ICD-10 Xxx.x | ICD-9-CM xxx | |
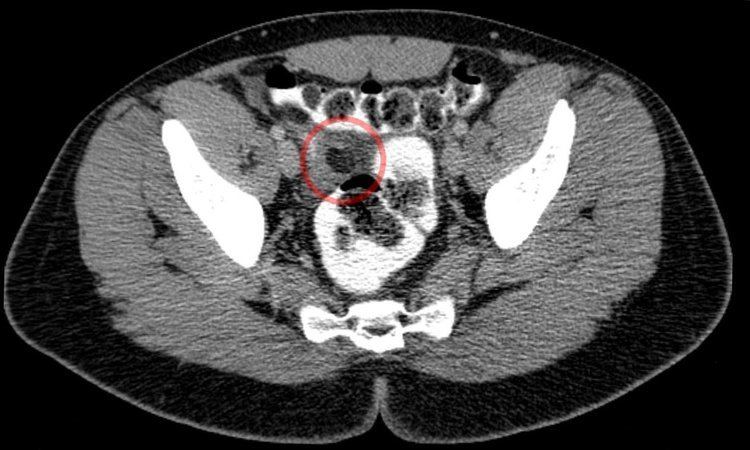 | ||
Epiploic appendagitis (EA) is an uncommon, benign, non-surgical, self-limiting inflammatory process of the epiploic appendices. Other, older terms for the process include appendicitis epiploica and appendagitis, but these terms are used less now in order to avoid confusion with acute appendicitis.
Epiploic appendices are small, fat-filled sacs or finger-like projections along the surface of the upper and lower colon and rectum. They may become acutely inflamed as a result of torsion (twisting) or venous thrombosis. The inflammation causes pain, often described as sharp or stabbing, located on the left, right, or central regions of the abdomen. There is sometimes nausea and vomiting. The symptoms may mimic those of acute appendicitis, diverticulitis, or cholecystitis. The pain is characteristically intense during/after defecation or micturition (espec. in the segmoid type) due to the effect of traction on the pedicle of the lesion caused by straining and emptying of the bowel and bladder. Initial lab studies are usually normal. EA is usually diagnosed incidentally on CT scan which is performed to exclude more serious conditions.
Although it is self-limiting, epiploic appendagitis can cause severe pain and discomfort. It is usually thought to be best treated with an anti-inflammatory and a moderate to severe pain medication (depending on the case) as needed. Surgery is not recommended in nearly all cases. Sand and colleagues, however, recommend laparascopic surgery to excise the inflamed appendage in most cases in order to prevent recurrence.
