pelvic CT scan, MRI or trans-rectal ultrasound. These studies are not necessary, though, in cases which the diagnosis can be made upon physical exam.
Treatment
Anal abscesses are rarely treated with a simple course of antibiotics. In almost all cases surgery will need to take place to remove the abscess. Treatment is possible in an emergency room under local anesthesia, but it is highly preferred to be formally admitted to a hospital and to have the surgery performed in an operating room under general anesthesia.
Generally speaking, a fairly small but deep incision is performed close to the root of the abscess. The surgeon will allow the abscess to drain its exudate and attempt to discover any other related lesions in the area. This is one of the most basic types of surgery, and is usually performed in less than thirty minutes by the anal surgical team. Generally, a portion of the exudate is sent for microbiological analysis to determine the type of infecting bacteria. The incision is not closed (stitched), as the damaged tissues must heal from the inside toward the skin over a period of time.
The patient is often sent home within twenty-four hours of the surgery, and may be instructed to perform several 'sitz baths' per day, whereby a small basin (which usually fits over a toilet) is filled with warm water (and possibly, salts) and the affected area is soaked for a period of time. Another method of recovery involves the use of surgical packing, which is initially inserted by the surgical team, with redressing generally performed by hospital staff or a District Nurse (however, following the results of several double-blind studies, the effectiveness of surgical packing has come into question). During the week following the surgery, many patients will have some form of antibiotic therapy, along with some form of pain management therapy, consistent with the nature of the abscess.
The patient usually experiences an almost complete relief of the severe pain associated to his/her abscess upon waking from anesthesia; the pain associated with the opening and draining incision during the post-operative period is often mild in comparison. This is very often not the case however. Many patients will be in significant pain in the weeks and months after surgery.
Complications
If left untreated, an anal fistula will almost certainly form, connecting the rectum to the skin. This requires more intensive surgery. Furthermore, any untreated abscess may (and most likely will) continue to expand, eventually becoming a serious systemic infection.
