Specialty urology ICD-9-CM 607.85 DiseasesDB 29308 | ICD-10 N48.6 OMIM 171000 MedlinePlus 001278 | |
 | ||
Peyronie's disease or Peyronie disease (/peɪroʊˈniː/), also known as induratio penis plastica (IPP) or chronic inflammation of the tunica albuginea (CITA), is a connective tissue disorder involving the growth of fibrous plaques in the soft tissue of the penis affecting an estimated 5% of men. Specifically, scar tissue forms in the tunica albuginea, the thick sheath of tissue surrounding the corpora cavernosa causing pain, abnormal curvature, erectile dysfunction, indentation, loss of girth and shortening. A variety of treatments have been used, but none have been especially effective.
Contents
Signs and symptoms
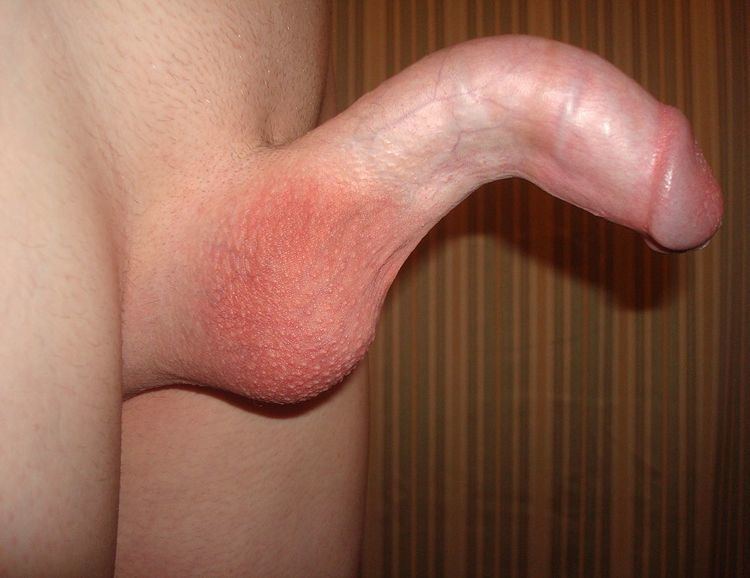
thumb|Penis with bend caused by Peyronie's disease.
A certain degree of curvature of the penis is considered normal, as many men are born with this benign condition, commonly referred to as congenital curvature.
The disease may cause pain; hardened, big, cord-like lesions (scar tissue known as "plaques"); or abnormal curvature of the penis when erect due to chronic inflammation of the tunica albuginea (CITA). Although the popular conception of Peyronie's Disease is that it always involves curvature of the penis, the scar tissue sometimes causes divots or indentations rather than curvature. The condition may also make sexual intercourse painful and/or difficult, though it is unclear whether some men report satisfactory or unsatisfactory intercourse in spite of the disorder. Although it can affect men of any race and age. The disorder is confined to the penis, although a substantial number of men with Peyronie's exhibit concurrent connective tissue disorders in the hand, and to a lesser degree, in the feet. About 30 percent of men with Peyronie's Disease develop fibrosis in other elastic tissues of the body, such as on the hand or foot, including Dupuytren's contracture of the hand. An increased incidence in genetically related males suggests a genetic component.
Diagnosis
A urologist may be able to diagnose the disease and suggest treatment. An ultrasound can provide conclusive evidence of Peyronie's disease, ruling out congenital curvature or other disorders.
Causes
The underlying cause of Peyronie's Disease is not well understood, but is thought to be caused by trauma or injury to the penis usually through sexual intercourse or physical activity although many patients often are unaware of any traumatic event or injury.
Some beta blocker drugs list Peyronie's disease as a possible side effect.
Treatment
Without treatment, about 12–13% of patients will spontaneously improve over time, 40–50% will get worse and the rest will be relatively stable. This is based on a survey of 97 men and therefore based on the subjective impression of the patients. No objective long term natural history via continual evaluation of patients has been recorded to date.
Medication and supplements
Many oral treatments have been studied, but results so far have been mixed. Some consider the use of non-surgical approaches to be "controversial".
Collagenase clostridium histolyticum (marketed as Xiaflex by [Auxilium]), a drug originally approved by the FDA to treat Dupuytren's contracture, is now an FDA approved injectable drug for treatment of Peyronie's disease. The drug is reported to work by breaking down the excess collagen in the penis that causes Peyronie's disease.
Vitamin E supplementation has been studied for decades, and some success has been reported in older trials, but those successes have not been reliably repeated in larger, newer studies. A combination of Vitamin E and colchicine has shown some promise in delaying progression of the condition.
Some newer agents targeting the basic mechanisms of inflammation have been studied in larger clinical trials. These include potassium para-aminobenzoate (Potaba), pentoxifylline (acting through TGFβ1 inhibition), and Coenzyme Q10.
The efficacy of Interferon-alpha-2b in the early stages of the disease has been reported in recent publications but it was found to be less effective in cases where calcification of the plaque had occurred in common with many treatments.
Formulations of superoxide dismutase are also reported to be effective in Peyronie's disease.
Injections to plaques (scar tissue formed by the inflammation) with Verapamil may be effective in some patients, but a recent placebo controlled trial failed to show a significant improvement. Use of iontophoresis with Verapamil and Dexamethasone, applied to the affected areas, has been studied.
Surgery
Surgery, such as the "Nesbit operation", (which is named after Reed M. Nesbit (1898–1979), an American Urologist at University of Michigan) is considered a last resort and should only be performed by highly skilled urological surgeons knowledgeable in specialized corrective surgical techniques. A penile prosthesis may be appropriate in advanced cases.
Physical therapy and devices
Penile traction therapy may be an effective treatment but the treatment course is difficult.
Counseling
Peyronie's Disease can be a physically and psychologically devastating disease. While most men will continue to be able to have sexual relations, they are likely to experience some degree of deformity and erectile dysfunction in the wake of the disease process. It is not uncommon for men afflicted with Peyronie's Disease to exhibit depression or withdrawal from their sexual partners.
